Tongue chewing: Causes, treatments, and information for patients
Editor's note: Originally posted in 2013 and updated regularly
The patient examined was Coy, an 18-year-old college student. Coy has just finished his first year of college, was home for the summer, and was in for his yearly maintenance appointment. Coy presented as a healthy, athletic young adult who denied using alcohol or tobacco.
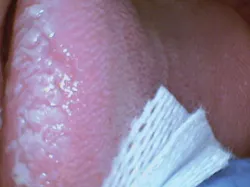
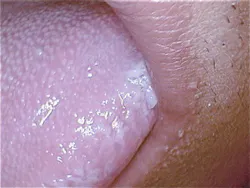
Coy had some white, raised, keratotic-appearing tissue on the lateral border of his tongue during the oral cancer exam. The thickened tissue was bilateral. When this came up with Coy, he said he'd been under a lot of stress with his exams in college. He was aware that he'd has been chewing on the sides of the tongue. He said that it had become a habit, and he wasn't able to stop chewing on his tongue. He tried to break the habit himself, but couldn't seem to disconnect the behavior.
Coy was asked whether he was this at night as well, and he said he didn't know. He did say that he felt a little tongue soreness when he woke up in the morning (see figures 1, 2).
Tongue chewing is certainly nothing new in this population, and dental practitioners find it on a regular basis. Varying states of tissue damage may be found clinically with both minor and extensive degrees of keratinization and pigmentation. The tissue responds to friction and becomes thickened in what is termed hyperkeratosis. As with other areas of tissue, wet tissue becomes whiter in color, just as the skin does when kept in water too long.
Also by Nancy W. Burkhart:
Lichen planus pemphigoides: An autoimmune blistering disease
The fibroma: Breaking a common habit
When found on the lateral borders of the tongue, morsicatio linguarum is a term often used, and morsicatio buccarum is used when the damage is found on the buccal mucosa. Additionally, morsicatio labiorum is used when the patient is chewing, biting, or placing pressure on the inner lip area. The tissue may appear abraded, ulcerative, or highly keratinized. As with any other injured tissue, such as a "cheek bite," the patient may continue to traumatize the area while chewing or speaking. As the tissue becomes more enlarged, the patient may traumatize it with normal mastication or speech.
Breaking the habit
Dental professionals can use several techniques to help patients in trying to overcome the habit and allow the tissue to heal. It is important to try to determine whether the patient is performing the habit while sleeping or during the day; in some cases, it could be both times of the day.
Some dentists and hygienists prefer to suggest a mouthguard that the patient wears day and night for a specified amount of time to help break the habit. Mouthguards are used for multiple reasons: protecting the tissues from constant trauma such as in athletics, eating disorders (protection of the teeth during purging episodes), bruxism, and other reasons.
With a patient first gets the guard, the patient may need some time to get accustomed to wearing ite, but the mouth guard may assist in relieving the tissue trauma. (See the suggestions for mouth guard use/patient instructions below).
Stress continues to be a byproduct of our fast-paced society. Stress is difficult to quantify, and each person will handle it in a different way. Some patients will be more successful long-term than others.
Below are some suggestions for dental professionals on assisting the patient who may be causing tissue damage in various areas of the mouth.
Treatment and prognosis
We usually are aware of stress factors when symptoms appear clinically with a patient. As the oral signs dissipate, we're able to tell if the protocol we have used is causing some reversal of damage. However, with some individuals, the evidence may reappear and we may need to repeat certain steps to work through the problem again. This is true for tongue chewing. As stress levels increase, the patient may resume the behavior and may need to take action to correct it again. Unless patients have take steps to adjust to a stressor and learn new coping strategies to deal with stress, the problem may be intermittent. Any chronic type of irritation is not a healthy state and may indicate underlying problems such as extreme stress or anxiety disorders. Finding the true source of the problem can help the patient manage their long-term health, in general. Any type of constant irritation should be taken seriously and chronic assault on the tissue may develop into more serious states such as dysplasia and frank carcinoma.
Information to share with patients about mouthguards
- The appliance should be either in your mouth or in the carrier case.
- Don't place it on a pile of papers! Since it's clear in color, it could get accidentally be thrown out.
- Keep it away from dogs—they're known to eat or chew mouth guards.
- Do not leave the appliance on your nightstand next to the bed. It may drop on the floor and be kicked under the bed.
- Never wrap it up and place the appliance in a paper napkin because the napkin, out of habit, could be thrown away along with your expensive appliance.
- Some people take the appliance out in their sleep and try to find it in the bedding later. Make a mental note that this should not occur. The appliance may accidentally be discarded or washed with the bed sheets in a harsh or bleach detergent.
The new mouthguard
- Do not place a new mouthguard in your mouth initially and try to fall asleep. Your mental processes will determine a foreign object is present, and it could affect your sleep patterns. You could end up chewing it and playing with it and ultimately taking the appliance out of the mouth.
- A new habit takes approximately 21 days to become part of your normal daily pattern. Be gentle and accepting with yourself in forming new habits.
- Our normal daily activities can be a good distraction from having a new appliance in the mouth.
a. Eat breakfast, brush and floss your teeth
b. Put your mouthguard in
c. Wear it all day, and only take it out when you eat
d. Don't eat with the appliance in your mouth
At lunchtime/throughout the day, cleaning the appliance:
- Brush the appliance with toothpaste and rinse with water just as you do with your teeth several times a day.
- While at work or school, run the appliance under cold water after meals. This will keep your breath feeling fresh and increase the likelihood that you will continue to wear the appliance.
- Brush the inside area that touches the tissue with a mild toothpaste, if possible. Several benefits occur with the cleanliness of any appliance. The appliance will feel fresh, and the amount of bacteria and candida will be decreased.
