Selecting the right tip for a water flossing device
Education tips for patients who are considering a water flossing device for their oral health needs
by Carol Jahn, RDH, MS
True confession: I use my Water Flosser on the #10 setting. When I tell this to other dental hygienists, I often hear, “But I heard that was dangerous,” or “My doctor (or the periodontist that we refer to) says it drives bacteria into the pocket and causes deeper pockets.”
It is difficult to know how this message got started or on what basis. In many cases, it seems to have emanated from an instructor or colleague. No one ever seems to be able to cite or locate a study or even know the specific patient case.
The truth is the Water Flosser is safe to use at any setting including high. This year, the Waterpik Water Flosser earned the ADA Seal of Acceptance as the first powered interdental cleaner. The seal ensures professionals and patients that a product is safe and effective. The Waterpik Water Flosser earned the Seal of Acceptance for the removal of plaque between teeth and below the gumline and for the prevention and reduction of gingivitis.
Let’s look at the evidence on the safety and efficacy of the Water Flosser.
Penetration of bacteria: In 1988 at the University of Missouri Kansas City, a periodontal researcher, Dr. Charles Cobb, conducted a safety study on the Water Flosser. His team looked at patients who needed extractions due to periodontitis. Some of the deep pockets were irrigated with a Water Flosser at the 60 psi setting; other pockets were not irrigated.
Any first-time user should always start on low so they can acclimate to the device.
Post extraction, the pockets were viewed under a scanning electron microscope. Dr. Cobb’s team found disruption of bacteria up to 6 mm in the irrigated pockets. In comparison, the nonirrigated teeth had thick mattes of bacteria. Researchers also viewed the pocket wall and found no trauma or damage. They concluded the Water Flosser is safe.1
Pocket depth: Numerous studies on the Water Flosser and periodontal maintenance patients have evaluated pocket depth. None found an increase in probing depth. A 2000 study at Baylor University found that water flossing at 60 psi significantly reduced probing depth in as little as 14 days.2
Bacteremia: The incidence of bacteremia from using a Water Flosser has ranged from 7% in people with gingivitis3 to around 50% in those with periodontitis.4 This is similar to brushing and flossing (20%-68%), or chewing (51%).5
Confused by tips?
Tips are another area that cause confusion. People sometimes believe the Pik Pocket is the only safe tip to use because it is low-pressure delivery. Others are afraid to use it because it is placed subgingivally. Some fear that if the patient leaves the unit on high instead of turning it to low, it will be damaging to the tissue.
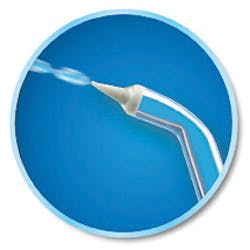
Figure 1: Pik Pocket Tip
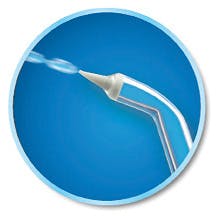
Figure 2: Classic Jet Tip
Regardless of the setting of the unit, the exit pressure from the Pik Pocket tip (see Figure 1) is always 20 psi. The opening at either end of the tip is smaller than the other tips, thus limiting the exit pressure. This tip is designed for the delivery of a medicament—not for full-mouth cleaning. To use, gently place the tip slightly subgingivally into the specific area. It has not been tested against string floss, so it should be used as an adjunct after either the Classic Jet Tip, the Plaque Seeker Tip or the Orthodontic Tip.
There are three tips that have been compared to string floss and can be used for general cleaning. The psi from these tips is dependent upon the setting of the Water Flosser. To use, these tips are designed to be swept along the gingival margin and held in place in the embrasure area for a few seconds.
