Case Study
History
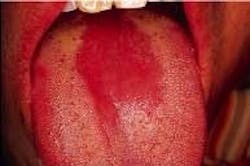
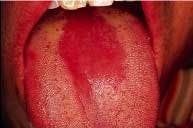
The patient was aware of the red patch on his tongue and claimed it had been present for several weeks. No pain, burning, or sensitivity was noted in the affected area. The patient also reported the lesion had not appeared to increase or decrease in size. The patient appeared to be in an overall good state of health. No health problems were noted, and the patient was not taking medications at the time of the dental examination. The patient's dental history included regular examinations and routine treatment.
Examinations
The patient's vital signs were all found to be within normal limits. Examination of the head and neck region revealed no enlarged or palpable lymph nodes. Extraoral examination revealed no significant or unusual findings. Intraoral examination revealed a large red patch on the posterior dorsal tongue (see photo). The affected area appeared to lack the normal keratotic white filiform papillae. Further oral examination revealed no other lesions present.
Clinical diagnosis
Based on the clinical information available, which one of the following is the most likely diagnosis?
- allergic reaction
- vitamin deficiency
- median rhomboid glossitis
- thermal injury
- geographic tongue
- median rhomboid glossitis
Discussion
Median rhomboid glossitis (also known as central papillary atrophy) appears as a red patch on the dorsal tongue. The term median indicates the location of this lesion - at the midline of the tongue. The term rhomboid refers to the shape of the lesion, and the term glossitis refers to the fact that it looks like an inflammation (-itis) of the tongue.
In the past, this lesion was believed to be a developmental defect of the tongue. It was previously presumed to be an embryologic failure of the tuberculum impar to retract or withdraw before the fusion of the lateral processes of the tongue, resulting in an area of the tongue devoid of papillae. The developmental origin of this lesion was later discounted when investigators discovered that this abnormality was extremely rare in children. This lesion is no longer considered developmental, because the vast majority of cases are seen in adults; if the lesion were truly developmental, it would occur with equal frequency in both children and adults.
Clinical features
Current evidence suggests that this lesion is actually a localized, chronic fungal infection known as erythematous or atrophic candidiasis. Erythematous candidiasis is one of the forms of oral candidiasis. Oral candidiasis is a superficial mucosal infection caused by the yeast-like fungus, Candida albicans.
As the name erythematous suggests, this form of candidiasis has a characteristic red appearance. It is found on the dorsal surface of the tongue, at the midline, and anterior to the circumvallate papillae. In the affected area, a total loss of papillae is seen; the area appears red due in part of the loss of filiform papillae.
The lesion is usually symmetric and may be ovoid-, diamond-, or rhomboid-shaped. The lesion may appear flat and smooth or lobulated. This lesion is usually asymptomatic and discovered during routine oral examination.
Diagnosis and treatment
Median rhomboid glossitis/erythematous candidiasis can be diagnosed using culture or cytologic examination techniques. A positive culture exhibits dome-shaped, creamy white colonies of Candida albicans on the surface of Sabouraud's agar after the incubation at room temperature for two to three days. A positive cytologic preparation exhibits fungal hyphae, characteristic of Candida albicans.
Once the diagnosis has been established, systemic or topical antifungal agents can be used to treat this lesion. The mucosal alteration resolves with antifungal therapy, although in some long-term cases, only partial resolution may be achieved. In addition, predisposing factors (smoking, wearing dentures, immune deficiencies, antibiotic use, corticosteriod use, etc.) for candidiasis must also be identified and corrected.
Joen Iannucci Haring, DDS, MS, is an associate professor of clinical dentistry, Section of Primary Care, The Ohio State University College of Dentistry.