Skin cancer screening: A dental hygienist's life-saving responsibility
“Necessity is the mother of invention” is the well-known proverb. It’s also the concept that led to the modern-day invention of sunscreen and what we now know as sun protection factor (SPF). Austrian chemist Franz Greiter is credited with inventing the first sunscreen in 1938, after suffering a sunburn while climbing Mount Piz Buin, a mountain in the Silvretta range of the Alps on the border between Austria and Switzerland.1 His was the first commercial sunscreen in the United States, and in the 1960s he established SPF ratings.1 He’s also recognized as developing the first sunscreen to protect against ultraviolet A (UVA) and ultraviolet B (UVB) light.1 Growing up in the ’60s and ’70s as I did, we didn’t wear sunscreen, baby oil was queen, and so was the bronzed look that took hours of “laying out in the sun” to achieve. It was cool to be tan. That attitude explains much of the situation we’re in today with skin cancer.
According to the Skin Cancer Foundation:2
- Skin cancer is the most common cancer in the United States and worldwide.
- One in five Americans will develop skin cancer before the age of 70.
- More than two people die of skin cancer in the US every hour.
- Having five or more sunburns doubles your risk for melanoma.
Personally, I can recall having more than five sunburns in the course of several years. Where does your risk, your family’s risk, and your patients’ risk fall?
As dental hygienists, we are optimally positioned to evaluate for skin abnormalities of the head and neck, face, ears, scalp, hairline, nose, and eyes, when performing our visual and tactile, intraoral and extraoral evaluation. While we are not equipped to diagnose skin cancer, we can and should use our assessment and evaluation skills to identify any abnormalities and talk with patients about seeing a dermatologist for further investigation. Early referral leads to early diagnosis, after all.
Types of skin cancer3
What are the types of skin cancer we as dental hygienists should be aware of when screening?
Basal cell carcinoma (BCC) is the most common type of skin cancer. “BCC often looks like a flesh-colored round growth, pearl-like bump, or a pinkish patch of skin.”3 While a BCC can appear anywhere on the body, it is commonly found on the head, neck, and arms. Because a basal cell carcinoma grows deep, can infiltrate bones and nerves, and can result in disfigurement and damage to anatomical structures locally, early detection is vital.
Squamous cell carcinoma (SCC) of the skin is the second most common type of skin cancer. “SCC often looks like a red firm bump, scaly patch, or a sore that heals and then reopens.”3 SCC will commonly occur on areas of the body that have more sun exposure, the face, neck, rim of the ear, chest, arms, and back. Like BCC, SCC can grow deep into local structures, resulting in disfigurement and damage. SCC of the skin can metastasize to other areas of the body, making early detection very important. An actinic keratosis is a precancerous growth that has potential to turn into SCC, and may appear as a dry, scaly spot or patch on the skin.
Melanoma is known as the deadliest form of skin cancer since it tends to metastasize, making early detection and treatment critical. It often appears in an existing mole or as a new dark spot on the skin.
Being familiar with the ABCDEs4 of melanoma will help dental hygienists assess patients and encourage them to see a dermatologist for early diagnosis when necessary.
A is for asymmetry. One half of the spot is different from the other half.
B is for border. The border of the spot is irregular, poorly defined, or scalloped.
C is for color. The spot has varying colors of tan, brown, black, red, or areas of white, red, or blue.
D is for diameter. “While melanomas are usually greater than six millimeters, or about the size of a pencil eraser, when diagnosed they can be smaller.”
E is for evolving. “The spot looks different from the rest or is changing in size, shape, or color.”
The American Academy of Dermatology has a downloadable infographic at aad.org/public/diseases/skin-cancer/how-to-spot-skin-cancer.
Who is at risk?
The Skin Cancer Foundation reports the following risk factors:5
- Indoor tanning. The risk of developing melanoma increases by 75% after one use of indoor tanning before the age of 35.
- Sunburn. A sunburn is an inflammatory response to UV radiation/UV damage to the outer layers of the skin. UV exposure increases skin cancer risk even before a burn.
- Skin type. Fair skin is more at risk for skin cancer, including melanoma.
- Prolonged exposure to UV radiation. UVA is associated with aging, while UVB is associated with sunburns. They both do harm by damaging DNA in skin cells.
- Genetics and red hair. Patients with a family history of skin cancer or who have naturally red hair are at increased risk.
- Atypical moles. See the ABCDEs of melanoma; having 10 or more atypical moles increases the risk of melanoma by 12 times.
- Organ transplant. The risk of developing SCC is approximately 100 times higher and the risk of developing BCC is approximately six times higher after transplantation, when compared to the general population.
The American Academy of Dermatology (AAD) offers these additional risk factors:6 blond hair; immune system suppressing diseases or treatments; a history of skin cancer; females age 15–29; men over 50; and Caucasian ethnicity.
