Science to the rescue
Appreciating the role of irrigation in maintaining optimal oral health
by Anne Nugent Guignon, RDH, MPHAbasic cornerstone of every dental hygiene student's education is helping patients understand, embrace, and implement effective self-care practices. For decades, students have been taught that brushing and flossing were critical tasks that would ensure lifetime oral health. Discussions in academia also included supplemental activities or products like picks, interproximal brushes, rubber-tip stimulators, mouth rinses, therapeutic toothpastes, site-specific brushes, floss threaders, and oral irrigators. Despite learning about other approaches, brushing and flossing remained the epicenter of adequate oral hygiene. As students, we believed health could not be achieved without performing these two activities on a daily basis.
While many adopted this thinking while in school, most of us found that oral health in the real world was not that easy to explain. Visible plaque did not necessarily result in disease, nor did the presence of calculus or a patient's reported health status. It did not take long to realize that disease is a very complex phenomenon. There have always been patients who could not, or would not, use traditional floss, yet they maintained clinical health year after year. In direct contrast, other patients floss every time a morsel of food passed their lips, yet they always remain in an active state of gingivitis, periodontitis, or caries.
Observant clinicians, frustrated by the enormous variations in patient health, started experimenting with recommendations that defied conventional thinking. Decades ago, forward-thinking clinicians recommended shorter than average recare intervals and adopted full-mouth ultrasonic instrumentation, utilizing fluid irrigation. Patients who began using power brushes and oral irrigation devices achieved oral health levels that went past our wildest dreams.
While we may not have understood exactly what we were seeing, our patients were becoming healthier. Gingival tissues became pink, firm, and quit bleeding. Patients were pleased with the results and many of us retired the floss-and-brush lecture.
Ten years ago, advances in confocal scanning electron microscopy led to a new understanding of how microorganisms form complex polymicrobial communities – not only in the mouth, but also on a wide variety of surfaces. Biofilm forms on showerheads, contact lenses, the surface of the ocean, air conditioning units, and devices implanted in the human body.1-5 While at Montana State University Center for Biofilm Research, J. William Costerton, PhD, coined the term biofilm to describe these diverse microbial communities.4
Scientists now estimate that 99% of all microorganisms on earth survive and thrive in a biofilm. Not all biofilm communities are considered pathogenic, but the Centers for Disease Control and Prevention estimates that at least 80% of all infectious diseases have a distinct biofilm component. Examples of biofilm-based diseases in humans include otitis media, bacterial endocarditis, Legionnaire's disease, and periodontal disease.4,6,7
As free-floating organisms begin to collect on a surface such as a tooth, the microbes begin to produce extracellular polysaccharide, a slimy substance that protects biofilm inhabitants. When the microorganisms encased in biofilm reach a critical mass, a process called quorum sensing allows microbes to communicate via the production of chemicals called pheromones. As the biofilm mass matures, microbial colonies subdivide the workload, creating more diversity.1,7
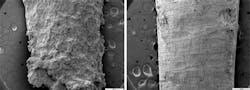
Untreated and treated bioflim samples above attest to the effectiveness of irrigation. The treated tooth had three seconds exposure, resulting in 99.9% removal. Dr. J. William Costerton, the founding director for the USC Center for Biofilms commented, "The results were almost impossible for me to believe the first time through. One of the difficulties with plaque biofilm is that you really can't see it – it's clear. So we didn't have visual evidence of complete removal. But now with these direct methods, the scanning electron microscopy, you apply the Waterpik to plaque on a surface of a tooth and you look with a scanning scope and it's gone. It's simply gone. And that's unequivocal and unarguable."
Research demonstrates that a mature biofilm has multiple regions with varying pH and oxygen levels that support highly diverse organisms contributing to multispecies biofilm masses.8 Low oxygen levels favor the proliferation of anaerobic organisms, microbes implicated in the development of gingivitis, and more aggressive forms of periodontal disease. In addition to anaerobes, Candida albicans is classified as an opportunistic fungal pathogen that can readily coexist with known periodontal pathogens, as well as Streptococcus mutans, an organism implicated in developing carious lesions. Yeast organisms promote a highly acidic microbial environment favored by the pathogens.9,10
Tiny channels within a biofilm allow nutrients and waste products to flow through these highly interdependent polymicrobial communities.1,2 In other words, one microbe's waste products serve as another's gourmet meal. Biofilms are classified as viscoelastic substances that combine both the properties of a fluid and a solid.8
Biofilms are elastic and can move across surfaces. Over time, biofilm can change from a slimy, sticky, elastic substance to a brittle solid.8 A perfect example of this phenomenon is calculus on a tooth.
