Periodontal musings
by Lynne H. Slim, RDH, BSDH, MSDH
I stepped into the shower this morning, and the word “musing” popped into my head. Don’t ask me why it landed there because I don’t have a clue. David, my husband, was standing nearby. I asked him to define the word for me. David speaks the Queen’s English, so I never hesitate to ask him anything, even if it’s trivial or absurd.
Synonyms for “musing” are “ruminating” and “contemplating.” Those three words describe my mood this week. I received tragic news that Nathan, my personal trainer, who was like a second son to me, died unexpectedly last week. The news hit me very hard. I had been working with Nathan for well over a year, and he was a fabulous fitness trainer. Nathan was the perfect personal trainer for me, because he believed in me and tolerated my erratic behavior. I would return from a vacation and jump on the scale to find that my weight had gone up by two pounds. He never even blinked, but he would certainly work me harder that day, though. He stood by me no matter what.
A television news item this week hit me like a bomb, too. The news anchor announced that a child had died from complications of an abscessed tooth. A seventh grader named Deamonte Driver was a well-liked 12-year-old whose mother had no dental insurance. Apparently, the oral infection spread to his brain. Many have wondered why a routine extraction that might have cost about $80 wasn’t made available to this child.
The story claims that the child’s mother didn’t have adequate medical insurance and that his problems went unnoticed because his younger brother also had rampant caries. Even though the family had Medicaid, the mother reported that it was difficult to find dental care. In January 2007, Driver began to experience headaches and seizures, and he was transported to a children’s hospital where he had two surgeries. Doctors believed that bacteria from an abscessed tooth had spread to his brain.
In my January 2006 column I wrote about the tragedy of American health care. I said we look forward to the day when Advanced Dental Hygiene Practitioners (ADHPs) are freed from supervised practice. We could begin to provide advanced preventive therapies, simple restorative procedures, and appropriate referrals to individuals in need. Let’s remember Deamonte Driver and vow to hold true to our future plans for our beloved profession.
Reprimanded for bad numbers
To make matters even worse (I don’t mean to depress readers), I received a phone call this week from a close colleague who was chastised by his employer because his monthly productivity was down from the month before. Mind you, this particular hygienist is not your chat-and-polish hygienist; instead, he is what I call a “professional health educated hygienist” whose skills and protocols are second to none. It turns out that his monthly production was being compared to another hygienist who overtreats patients and works on a 45-minute schedule.
I have to be totally honest about something before I explode into a million pieces (it wouldn’t be a pretty sight!). How can professional health-dedicated hygienists be expected to meet “production” quotas? This word “productivity” as applied to dental hygiene is repulsive to me. Since when have we become assembly-line production workers? If it just so happens that our daily schedule is filled on one particular day with recare patients who do not need radiographs and who are periodontally healthy, are we supposed to feel guilty? Are we supposed to overtreat patients with unnecessary radiographs and other services just to meet production quotas?
The health-dedicated hygienists I know and respect don’t concern themselves with production, because clinical excellence almost always results in dental hygiene department success. It’s true that ethical practice management consultants help practices maximize hygiene department performance. But such recommendations are accomplished in a way that focuses on improved oral and general health.
My contemplative mood continues when my “down in the dumps” colleague also tells me that his employer doesn’t really understand a registered dental hygienist’s contribution to the gingival/periodontal health of his patients. By this point, I’m ready to raid the refrigerator or hit one of my precious dogs on the head. I rant and rave on the phone about our value, and I try to make him feel better by telling him about some of the new research I have been reading regarding the clinical benefits of preventive programs for patients who are periodontally healthy or for those with minimal disease.
As usual, he thinks I am a looney-tune for getting excited about research but he tolerates my quirky ways.
The proof of our value
If anyone ever questions your value as a registered dental hygienist in improving/maintaining a high level of oral hygiene in your patients, cite the long-term study by Axelsson, Nystrom, and Lindhe titled “The long-term effect of a plaque control program on tooth mortality, caries and periodontal disease in adults.”1 Axelsson and his colleagues monitored the tooth loss, caries, and attachment loss in a large group of adults (550 were recruited and 70 percent completed the study) during a 30-year period. These subjects maintained a carefully managed plaque control program. Few teeth were lost during the 30 years of maintenance, and the main reason for any loss was root fracture. Out of the total number of subjects who were followed for 30 years, only 21 teeth were lost because of progressive periodontitis or dental caries! Among the various groups of subjects who were defined by age, the mean (average) number of new carious lesions was only 1.2, 1.7, and 2.1. All dental hygiene clinicians need to keep this particular study in their operatories, and it should be laminated for all to read!
