Readers’ Forum
Dear RDH:
I was compelled to write after reading “Storm Clouds over Florida” in the April 2007 issue, which spoke of foreign-trained dentists taking over RDH jobs. I have been a hygienist for 27 years. I am a U.S. citizen and worked very hard to obtain my licensure in the state of Florida, because I had to retake my board exams there, after working for many years in other states.
I recently went on a job interview where they were looking for a part-time hygienist and a full-time hygienist. The full-time position had many benefits that the part-time position didn’t have, including health insurance, which I needed badly because I am a diabetic. My COBRA had recently ended, and no other insurance company would pick me up. I could not afford my diabetic medications. I was between jobs and had two kids to raise by myself.
Needless to say, I was in quite a desperate situation, and needed a full-time position with benefits badly. I interviewed and was hired for the part-time position.
I did not get the full-time position. A girl from China got it because she was a dentist and, according to my boss, better qualified than me. She had just moved here, could barely speak English, and her husband was a professor at the nearby university which included full benefits.
I was so mad that steam was coming out of the top of my head. What gives these foreigners the right to come to this country and take jobs away from Americans who really need them? I know this is a free country, but it just seems unfair and unjust. I worked there for a little while, and she tried to tell me how to do my job. She thought she was much more qualified than me as a hygienist, just because she was a dentist.
Anyway, I finally did land a full-time position with benefits and my boss is a true gem. I thank my lucky stars every day because I finally found a job that I will never leave and with a boss that truly appreciates me and my expertise!
Debra A. Miller, RDH
Gainesville, Florida
Dear RDH:
Reading the May 2007 issue of RDH magazine had to have been the highlight of my day today. I thoroughly enjoyed the issue, but one article made me really reflect on my life experiences. While growing up, being a Jewish child in a predominantly non-Jewish city in Connecticut was a difficult challenge for many of us. I came from a very open-minded family and knew all walks of life (it was never surprising for me to see a meeting of the NAACP or the ADL in my home when walking in from school). I encountered many different cultures during my daily living activities.
But I vividly recall one day in middle school when I was confronted by an Italian “friend.” She was angry with me about something and proceeded to call me a most derogatory name, which I had never heard before. When I went home, being inquisitive as I was and still am, I looked the word up in the dictionary. My dad happened upon me as I was doing this and he was shocked to hear what word I was looking up.
He proceeded to explain the term to me in very clear language and told me how derogatory it was and wanted to know where I heard it. Knowing that I could not lie to my parents I told him who used it and how it was used. Much to my embarrassment at the time, he got in touch with her parents and had quite a talk with them and their daughter. How she and I survived that I still don’t know, but it did show the importance of “cultural differences” and how we must respect one another so much, accepting people for who they are.
Recently, at a board review I experienced a similar incident in which a student used a very derogatory term toward a lovely black employee of the college where I was teaching. The employee reported the incident to campus security, and the student was placed on suspension and had to take several courses, one being intercultural differences.
This only proves that what Toni Adams has to say is true (Finding our footing in the ocean, page 29). As health-care professionals, we must respect and understand intercultural differences. We cannot judge people for ignorance when they have not been taught. We must be able to encourage good health care to the underserved and understand how to enlighten them without insulting them. These courses are absolutely a must.
I really must be naïve, though, since I grew up so integrated with so many cultures that race, different value systems, different levels of education, etc., never even bothered me nor allowed me to judge others. I accept people for who they are and treat each accordingly with the same level of respect that I expect to receive.
Never did I think that I would see (especially from a health-care provider or a potential one) the lack of respect for another person regardless of race or creed and there it was, staring me in the face. Thank you, Toni, for making the profession aware of the need for these type of courses and for imploring us to understand the cultural differences so that we might treat all people equally and provide adequate health care for all.
Jane Weiner, RDH
Tamarac, Florida
Dear RDH:
As a follow-up to the informative articles about Xylitol and its virtues that we have all read, and my letter addressing one concern in the May 2007 issue, perhaps the subject of toxicity to dogs should be raised.
All of us should warn our patients, when we recommend Xylitol products, that the substance can very quickly be lethal to dogs, should they ingest it. Severe hypoglycemia with liver damage or failure (especially in small dogs) is the result with even a couple of pieces of Xylitol-containing chewing gum.
The more information we have at our fingertips, the better!
Amy Brown, RDH, BS, EDH
Leawood, Kansas
Dear RDH:
The article, “Researching essential oils,” by Cathy Hester Seckman, RDH, contains a tremendous amount of misinformation, some of it dangerous. First, there is no “cherry essential oil.” Fruits (other than citrus) do not yield essential oils, so whatever fragrance is being tested, it is synthetic, thus not aromatherapy.
She also states, “...but the usual dose of essential oils for adults is 1 to 4 ml three times daily.” That is frightening. First, it suggests internal dosage, which in those quantities could be dangerous. Secondly, application of essential oils is normally measured by drops, not milliliters. In a bath, for example, we normally use perhaps eight to 10 drops.
The description of chamomile is taken from herbal use, not necessarily applicable to essential oils. At least one of the oils suggested for relaxation (peppermint) is a stimulant, not a sedative.
Those of us who have experienced the healing power of true essential oils love to see it discussed (see www.naturesgift.com), but we also suggest safe and appropriate usage.
My dentist diffuses a blend of essential oils designed to reduce anxiety in his treatment rooms. He says it makes a marked improvement in the emotional condition of some patients. I have seen case studies showing a total lack of swelling and bruising after multiple extractions with the use of ice and topically applied aromatherapy products. It does work and does have application to dental practice, just not in the manner suggested in this article.
Marge Clark, RDH
Madison, Virginia
Editor’s Note:
Ms. Seckman was a guest columnist for the “Mind, Body & Spirit” column. She said in her opening paragraph that she wanted to “explore the world of essential oils from the perspective of a neophyte.” So she reviewed the literature regarding clinical trials on essential oils. Seckman said Ms. Clark’s “comments highlight what I see as significant problems with the field of aromatherapy - a lack of hard science and controlled vocabulary.”
“I’m sure I did confuse fruit oils, herbal oils, and essential oils, but so do the researchers who use the terms interchangeably. Thank you for your comments. I should have been more careful in reading research, and should have realized the vocabulary isn’t standardized.”
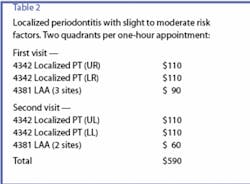
Correction
The chart above appeared in the June 2007 issue. The article, which was titled, "Confusion About Codes," offered the information in the chart as a suggestion for a treatment process, but it unfortunately repeated on quadrant. The chart, as it now stands, is correct. We regret any confusion.