The deepest layers of biofilm contain organisms known as persisters – microbes that remain semidormant but are fully capable of reforming a new mature biofilm when a biofilm community is disrupted or stressed. Persisters are thought to contribute persistent recurrent infections that baffle the efforts of the patients and clinicians alike.6,7,11,12 The presence of persister microbes left behind by oral hygiene methods that do not eradicate all vestiges of plaque on the tooth surface may very well be the source of infection for those that suffer from chronic gingivitis, bleeding, and ongoing periodontal disease.
While biofilms can be torn away from their surface attachments through a variety of actions, research indicates that biofilms are difficult to remove completely1,4,8 by conventional methods such as brushing, flossing, and hand scaling. Biofilm disruption via some type of scraping action is limited to a device coming in direct contact with the tooth surface, which is nearly impossible in the oral cavity. Factors that compromise biofilm disruption by some type of scraping action includes complex tooth anatomy, malpositioned teeth, orthodontic appliances, restorative materials, complex restorations, limited ability to reach a tooth surface, and compromised manual dexterity.
Research that speaks for itself
Until recently, it was impossible to know if plaque biofilm on the tooth surface was really disrupted through conventional methods. Research published in 2009 by Dr. Costerton's team at the University of Southern California's Center for Biofilm Research, however, provided some amazing results. Pieces of teeth covered with a mature biofilm were subjected to a pressurized, pulsating stream of water from a Waterpik oral irrigator (operated at a medium setting using a standard jet tip for three seconds). Scanning electron microscopy showed 99.9% of the plaque biofilm was gone after this short exposure to the water jet. In addition, 98.9% of biofilm was removed using a specially designed orthodontic tip that features a conical micro brush embedded at the tip end.13
Additional research further substantiated the importance of oral irrigation via a Waterpik. One study showed that the Waterpik device was more effective in improving gingival health as traditional string floss14 and that oral irrigation was three times as effective in removing biofilm around orthodontic brackets, one of the biggest challenges our patients face at home.15,16
Studies have demonstrated that, if properly used, the pulsating, pressurized stream of fluid from the irrigator using a standard subgingival tip with the fluid flow directed perpendicularly to the target area along the CEJ can penetrate approximately 50% of the pocket.17 A soft, conical periodontal tip used for periodontal irrigation can penetrate 90% of a 6 mm pocket, providing an effective option for those challenged with managing deeper periodontal pockets.18
Oral irrigation is a perfect example of a minimally invasive approach to maintaining health. Waterpik irrigation units use water, pressure, and pulsation to disrupt the enemy – plaque biofilm. The device is easy to use, dislodges stubborn food particles, flushes away disease-producing organisms, and provides a clean, fresh feeling. The ultimate goal is to remove pathogenic biofilms on a daily basis, which sets the stage for the formation of a healthy biofilm, resulting in homeostasis among oral organisms.
Enhancing home care effectiveness
Clinical dental hygienists are expected to guide patients in the selection of devices and tools that create health. We are charged with developing a protocol that is not only effective but is supported by research-based evidence. Patients want a regimen that is easy and fits their personal lifestyle. Teeth are the only common denominator among our patients, so a one-size-fits-all approach will never be appropriate. In addition, we must consider what will motivate a patient to include a particular activity in their daily routine. Based on the science, oral irrigation makes sense; however, clinicians need to take into account the human factor when making recommendations.
Recognizing diversity is the key to successful recommendations and subsequent changes in behavior. A certain segment of the population will do whatever it takes to achieve and maintain health. They want to be in charge of their own health outcomes. Recommending oral irrigation to these so-called health nuts is easy.
Scientists and those interested in technology appreciate the science behind irrigation and how sophisticated devices can help achieve health. The all-natural crowd gravitates to disrupting biofilm using a pulsating water jet.
Oral irrigators are perfect for people with large hands, limited dexterity, a hyperactive gag reflex, an inability to open wide, or who hate to put their hands in their mouths. Irrigation is an obvious choice for patients challenged by implants, crowns and bridges, and orthodontic appliances. The Waterpik is perfect for those who experience chronic gingivitis, are not responding to other therapies, or who will not commit to more traditional homecare activities.
Changing population needs and expectations
The overall health of the nation has been changing over the last half century. Thirty-four percent of those 20 or older in the U.S. population are now classified as obese and the same number are considered overweight – conditions that are contributing to the dramatic increase in diabetes. Close to 8% of the population has been diagnosed with diabetes.