The Classic Jet Tip (see Figure 2) was the first tip designed for the Water Flosser. The tip is held about a millimeter from the tooth. A study conducted at the University of Southern California Center for Biofilms found the Water Flosser used with a Classic Jet Tip set at 70 psi setting removed 99.9% of plaque biofilm from treated areas.6 Regarding bleeding, a study at the Academic Centre for Dentistry in Amsterdam found the Water Flosser at 60 psi was twice as effective as string floss at reducing bleeding.7
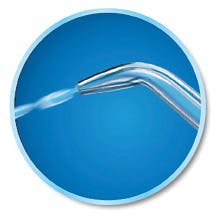
Figure 3: Plaque Seeker Tip
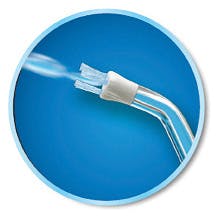
Figure 4: Orthodontic Tip
The Plaque Seeker Tip (see Figure 3) features three thin tufts of bristles. Because of the distance between the opening and the end of these filaments, the tip can be placed along the gingival margin and into the embrasure area. It was designed for use with implants. However, it can be used by anyone and is good for first time users. A study at Tufts University found that people with implants who used the Plaque Seeker Tip with the unit set at 60 psi had a 145% better reduction in bleeding than people who used string floss around the implant.8
The Orthodontic Tip (see Figure 4) has a short tapered brush at the end designed to clean around orthodontic brackets. A study published in the Journal for the American Association of Orthodontics found that adolescents with fixed orthodontic appliances who added a Water Flosser at 50 psi to manual toothbrushing removed three times as much plaque as brushing and flossing, as well as five times as much as brushing alone. The reduction of bleeding was 26% better than with floss and 53% better than brushing only.9
There are many different types of Water Flossers, and professionals often want to know which is better—countertop or handheld. The answer is the best model is the one that meets your patient’s needs, wants, and lifestyle. Both models have a pressure and pulsation range consistent with that used in clinical trials. Most countertop models have a pressure range from 20 psi to 100 psi. For cordless, if there are two pressure settings, it is 45 and 75. For the three setting model, it is 45, 60, and 75.
Any first time user should always start on low so they can acclimate to the device. For optimal results, they should increase the pressure comfortably until reaching the 6 or 7 setting on the countertop or the 60 or 75 setting on a handheld. The Water Flosser can be used at the 8, 9, or 10 setting. The reason that the setting is medium for clinical trials is to ensure a setting that everyone can use.
The Waterpik Water Flosser is safe and effective. It has been evaluated in 70 clinical trials, and it has been recommended by dental professionals and used by the public for 55 years.
Carol Jahn, RDH, MS, is the director of professional relations and education at Water Pik, Inc. She can be contacted at [email protected].
References:
1. Cobb CM et al. Ultrastructural examination of human periodontal pockets following the use of an oral irrigation device in vivo. J Periodontol 1988; 59: 155–163. https://www.ncbi.nlm.nih.gov/pubmed/3162980
2. Cutler C et al. Clinical benefits of oral irrigation for periodontitis are related to reduction of pro-inflammatory cytokine levels and plaque. J Clin Periodontol 2000; 27: 134–143. https://www.ncbi.nlm.nih.gov/pubmed/10703660
3. Romans AR, App GR. Bacteremia, a result from oral irrigation in subjects with gingivitis. J Periodontol, 1971; 42: 757–760.
4. Romans AR, App GR. Bacteremia, a result from oral irrigation in subjects with gingivitis. J Periodontol, 1971; 42: 757–760.
5. Wilson W, et al. Prevention of infective endocarditis. Guidelines from the American Heart Association. Circulation 2007; 116: 1736–1754. http://circ.ahajournals.org/content/116/15/1736.full
6. Gorur A, et al. Biofilm removal with a dental water jet. Compend Cont Educ Dent 2009; 30(Special issue 1): 1–6. https://www.ncbi.nlm.nih.gov/pubmed/19385349
7. Rosema NAM, et al. The effect of different interdental cleaning devices on gingival bleeding. J Int Acad Periodontol 2011; 13, 2–10. https://www.ncbi.nlm.nih.gov/pubmed/21387981
8. Magnuson B, et al. Comparison of the effect of two interdental cleaning devices around implants on the reduction of bleeding. A 30-day randomized clinical trial. Compend of Contin Educ in Dent 2013; 34(Special Issue 8): 2–7. https://www.ncbi.nlm.nih.gov/pubmed/24568169
9. Sharma NC, et al. Effect of a dental water jet with orthodontic tip on plaque and bleeding in adolescent patients with fixed orthodontic appliances. Am J Orthod Dentofacial Orthop 2008; 133: 565–571. https://www.ncbi.nlm.nih.gov/pubmed/18405821