Here’s another important study to keep in our public relations toolbox: “A three-year prospective study of adult subjects with gingivitis II: microbiological parameters.”2
Excited like I was to hear about it?
The objective of the research was to determine whether the clinical benefits obtained by a periodontal prevention program were accompanied by beneficial changes in the subgingival microbiota. What’s the subgingival microbiota? In simple terms, it’s the colony of microorganisms that inhabit the subgingival environment being studied.
The study population included 124 adult patients in the United States and in Sweden who were either periodontally healthy or minimally diseased. Subjects received a dental prophylaxis (supragingival scaling and polishing) and home-care instructions at the beginning of the study and every six months thereafter for a total of three years.
A DNA probe count (which counts the number and types of microorganisms) revealed some startling statistics that mean good news for dental hygienists everywhere! It seems that preventive measures aimed at supragingival plaque control are accompanied by shifts to a more host-compatible subgingival microbiota. The duration of these shifts lasted longer than the researchers expected, and it wasn’t until the third year that the subgingival biofilms returned to their original composition.
On tooth surfaces, the supra- and subgingival biofilms form a continuum.3 This means that a prophylaxis and optimum home plaque removal not only reduces the microbial load supragingivally but it also brings about shifts in the subgingival microbiota. The current thinking is that supragingival plaque control decreases inflammation and gingival crevicular flow, which in turn may provide fewer nutrients for the subgingival periodontopathogens.
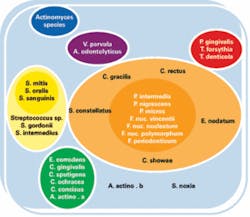
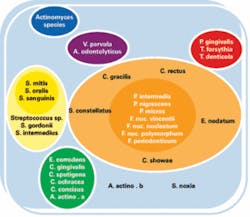
Starve the buggers, I say, and this thought is indeed supported by current research! As a result of meticulous debridement (which is our area of expertise and ours alone), there is a reduction in the total number of microorganisms, and there is also a reduction in the number of red and orange complex species.3 The red and orange complex species are found in higher counts in individuals with periodontitis. (See figure 1 which displays the various complexes of microorganisms.) Years ago, we used to think that supragingival instrumentation and home plaque control had a minimal effect on the subgingival microbiota.
Several reports now suggest that these measures result in a profound effect on subgingival biofilms. It’s not enough to lead to a microbiota that is compatible with health but it does indeed affect the amount of subgingival biofilm and its composition.
How can we apply this research to the everyday delivery of clinical services? Persistent, meticulous control of biofilm plaques, professionally and at home, is a goal worth striving for! Discourage hygienists from working on a 45-minute recare schedule. We all know that even an hour per recare adult patient isn’t always enough! Take time to customize homecare, use disclosing agents, and take your time with instrumentation. Slow down when using micro-ultrasonic inserts during recare appointments and become proficient at using the straight, right, and left inserts. Become a professional health-dedicated dental hygienist who remains on the cutting edge of anti-infective therapy, and your patients will follow you wherever you go.
So, back to my contemplative mood. This month’s column started out a bit on the dark side. In all honesty, though, I see our future as sunny-side-up, full of opportunities for clinicians to shine and be recognized. Think positive and let’s continue to celebrate our worth.
Lynne H. Slim, RDH, BSDH, MSDH, is a practicing hygienist/periodontal therapist who has more than 20 years’ experience in both clinical and educational settings. She is also president of Perio C Dent Inc. (Perio-Centered Dentistry), a practice-management consulting firm that specializes in creating outstanding dental hygiene teams. Lynne is a member of the Speaking and Consulting Network (SCN) that was founded by Linda Miles, and has won two first-place journalism awards from ADHA. Lynne is also owner/moderator of a periodontal therapist yahoo group: http://yahoogroups.com/group/periotherapist. She can be contacted at [email protected].
References
1 Axelsson P, Nystrom B, Lindhe J: The long-term effect of a plaque control program on tooth mortality, caries and periodontal disease in adults. Results after 30 years of maintenance. J Clin Periodontol 2004: 31: 749-757.
2 Teles RP, Bogren A, Patel M, Wennstrom JL, Socransky SS, Haffajee AD. A three-year prospective study of adult subjects with gingivitis II: microbiological parameters. J Clin Periodontol 2007; 34: 7-17.
3 Teles RP, Haffajee AD and Socransky SS: Microbiological goals of periodontal therapy. Perio 2000 2006: 42: 180-191.