Data from the National Institutes of Health estimate that there are at least 5.7 million people undiagnosed and another 57 million are prediabetic. A three-month randomized clinical trial of 52 subjects with diabetes demonstrated that the twice-a-day use of a Waterpik device coupled with a regular oral hygiene routine can reduce gingivitis, bleeding on probing, and lower levels of pro-inflammatory cytokines.
Arthritis by definition is classified as an inflammatory disease of the joints. Those who are overweight or obese are at increased risk for developing arthritic conditions. One third of all people between 45 and 64 years of age have some form of arthritis, and over half of those over age 65 have arthritis. Arthritis is the leading cause of overall limited physical activity. Painful swollen joints in the hands, wrists, forearm, and shoulder can compromise the effectiveness of traditional oral hygiene activities. In many cases, oral irrigation can allow patients with physical challenges to continue with their personal oral hygiene routines without assistance or with a slight modification of the handle diameter.
Despite the fact that baby boomers are now entering their senior years, as a group their expectations about health, longevity, and independence are dramatically different than those of previous generations. People expect to keep their teeth for a lifetime and are looking for effective alternatives that will allow them to maintain their oral health independently. Oral irrigators and power toothbrushes are particularly well suited for use among this population cohort.
Multiple platforms to suit individual needs
Waterpik technology comes in two different formats. The traditional unit, now called the Ultra Water Flosser, has a full tank fluid reservoir and is powered by a pressure control system with 10 settings. The removable lid serves as a storage pod for a variety of irrigation tips. The Cordless Plus unit is a handheld device, which features a small fluid reservoir and a dual control pressure system. This portable unit can be used in the shower and is a perfect choice for those who travel.
Six different tips are available that will work in either unit and range from a standard jet tip to ones for site-specific applications. Tips with bristles and the Pik Pocket Tip should be replaced every three months. Replace the Classic Jet Tip and Tongue Cleaner twice a year.
Instruct patients to fill the fluid reservoir and attach the appropriate tip to the handle. Prior to activating the tip, ask the patient to position their head over the sink.
Place the tip on a specific starting tooth, slowly tracing the gingival margin on both the facial and lingual surfaces of all teeth, paying particular attention to challenging areas in their mouth. It is important to close the lips gently around the shaft of the tip, allowing fluid to flow from the mouth into the washbasin. Turn the unit off before removing the tip from the mouth.
Plain water provides excellent biofilm disruption but other fluids such as a favorite mouthwash or chlorhexidine for irrigation into a periodontal pocket can be used in Waterpik units. It is important to flush the unit thoroughly with water to remove any chemical residue left from a mouth rinse.
Mother Nature rules. Biofilm will always be found in the oral cavity. The ultimate goal is to disrupt pathogenic biofilm on a daily basis, thus slowing down or eliminating the destructive disease process.
For years, dental professionals have preached the value of flossing, based on the goal of disrupting plaque. Over the years, numerous studies have demonstrated the value of oral irrigation using a Waterpik. There is an adequate body of research to adopt the concept of water flossing. It is time to change the dialogue with our patients and include water flossing via oral irrigation as a legitimate, easy-to-use approach to managing biofilm-based dental disease.
Author's note: The author received an educational grant from Water Pik, Inc., for preparation of this manuscript.
Anne Nugent Guignon, RDH, MPH, provides popular programs, including topics on biofilms, power driven scaling, ergonomics, hypersensitivity, and remineralization. Recipient of the 2004 Mentor of the Year Award and the 2009 ADHA Irene Newman Award, Anne has practiced clinical dental hygiene in Houston since 1971.
References
1. What are biofilms? http://www.erc.montana.edu/biofilmbook/module_01/Mod01_Blue/Mod01_S01_Blue.htm. Published 10/27/06.
2. Where do biofilms grow? http://www.erc.montana.edu/biofilmbook/module_01/Mod01_Blue/Mod01_S02_Blue.htm. Published 10/27/06.
3. How do biofilms impact our world? http://www.erc.montana.edu/biofilmbook/module_01/Mod01_Blue/Mod01_S03_Blue.htm. Published 10/27/06.
4. Costerton JW. The biofilm primer. New York. Springer Science. 2007.
5. Zimmer C. Scientists find a microbe haven at ocean's surface. http://www.nytimes.com/2009/07/28/science/28ocea.html. Published 10/27/09.
6.What is the connection between biofilms and persistent infections? http://www.erc.montana.edu/biofilmbook/module_07/Mod07_S01-1_Blue.htm. Published 10/27/06.
