The surprising benefits of air: Low-abrasive powders for air polishers
By Karen Davis, RDH, BSDH
Dental hygienists have a wide variety of experiences with and opinions about air polishing-everything from loving it to hating it. Patients likely have similar opinions depending on the type of device used, the powders used, and the expertise of the clinician providing the air polishing. If you're the clinician that threw the air polisher into the cabinet a decade ago to gather dust, pay close attention to this article. New advancements in this technology have some pleasant benefits for you and your patients.
With the advent of air polishing devices designed for use with low-abrasive powders, dentists and dental hygienists can obliterate supra- and subgingival biofilm from enamel, exposed root surfaces, and restorative materials efficiently and comfortably. That becomes a game changer.
Air polishing devices with sodium bicarbonate powders are effective stain and biofilm removal on enamel, and highly effective for biofilm removal in pits and fissures prior to sealant placement. But caution must be taken to avoid exposed root surfaces and most restorative materials, which limits their use on periodontal maintenance patients.
In fact, a study published in 2014 by the Journal of Periodontology concluded, "For exposed root surfaces, sodium bicarbonate cannot be recommended." It revealed that even five-second exposure with air polishing devices using sodium bicarbonate powder showed considerable surface defects.1
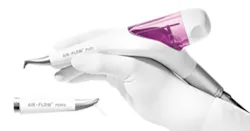
Figure 1: Hu-Friedy/EMS Handy 3.0 Premium Package
Figure 2: Hu-Friedy/EMS Air Flow Master Piezon
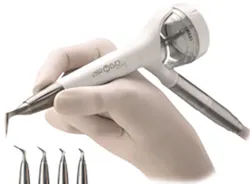
Figure 3: Acteon Air-N-Go Easy
Low-abrasive polishing powders
First, let's examine some benefits of low-abrasive powders. Glycine, an amino acid powder, and erythritol, a natural sweetener powder, are unlike sodium bicarbonate, calcium carbonate, or aluminum trihydroxide powders traditionally used with air polishing devices for supragingival use. In terms of micron size, these supragingival powders are between 40 and 76 microns in size. By comparison, glycine has a micron size of 20-25, and erythritol powder has a micron size of 14.
On the Mohs hardness scale (which measures the hardness of various minerals) these supragingival powders are between 2.5 and 4. Glycine and erythritol powders rank 2 on the Mohs hardness scale. These differences in micron size and hardness translate into a broader use for air polishing, which enables safe use for the removal of biofilm above and below the gum line. In the U.S., glycine powder is currently available, and erythritol powder is undergoing FDA approval.
A 2008 study concluded that air polishing with glycine powder in shallow pockets was safe,2 and a 2012 study confirmed air polishing with glycine powder was safe in deeper pockets.3 A 2014 study concluded that air polishing with erythritol powder is equally safe and can be used as an alternative to glycine.4 It should be noted that these studies were performed on supportive periodontal therapy patients that did not present with significant subgingival calculus, but rather supra- and subgingival biofilm.
Because air polishing devices can obliterate biofilm but do not remove calculus, some clinicians dismiss their value for periodontal maintenance patients. The reality for most periodontal maintenance patients is that they present with isolated areas of calculus but significant amounts of biofilm. They have multiple exposed root surfaces and present with various restorative materials. This should give clinicians pause to consider which methods of biofilm removal are the least abrasive for repeated instrumentation.
A 2007 Journal of Periodontology article by Flemmig et al. reminds us that "Abrasion on tooth surfaces might become substantial over time when the cumulative effects of repeated instrumentation in supportive periodontal therapy are considered."5 This study referenced clinical results of complete biofilm removal in shallow subgingival pockets of supportive periodontal patients with glycine powder air polishing (GPAP) to curettes and ultrasonic instrumentation. GPAP has the added benefits of significantly greater efficiency and greater patient comfort for biofilm removal.
Subsequent data published have collaborated these benefits with GPAP used for five seconds per site to remove biofilm in deep pockets compared to an average of 64 seconds with hand curettes.6 This data supported GPAP for five seconds per site compared to an average of 30 seconds with ultrasonics to remove biofilm on periodontal maintenance patients with deep pockets.3 For patients being seen on a frequent interval, the goal should be the removal of as much biofilm as possible, as comfortably as possible, as efficiently as possible, and as safely as possible. This is in order to preserve tooth structure and adjacent tissues without any deleterious effects. Low-abrasive powders and air polishing devices accomplish these goals.
Another consideration for air polishing with low-abrasive powders includes effective biofilm removal for patients with implants. The International Journal of Evidence-Based Dental Hygiene7 recently concluded that for patients presenting with peri-implant disease: "A therapeutic intervention starting with simple nonsurgical modalities (e.g., air polishing) should be initiated as soon as possible." It is interesting to note that this conclusion was based on a systematic review of studies that used glycine powder air polishing (GPAP) for biofilm removal around implants for mucositis and peri-implantitis.
Compatible devices
Not all air polishing devices support the use of low-abrasive powders. If you attempt to use the powders in inappropriate devices, a plume of powder will most likely cover you and the patient. It may also clog the device. Therefore, before using low-abrasive powders in your air polishing device, check with your manufacturer. When correctly using devices designed for low-abrasive powders, there will be no plume of powder covering the room. However, it should be emphasized that, as with all air polishing devices, high-speed evacuation should accompany the procedure to capture excess water and powder and prevent unnecessary aerosols.
Which air polishing devices are currently designed for low-abrasive powders? The technology is rapidly changing in this area, but two companies that have air polishing devices with substantial versatility are Hu-Friedy/EMS and Acteon.
