My Nerdy Disposition
by Lynne H. Slim, RDH, BSDH, MSDH
During the Christmas holidays, I received several e-mails and telephone calls regarding my December 2007 column, "Periodontal Nitwits and Flossing." Most readers agreed with my comments. But, in trying to make my point as clear as possible, I unintentionally offended the hygienists with whom I work. I sincerely apologize to these colleagues, and to any other readers who may have taken my remarks personally. Those of us who love to write and challenge the status quo sometimes have to eat humble pie, and I've learned that it's an unavoidable part of the job. I wish it were not. Like politicians, we err on the side of caution and try not to offend anyone, but sometimes even our best intentions turn out to be misguided.
I work one day a week in a high-quality, general dental practice in Buckhead, Ga., which is near Atlanta. I love my fellow team members, and we're like one big, happy family, although we do have occasional spats over minor issues. My employer is a member of the Academy of Restorative Dentistry, and he frequently continues his education at the Pankey Institute in Florida. I work with two excellent dental hygiene clinicians, and the three of us pride ourselves in keeping our patients healthy and well-educated. We practice conservative periodontal therapy successfully, and our patients go home with better (and healthier!) goody bags than trick-or-treaters after a whole evening of going house to house.
We customize our patients' oral hygiene because no one in our practice believes in a cookie-cutter approach. I mentioned in the December column that the hygienists in my office challenged me on my thinking that it's OK for some adult periodontal patients to use appropriate interdental biofilm-removing devices other than floss, such as interdental brushes. I didn't mean to imply that these two hygienists were in the periodontal nitwit category, because they are definitely not! But I wanted to make a point that we can agree to disagree about the value of dental flossing in adult periodontal patients. I think we should continue to discuss this topic and try to reach a consensus.
About once a week, I e-mail my good friend, Dr. Paul H. Keyes. I also like to talk to Dr. Walter Loesche, and these retired periodontal researchers are wonderful mentors who are more than happy to discuss periodontal issues with me, especially when I'm troubled by something I don't understand. You see, as a periodontal "nerd," I'm forever questioning theories and procedures, and my "nerdy" disposition sometimes gets me in hot water, particularly when I disagree with a professional colleague. Drs. Keyes and Loesche have never been big advocates of dental flossing as a form of pathogenic biofilm removal in periodontal pockets, particularly in patients with periodontitis. Flossing has serious limitations in sites where there is recession/attachment loss and wide embrasures.1
Here are some other "nerdy" thoughts I had as I pondered this issue:
• What about the adult patient who already flosses but who, as a periodontal patient with clinical attachment loss and embrasures the size of craters, needs additional reinforcement to fight the pathogenic biofilm battle? Should he/she discontinue flossing?
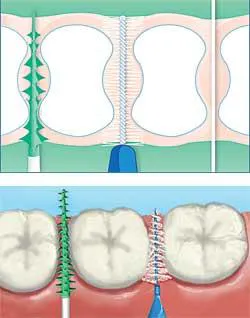
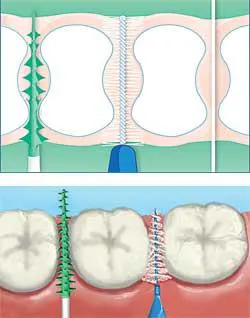
It really doesn't matter what this pathetic nerd thinks (and I'm referring only to me). But common sense tells me that we should tread carefully. If the patient enjoys flossing and is a bit on the anal-retentive side, I'd tell him or her to continue flossing, but I'd make sure to pull out my nerdy laminated visual aid, which shows the hourglass shape of posterior teeth to convince patients to add an interdental brush where it fits. I'd also customize the interdental brush size, like an old-fashioned shoe salesman who fits shoes with a shoe-fitting device. (As a girl I had to wear Stride Rite shoes because I had nerdy feet that rolled inward when I walked. Back then, Stride Rite shoes were plumb ugly and our choices were limited.)
• What about the dental caries risk for adult patients who eliminate daily flossing from their oral hygiene regimen and substitute interdental brushes, picks or wooden sticks? Yes, it's boring, but let's examine it anyway. For those who think that flossing prevents dental caries on proximal surfaces, this thinking is now considered questionable and quite possibly falls into the "nitwit" category.
Does this statement shock you? If so, I want to direct you to a really nerdy library: the October and November 2007 issues of the Journal of the California Dental Association (www.cdafoundation.org/library). There you will find a wonderful series of articles on caries management by risk assessment (CAMBRA) that has caught on in several parts of the United States, particularly among practicing nerds. CAMBRA uses a risk assessment protocol for diagnosis, treatment and prevention of dental caries, and once the risk factors are assessed, treatment recommendations are put in place.
Caries is now carefully assessed and we no longer recite the mantra to "brush and floss" and "eliminate sugar from the diet." The authors point out that patients with high plaque levels frequently demonstrate no evidence of dental caries! It took my nerdy brain quite some time to wrap itself around this new paradigm in caries management, but I now understand that cariogenic biofilm (biofilm filled with cariogenic bacteria) in the presence of a specific oral status (situation in which biofilms become pathogenic) is what leads to the demineralization of dental hard tissues.
I urge readers to read the CDA journal articles in full and implement the CAMBRA protocol. Better yet, schedule a staff meeting for the entire team to study the CAMBRA protocol and make plans to implement it. You might want to continue to recommend daily flossing to patients at high risk of dental caries, but customization of oral hygiene care is always preferable to a cookie cutter approach. (Both TePe and Sunstar Americas have beautiful color drawings of interdental spaces that show the hourglass shape of posterior teeth. I have laminated copies of both so I can show patients how posterior embrasures are shaped.)
• What about flossing to reduce gingivitis? Is there evidence to support this? Absolutely! Mechanical removal of plaque biofilms remains the primary method for controlling supra-gingival accumulations.1 Manual and power toothbrushes can remove some supra and subgingival plaque biofilms, but they are incapable of removing plaque biofilms on their own.1 Being the nerd I am, I remember discussing a study in the 1970s (while I was at Old Dominion University) that showed that the addition of flossing to tooth brushing improved gingival health, and neither waxed or unwaxed floss was superior.2 Many studies since the 1970s have shown that flossing removes both plaque and gingivitis scores.1 Many dental hygienists, dentists and dental assistants are biased towards manual finger flossing, so it's important to remember that interproximal cleaning suggestions should be based on a patient's ability, preference and oral status.1
About the Author
Lynne Slim is the perio therapy columnist for RDH magazine and an award-winning dental author who has published extensively in dental/dental hygiene journals. Lynne is the CEO of Perio C Dent, a dental practice management company. Lynne coaches dental hygienists and dentists in ultrasonic instrumentation and other advanced hygiene initiatives. She is also the owner and moderator of the periotherapist yahoo group:www.yahoogroups.com/group/periotherapist. In addition, Lynne is the editor of Sunstar America's e-newsletter "The GUMline." Lynne welcomes speaking engagements on the topic of conservative periodontal therapy and other dental hygiene-related topics. Lynne can be reached at: [email protected] or www.periocdent.com
References
1 Asodoorian J. CDHA position paper. Canadian J of Dent Hyg. 2006; 40(3): 1-9.
2 Finkelstein P, Grossman E. The effectiveness of dental flossing in reducing gingival inflammation. J Dent Res. 1979; 58(3): 1034-1039.