7. What is the evidence that biofilm forms in chronic wounds? http://www.erc.montana.edu/biofilmbook/module_07/Mod07_S04-1_Blue.htm. Published 10/27/06.
8. What are the key characteristics of biofilms? http://www.cbe.montana.edu/biofilmbook/module_01/Mod01_Blue/Mod01_S04_Blue.htm. Published 10/27/06.
9. Marsh PD. Dental plaque as a biofilm and a microbial community - implications for health and disease. BMC Oral Health. 2006 Jun 15;6 Suppl 1:S14.
10. Marsh PD. Are dental diseases examples of ecological catastrophes? Microbiology. 2003 Feb;149(Pt 2):279-94.
11. Lewis K. Persister cells and the riddle of biofilm survival. Biochemistry (Mosc). 2005 Feb;70(2):267-74.
12. LaFleur MD, Kumamoto CA, Lewis K. Persister cells, dormancy and infectious disease. Antimicrob Agents Chemother. 2006 Nov;50(11):3839-46. Epub 2006 Aug 21.
13. Gorur A, Lyle DM, Schaudinn C, Costerton JW. Biofilm removal with a dental water jet. Compend Contin Educ Dent. 2009 Mar;30 Spec No 1:1-6.
14. Barnes CM, Russell CM, Reinhardt RA, Payne JB, Lyle DM. Comparison of irrigation to floss as an adjunct to tooth brushing: effect on bleeding, gingivitis, and supragingival plaque. J Clin Dent. 2005;16(3):71-7.
15. Sharma NC, Lyle DM, Qaqish JG, Galustians J, Schuller R. Effect of a dental water jet with orthodontic tip on plaque and bleeding in adolescent patients with fixed orthodontic appliances. Am J Orthod Dentofacial Orthop. 2008 Apr;133(4):565-71.
16. Burch JG, Lanese R, Ngan P. A two-month study of the effects of oral irrigation and automatic toothbrush use in an adult orthodontic population with fixed appliances. Am J Orthod Dentofacial Orthop. 1994 Aug;106(2):121-6.
17. Boyd RL, Hollander BN, Eakle WS. Comparison of a subgingivally placed cannula oral irrigator tip with a supragingivally placed standard irrigator tip. J Clin Periodontol. 1992 May;19(5):340-4.
18. Braun RE, Ciancio SG. Subgingival delivery by an oral irrigation device. J Periodontol. 1992 May;63(5):469-72.
19. Miyamoto T, Kumagai T, Lang MS, Nunn ME. Compliance as a prognostic indicator. II. Impact of patient's compliance to the individual tooth survival. J Periodontol. 2010 Sep;81(9):1280-8.
20. Galliher JM, Post DM, et al. Patients' question-asking behavior during primary care visits: a report from the AAFP National Research Network. Ann Fam Med. 2010 Mar-Apr;8(2):151-9.
21. Felo A, Shibly O, Ciancio SG, Lauciello FR, Ho A. Effects of subgingival chlorhexidine irrigation on peri-implant maintenance. Am J Dent. 1997 Apr;10(2):107-10.
22. Watts EA, Newman HN. Clinical effects on chronic periodontitis of a simplified system of oral hygiene including subgingival pulsated jet irrigation with chlorhexidine. J Clin Periodontol. 1986 Aug;13(7):666-70.
23. Cutler CW, Stanford TW, Abraham C, et al. Clinical benefits of oral irrigation for periodontitis are related to reduction of pro-inflammatory cytokine levels and plaque. J Clin Periodontol. 2000 Feb;27(2):134-43.
24. Al-Mubarak S, Ciancio S, Aljada A, et al. Comparative evaluation of adjunctive oral irrigation in diabetics. J Clin Periodontol. 2002 Apr;29(4):295-300.
25. Moutsopoulos NM, Madianos PN. Low-grade inflammation in chronic infectious diseases: paradigm of periodontal infections. Ann N Y Acad Sci. 2006 Nov;1088:251-64.
26. Overweight and obesity (BMI) - 2009. National center for chronic disease prevention and health promotion. Behavioral risk factor surveillance system prevalence and trends data. http://apps.nccd.cdc.gov/BRFSS
27. 2007 National diabetes fact sheet. http://www.cdc.gov/diabetes/pubs/factsheet07.htm
28. Arthritis - data and statistics. http://www.cdc.gov/arthritis/data_statistics.htm
Past RDH Issues
• Classic Jet Tip – The all-purpose irrigation tip