The perception exists that people of color are not at risk for skin cancer. While skin cancers are less prevalent in nonwhite racial ethnic groups, when they do occur the outcome tends to be much worse.7 The Skin Cancer Foundation reports that this may be because people of color believe they aren’t at risk, and so receive fewer full-body screenings for skin abnormalities. Also, people of color tend to develop skin cancer on areas of the body that are exposed to the sun to a lessor degree. Melanoma is most common in people of color in the lower extremities, especially the soles of the feet. It is important to note that the Skin Cancer Foundation also reports, “In melanomas on the whole, UV radiation is certainly a major risk factor, and we see plenty of UV-induced melanomas and squamous cell carcinomas in people of color, who can have a wide range of complexions, from very fair to very dark.”7
Dental hygienists’ role
What’s our role, and how can we “promote high standards of quality care … and uphold the highest standards of professional competence” as the dental hygiene oath states?8 The American Dental Hygienists’ Association “supports a comprehensive screening for oral cancer, oropharyngeal cancer, and any abnormality for all patients to achieve earliest referral for diagnosis.”9 As dental hygienists, while performing extraoral evaluations, we are optimally positioned to evaluate for skin abnormalities using our loupes and lighting. We should make a habit of asking patients about any history of sunburns and if they are using a sunscreen with an SPF of 30 or higher as recommended by the AAD.5 It’s also good practice to ask patients about personal or family history of skin cancer, current or past use of indoor tanning, history of organ transplant, and if the patient is immunocompromised in any way. Regarding patients of color, discuss their risk and encourage regular skin cancer evaluations. Keep in mind the phrase I often use when consulting using the Cotten Method, “If it’s not right, it’s wrong; react and refer.”
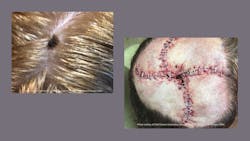
As with most things, my passion for this topic comes from life experience. After three major skin cancer surgeries (Mohs) in the last 26 years to remove BCCs from my nose—one that even invaded the rim of my nose and resulted in reconstruction—it is my mission to help others prevent skin cancer and to encourage dental hygienists to be advocates for early detection.
References
- Ross M. Coppertone owes its success to a pharmacist. Pharmacy Times. June 2, 2015. https://www.pharmacytimes.com/view/coppertone-owes-its-success-to-a-pharmacist
- Skin cancer facts & statistics. Skin Cancer Foundation. Updated January 13, 2021. https://www.skincancer.org/skin-cancer-information/skin-cancer-facts/
- Types of skin cancer. American Academy of Dermatology Association. https://www.aad.org/public/diseases/skin-cancer/types/common
- What to look for: ABCDEs of melanoma. American Academy of Dermatology Association. https://www.aad.org/public/diseases/skin-cancer/find/at-risk/abcdes
- Risk factors. Skin Cancer Foundation. https://www.skincancer.org/risk-factors/
- Skin cancer facts PDF. American Academy of Dermatology. https://assets.ctfassets.net/1ny4yoiyrqia/2Mib7sdsmxQaxS9gPcTqbm/a16298acaff8112aac5e21ed43cb40d8/skin-cancer-facts.pdf
- Ask the expert: Is there a skin cancer crisis in people of color? Skin Cancer Foundation. July 5, 2020. https://www.skincancer.org/blog/ask-the-expert-is-there-a-skin-cancer- crisis-in-people-of-color/
- Cruz N. Ethics and law in dental hygiene slideshow. https://slideplayer.com/slide/5786345/
- ADHA policy manual. American Dental Hygienists’ Association. Practice & Technology chapter (p. 19). June 2020. https://mymembership.adha.org/images/pdf/ADHA_Policy_Manual.pdf
SUSAN COTTEN, BS, RDH, OMT, is a passionate speaker, consultant, trainer, and subject-matter expert on HPV and the head and neck oral/oropharyngeal cancer evaluation. She is owner of Oral Cancer Consulting. Susan developed the “Cotten Method,” a comprehensive oral cancer office system which increases confidence in screening and aids in reducing liability. She is a 2018 recipient of the Sunstar/RDH Award of Distinction and 2020 Colorado Dental Hygienists’ Association Ethel Covington Award.
About the Author

Susan Cotten, BSDH, RDH, OMT
Susan Cotten, BSDH, RDH, OMT, is dentistry’s oral cancer coach, 2018 Sunstar/RDH Award of Distinction recipient, and developed The Cotten Method™ of Screening for oral, oropharyngeal cancer, and other head and neck concerns. With more than 30 years as an RDH, Susan provides in-office training, speaking, and hands-on workshops to deepen confidence in a comprehensive screening, reduce liability, and increase early detection. Determined to have a world Oral Cancer Free™, her course is available online through the National Network of Healthcare Hygienists. Reach her at [email protected].