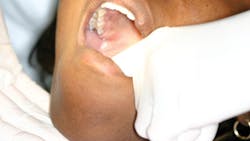
Why palpation is so important: Early detection of oral cancer still depends on correct technique
I attended the Donald Kerr Symposium at the University of Michigan. The theme was, “Personalized Medicine in Oral Cancer.” The seminar had some notable speakers, and I wanted some updates about the human papilloma virus and its role in oral/pharyngeal cancer.
Other topics included valuable information related to the complete treatment of oral cancer patients by head and neck surgeons, ranging from identification of oral/pharyngeal cancer through the actual treatment phase. All of the speakers were excellent and so knowledgeable about HPV and oral cancer.
Two speakers expanded upon the importance of the oral exam in early cancer detection and that the exam is a key factor leading to an early diagnosis - one of the most important components being intraoral and extraoral palpation. One participant asked some specific questions about how one should palpate during an oral exam. I remember thinking that there are probably many dentists and hygienists who really do not know if they are performing this task in the most beneficial way. This is especially crucial regarding pharyngeal cancer since palpation is essential to early detection for this type of cancer.
Also by Nancy Burkhart
Oral medicine: Linking medicine and pathology
The fibroma: Breaking a chronic habit
Carol Bradford, MD, demonstrated on someone close by and suggested some techniques that she felt could be beneficial. Dr. Bradford also stressed the point that these types of cancers are not usually detected early in a medical office but rather in a dental office. She also raised the question of whether we might see dental personnel administering the HPV vaccine since patients are seen more often by dental professionals than medical professionals.
Another speaker, Dr. Mark Lingen, mentioned that a thorough oral exam surpasses any other device that is currently on the market. In the case of HPV, a few signs are known to occur:
- Swelling and nodules in the salivary gland areas such as submandibular and sublingual glands
- Pain, discomfort, or tenderness extending into the auricular area
- Some lesions may be detectable toward the base of the tongue
Because of the extensive tonsillar crypts, there is little to no warning of tissue lesions/ulcerations until the cancer is more advanced in tonsillar cancer. But, palpation is often able to detect the nodes that have been invaded and these nodes often feel firm or hard.
Careful questioning of the patient adds to this vital information. As I listened to Dr. Lingen, I remember thinking that the oral cancer exam is not performed in many offices or performed poorly by others. How many perform a good extraoral exam with optimal palpation?
We continue to see a rise in oral/pharyngeal cancer in younger patients and we seem to be missing the opportunity for early oral cancer detection. Although the HPV vaccine is recommended, several speakers commented that the administration is still low, and it may be 30 years before we see a difference in these types of oral cancers.
| Palpation of salivary glands and floor of the mouth. |
Steps in palpation
Palpation is defined as using the sense of touch to examine anatomic structures or areas for size, shape, consistency, texture, and other characteristics. This is a learned skill that must be practiced many times before a clinician can feel somewhat confident about his or her findings. It is important to develop a systematic method for palpating the structures of the head, neck, and oral cavity. Clinicians should be looking for the following while performing palpations:
- Differences (size, shape, consistency, and texture among others) between structures that occur on opposite sides. For example, submandibular lymph nodes on the right side may be enlarged while those on the left are nonpalpable. Or the left parotid gland may be hard or doughy to palpation while the right gland is not. These differences could be significant and should be noted.
- Before beginning palpation, the clinician should ask the patient to report any feelings of tenderness or pain. In addition, it may be helpful for the patient to report any sort of difference between sensations felt in one area and those felt in other areas. Problems associated with nerve damage, such as paresthesia, may be discovered in this fashion.
- Be aware of temperature variations of structures as they are palpated. A rise in the temperature can indicate increased blood supply to the area and may be associated with abnormalities, such as vascular malformations or infections.
- Alterations in color during palpation of an area should also be noted. Color changes can indicate a vascular lesion or perhaps an inflammatory reaction if the tissue blanches upon palpation. A diascopy is sometimes performed to assist in determining a vascular lesion from others that are nonvascular.
- The clinician should be aware of any sounds that are produced when tissues are palpated. Fluid movement from one part of a lesion to another may cause a crackling sound, or crepitus.
- Pulsation may be observed. This may indicate a vascular issue. A light touch will allow the clinician to observe any vascular areas.
- Palpation of both the intraoral tissue and the extraoral tissue is necessary. Pressing against the floor of the mouth with the fingers of one hand and using the other hand extraorally to feel any abnormality in the sublingual and submandibular glands is optimal.
- Palpation of the chain of cervical nodes along the neck with the patient turning to the right and then to the left. The occipital region and auricular nodes should be palpated as well.
The palpation techniques described above were modified from the textbook, General and Oral Pathology for the Dental Hygienist.
Identification of abnormalities during palpation is just the first step. Formulating a differential diagnosis is the next step. The process then of determining a definitive diagnosis from a differential diagnosis and this can involve a referral, biopsy and/or additional tests.
As always, listen to your patients and continue to ask good questions.
Originally published in 2017 and updated in January 2023.
About the Author
Nancy W. Burkhart, EdD, MEd, BSDH, AAFAAOM
NANCY W. BURKHART, EdD, MEd, BSDH, AAFAAOM, is an adjunct professor in the Department of Periodontics-Stomatology, College of Dentistry, Texas A&M University, Dallas, Texas. She is founder and cohost of the International Oral Lichen Planus Support Group (dentistry.tamhsc.edu/olp/) and coauthor of General and Oral Pathology for the Dental Hygienist, now in its third edition. Dr. Burkhart is an academic affiliate fellow with the American Academy of Oral Medicine, where she also serves as chair of the Affiliate Fellowship Program Committee. She was awarded the Dental Professional of the Year in 2017 through the International Pemphigus and Pemphigoid Foundation, and she is a 2017 Sunstar/RDH Award of Distinction recipient. Her professional interests are in the areas of oral medicine and the relationship between oral and whole-body health, with a focus on mucosal disease and early oral cancer detection. Contact her at [email protected].