- Never place the appliance in any "bleach" solution.
- Do not place the appliance in mouthwash.
- Storage and transportation of the appliance should be in a vented container.
- Occasionally clean the mouthguard in warm soapy water and rinse thoroughly.
- Never leave the mouthguard in the sun or in hot water.
Dental appointments and follow-up
- Always bring the appliance with you to your dental visits for a thorough cleaning by the hygienist (usually in an ultrasonic cleaner) and the dentist can check the appliance for the fit.
- Write yourself a reminder in your calendar to bring it to your prophy/maintenance recall visit.
- In the beginning while wearing the appliance, please note that talking and speech may be affected and will take a few days for speech to resume to normal when the tongue compensates for the appliance. If you say the numbers 33, 34, 35, 64, 65, 66, the number 66 will often cause you to make a whistle-like sound.
- When the mouthguard is recommended for tongue chewing, intraoral images may be taken so that tissue comparison may be performed in future visits.
Long-term goals
After a set time, and with careful determination by the dental team, you may wish to stop using the appliance and determine whether the tongue chewing habit is broken. You should, however:
- Save the appliance in the carry case at a safe location.
- Never throw it away because it is very expensive to remake.
- The appliance will be good for years and could be worn in the future.
- A new appliance may be needed if any tears or roughness occur at any time.
Source: Modified from information given to patients for Mouthguard Maintenance by Carol Perkins, RDH, Pleasanton, CA. June 2013.
Clinical suggestions for morsicatio buccarum, morsicatio linguarum, or morsicatio labiorum
- First, show the patient the area of concern. Determine if the patient is aware of the morsicatio buccarum, morsicatio labiorum, or morsicatio linguarum. Give the patient a hand mirror and use the dental lighting to observe the area together.
- Try to determine whether the patient is chewing on the area at night, during the day, or at other specific times. Professionally produced night guards may be beneficial for patients who are performing the habit at night. Often, the patient may also exhibit evidence of bruxism as noted by tooth surface changes. Some shields can be fabricated and worn daily as well.
- If the patient is new, determine how long ago he or she has noticed the habit. If the tissue is being observed in a patient of record, review the history to determine if any notation is listed in prior visits. How long has it been documented? Chronic habits may take a long time to break.
- If it is determined to be a situational stress problem, suggest stress reduction techniques that may help the patient lower stressful situations. Additionally, forming new coping strategies is crucial in changing a chronic, negative habit and modifying the way that we react to stressors. Some helpful techniques may be exercise, prayer, meditation or other techniques such as biofeedback. Biofeedback will teach a person to use his or her breathing and focus to reduce stress. Personally, I like the hand-held, pocket size device called the EM-WAVE that can be carried by the person and is always available. The device and other relaxation products may be found at the Stens website.
- Most people with stress-related conditions are not aware they are stressed, and will tell you that they are no more stressed than anyone else. We all handle stress in different ways, and some techniques are better than others for each person. Ultimately, success depends upon the individual. The good news is: stress reduction can be learned and coping skills can be developed.
- In certain situations, the patient may have taken antianxiety medications and since discontinued those medications, leading to poor health habits. Suggesting that they contact their physician or see a counselor may be appropriate, depending on the person and the clinical signs. In today's society, many people are overwhelmed with everyday stress, and many dental or medical offices report an increase in the number of people who are diagnosed with morsicatio buccarum, morsicatio linguarum, morsicatio labiorum and bruxism.
- Use intraoral photography to document the areas of concern, and use the images for future comparison at maintenance visits.
- If the patient uses tobacco and/or alcohol, there is further concern related to future changes in the tissue and oral cancer. If the patient has not had an oral cancer screening, perform one or suggest a biopsy if there is any indication that the area of concern has the possibility of a malignancy. If changes occur or the habit continues, careful evaluation, referral, or future biopsy in some cases is always wise.
- Remind the patient that any irritation and inflammation in the body is detrimental to our health. Pathogens are able to enter the body and chronic inflammation places us at risk for other health-related disease states.
- Develop some techniques that will make the patient aware of the habit, including:
- Tying a ribbon, rubber band or string around the wrist, which is always helpful in behavior modification and used as a reminder to the person to check his or her own behavior.
- Placing strategically located stickers in the home and workplace to remind the person to check their progress.
- Finally, have the patient visualize the word "No" circled with an X through it. This step will help the person eliminate the habit through visualization.
Disclaimer: The author has no affiliation with the Stens Corp.
Modified from Delong L. & Burkhart N. "General and Oral Pathology for the Dental Hygienist." 2nd ed. Lippincott, Williams and Wilkins, Baltimore, 2013.
About the Author
Nancy W. Burkhart, EdD, MEd, BSDH, AAFAAOM
NANCY W. BURKHART, EdD, MEd, BSDH, AAFAAOM, is an adjunct professor in the Department of Periodontics-Stomatology, College of Dentistry, Texas A&M University, Dallas, Texas. She is founder and cohost of the International Oral Lichen Planus Support Group (dentistry.tamhsc.edu/olp/) and coauthor of General and Oral Pathology for the Dental Hygienist, now in its third edition. Dr. Burkhart is an academic affiliate fellow with the American Academy of Oral Medicine, where she also serves as chair of the Affiliate Fellowship Program Committee. She was awarded the Dental Professional of the Year in 2017 through the International Pemphigus and Pemphigoid Foundation, and she is a 2017 Sunstar/RDH Award of Distinction recipient. Her professional interests are in the areas of oral medicine and the relationship between oral and whole-body health, with a focus on mucosal disease and early oral cancer detection. Contact her at [email protected].