Hu-Friedy/EMS is a leader in subgingival air polishing as it was the first to provide scientific studies supporting devices with low-abrasive powders for managing biofilm as early as 2003. Hu-Friedy/EMS makes a variety of air polishing devices, but two of their most versatile devices warrant a closer look.
The Hu-Friedy/EMS Handy 3.0 Premium Package as seen in Figure 1 is new to the market this year. It includes the PERIO-FLOW handpiece with disposable subgingival tips that are flexible to adapt to deep periodontal pockets, and the PLUS handpiece, which removes biofilm supragingivally and up to 4 mm subgingivally. The Handy 3.0 Premium Package is a portable device that connects directly to the dental unit and uses low-abrasive powders such as glycine or erythritol and has two interchangeable handpieces.
The Hu-Friedy/EMS Air Flow Master Piezon provides "one-stop shopping" for clinicians. It is a countertop device, as seen in Figure 2. It gives clinicians the greatest versatility in the control of power/water/powder mixtures. It includes piezo ultrasonic technology, a Plus handpiece, a Perio handpiece, and interchangeable canisters for sodium bicarbonate powder or low-abrasive powders, depending on what the clinician wants. The Master Piezon also provides heated water for extra comfort during air polishing.
Another innovative device in subgingival air polishing is Acteon's Air-N-Go Easy. This is a portable device that connects directly into the dental unit and has four different nozzles for different clinical needs. It has the versatility of sodium bicarbonate or calcium carbonate supragingival powders and glycine powder for supra- and subgingival use, as seen in Figure 3. The four nozzles are the Supra nozzle using sodium bicarbonate or calcium carbonate powder for supragingival use, the Perio-Easy nozzle using glycine powder for subgingival biofilm removal in shallow pockets, the Perio-Maintenance nozzle using glycine powder supragingivally, and the Perio nozzle using glycine powder for deeper periodontal pockets.
The paradigm shift
The title of an article published in 2013 by Quintessence International should pique the interest of clinicians about air polishing with low-abrasive powders. It is titled "A Paradigm Shift in Mechanical Biofilm Management? Subgingival Air Polishing: A New Way to Improve Mechanical Biofilm Management in the Dental Practice."8
This article is the consensus of world-renowned experts at the EuroPerio 7 conference reviewing the literature published on subgingival air polishing and low-abrasive powders. Here is a summary of their findings:
- The new generation of powders and devices with subgingival nozzles provide better access to subgingival and interdental areas.
- In shallow pockets up to 4 mm and in deep pockets ≥5 mm, air-polishing removes biofilm significantly more efficiently than hand curettes.
- Subgingival biofilm removal with air-polishing is considerably faster than hand instrumentation or ultrasonics.
- Glycine-based air polishing is perceived as more comfortable by patients than hand instrumentation or ultrasonics.
- Subgingival air-polishing with glycine-based powder is safe if used as recommended.
Download the Clinical Evidence Guide at hu-friedy.com/HFEMS for access to this and other pertinent literature.
The greatest benefit of air polishing with low-abrasive powders during periodontal maintenance or preventive treatment is the fact that it saves you precious minutes. You use these devices and powders first during the clinical protocols with patients rather than at the end of the appointment. Because it is substantially more efficient than biofilm removal with ultrasonics or curettes, this saves valuable time to provide additional services to your patients!
Clinical studies confirm comparable clinical outcomes, so the result is simply a more efficient and comfortable experience for patients when using low abrasive air polishing powders first. These are interesting benefits! Patients adapt easily to this shift in protocols when they're informed that their visit will begin rather than end with polishing their teeth. This is in order to more comfortably and efficiently remove the plaque biofilm from surfaces prior to removal of hard deposits.
What are you waiting for?
With benefits such as preservation of delicate exposed root surfaces and restorative materials, easy access to subgingival biofilm, increased efficiency, and patient comfort, why would you wait to jump into this new paradigm for managing biofilm? If your experience is like mine, this is one game-changer you'll never want to be without! RDH
Karen Davis, RDH, BSDH, is the founder of Cutting Edge Concepts, an international continuing education company, and practices dental hygiene in Dallas, Texas. She is an independent consultant to the Philips Corp., Periosciences, and Hu-Friedy/EMS. She can be reached at [email protected].
References
1. Sahrmann P, Ronay V, Schmidlin PR, Atinn T, Paque F. Three-dimensional defect evaluation of air polishing on extracted human roots. J Periodontol 2014;85:1107-1114.
2. Petersilka GJ, Faggion Jr CM, Stratmann U, et al. Effect of glycine powder air-polishing on gingiva. J Clinical Periodontol 2008;35(4);324-32.
3. Flemmig TF, Arushanov D, Daubert D, et al. Randomized controlled trial assessing efficacy and safety of glycine powder air polishing in moderate-to-deep periodontal pockets. J Periodontol 2012;83(4);444-452.
4. Dragoo L, Del Fabbro M, Bortolin M, et al. Biofilm removal and antimicrobial activity of two different air polishing powders: an in vitro study. J Periodontol 2014;85:e363-e369.
5. Flemmig, TF, Hetzel M, Topoll H, et al. Subgingival debridement efficacy of glycine powder air polishing. J Periodontol 2007;78:1002- 1010.
6. Moene R, Decaillet F, Andersen E, Mombelli A. Subgingival plaque removal using a new air polishing device. J Periodontol 2010;81:79-88.
7. Alqutaibi AY. Air polishing is a promising nonsurgical treatment modality for peri-implant disease. Int. J Evid Based Pract Dent Hygienist 2016;2:57-60.
8. Sculean A et al. "A paradigm shift in mechanical biofilm management? Subgingival air polishing: a new way to improve mechanical biofilm management in the dental practice." Quintessence International 44.7 (2013).