Case Study
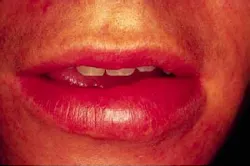
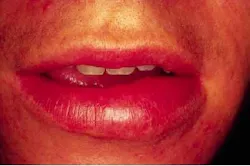
A 26-year-old male presented to the dental office for a routine check-up. At the time of the appointment, a diffuse swelling of the lower lip was noted.
History
When questioned about the swollen lower lip, the patient stated that it had first appeared several days earlier. The patient admitted to a history of previous episodes varying in duration from hours to weeks. The patient described the area as painless and denied any history of injury to the area. The patient's last dental visit had taken place one year earlier. At the time of the dental appointment, the patient appeared to be in an overall good state of health.
Examinations
The patient's vital signs were all found to be within normal limits. Extraoral examination revealed a diffuse nontender enlargement of the lower lip (see photo). No evidence of erosion or ulceration was noted. Further extraoral examination revealed no other areas of swelling present. No unusual or abnormal intraoral findings were noted.
Clinical diagnosis
Based on the clinical information presented, which one of the following is the most likely clinical diagnosis?
- nasolabial cyst
- angioedema
- cheilitis glandularis
- cheilitis granulomatosa
- factitious cheilitis
Diagnosis
- cheilitis granulomatosa
Discussion
Orofacial granulomatosis is a condition that involves the granulomatous inflammation and enlargement of tissues in the oral and facial regions. In cases where only the lips are involved, the condition is known as cheilitis granulomatosa. The cause of cheilitis granulomatosa is unclear. This disorder is currently believed to be an abnormal autoimmune reaction, either primary or secondary. Suggested precipitating factors include a genetic predisposition, infections (such as bacterial, viral, or odontogenic), or allergic reactions to food or other materials.
Clinical features
Cheilitis granulomatosa presents as a diffuse firm and nontender swelling of the lips. The swelling is firm and nontender. Although both lips may be involved, the lower lip is affected more often. The diffuse enlargement of the lip does not affect the lip color. Recurring episodes of cheilitis granulomatosa are common and may last from hours to months at a time, some may result in permanent enlargement.
Diagnosis
The diagnosis of cheilitis granulomatosa involves the exclusion of potential systemic granulomatous processes that have oral or facial involvement. Systemic diseases such as Crohn's disease, hairy cell leukemia, tuberculosis, sarcoidosis, and chronic granulomatous disease must be ruled out. A biopsy is required to rule out a foreign body or infection. If an allergic response is suspected as a precipitating factor, patch testing and elimination diets may be used to confirm the probable cause.
Treatment
Treatment for cheilitis granulomatosa is often disappointing. Intralesional injections of corticosteroid preparations often are used, but with limited success. Systemic corticosteroid medications also may be used. Some patients respond to the elimination of the suspected precipitating factor or management of the underlying systemic disease. In individuals that do not respond to therapies, surgical recontouring has been used; however, there is a considerable risk of recurrence.
Joen Iannucci Haring, DDS, MS, is an associate professor of clinical dentistry, Section of Primary Care, The Ohio State University College of Dentistry.