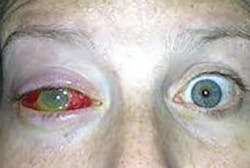
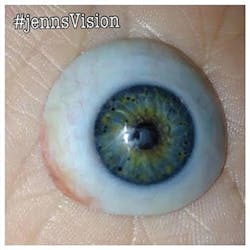
Jenn's vision: Victim of eye injury turns into advocate for eyewear for dental patients
By Noel Kelsch, RDH, RDHAP, MS
When it comes to eye protection for patients, there is no law, no regulation, and no place to go for clearly defined rights and wrongs. Even with no standards to rely on, things are changing. Best practices are being embraced. Why is this happening?
A few years ago, a young lady with a mission wrote to me about her devastating experience in the dental setting.1 Jenn is a wife and mother of two bubbly princesses. She went to the dentist and her life was changed forever. She was not offered eye protection, and as a used syringe was passed over Jenn’s eyes, the dentist dropped it. The needle penetrated Jenn’s eye, injecting bacteria from the mouth into the eye. First aid, such as an eyewash station, was not offered. Jenn was not taken to the emergency room; rather, the dental professional chose to continue treatment. Afterwards, Jenn went home. When the numbness wore off, Jenn felt like her eye was on fire. After multiple surgeries, Jenn lost her vision in the injured eye and must now wear a prosthesis.
Jenn is a positive person and does not want this to happen to anyone else. She has refused to give up, and over the years since the injury she has become an advocate for change. Her mission has been shared by media from Good Housekeeping magazine to ABC News.
I caught up with Jenn this month to see how her mission was progressing. Between princess tea parties and school recitals, we shared the memories of bringing this mission forward. Jenn settled out of court with the dental professionals and cannot discuss the case, but she continues to share her mission!
As you look back at this event, what could have been changed to prevent this from happening?
Jenn: Eye protection. It is that simple. If I had been given eye protection, this would have never happened. Period.
Medically, how has this impacted your life? What has been the outcome of the event in the long term for your eyes?
Jenn: As far as impacting my life, I don’t think there is a facet of my life that has not been affected. Everything I once knew is now a distant memory. I have had to relearn my way of living. I will never get my eyesight back, so I make the best of it. One small example is that the loss of one eye has impaired my depth perception and ability to judge distances. There is no aspect of my life that this has not impacted.
How did this event impact your family?
Jenn: It has impacted my family in so many ways, I don’t think I could list them all. One thing I can say is that it has made me a stronger person. I have shown my girls that when something bad happens to you, you can control how you let it affect you. I hope when they get older and understand the extent of what happened to me, that they will realize how much of myself I gave to give them a “normal” upbringing.
What do you want to have changed in the practice of dentistry as a result of your experience?
Jenn: I would really like for eye protection to be a mandatory law for all patients at every visit for every procedure.
The Centers for Disease Control and Prevention (CDC) states in frequently asked questions that clinicians offer eye protection to patients: “Protective eyewear for patients also can protect their eyes from spatter or debris generated during dental procedures.”2 What are your thoughts on this statement and how have you worked with the CDC on your mission?
Jenn: First, the CDC is very hard to get in touch with! I have sent numerous e-mails, made calls, had other people e-mail them as well - not to mention the campaign. While I am glad that they “suggest” in their FAQ that eye protection is to be worn, I just don’t think that is enough. I think that it needs to be law. Unfortunately, even with that suggested guideline, I feel that some dentists still take advantage and do not supply the proper eye protection. Every state dental practice act should include eye protection for the patient in its infection control section to protect the patient.
What can clinicians do to make sure this does not happen to anyone else?
Jenn: Provide eye protection for every single patient that they see, regardless of the procedure.
Have you heard of this happening to anyone else?
Jenn: Yes, I have read about several others who have gone through the same thing as me, but I have read many more reports on various accidents that have occurred in the dental office involving eyes. This really needs to change. One person is one too many!
Eye protection reminders
There are many things in the dental setting that can damage the eye. As the handpiece rotates 180,000 to 500,000 times a minute, it can cause particles to be projected up to 50 miles an hour! Chemicals, overspray, pieces of old filling materials, prophy paste, or other broken pieces of instruments and materials can fly into patients’ eyes even during routine dental procedures. According to the CDC, more than 2,000 eye injuries occur in the workplace a day.3 Injuries that may even seem minor can cause lifelong vision problems.3
What is required for eye protection for clinicians? The Occupational Safety and Health Administration (OSHA), which develops the regulations for keeping employees safe, has specific requirements for the eye protection that you wear. In the Regulations Standards 29, it states these general requirements:
- 1910.133(a)(1) - The employer shall ensure that each affected employee uses appropriate eye or face protection when exposed to eye or face hazards from flying particles, molten metal, liquid chemicals, acids or caustic liquids, chemical gases or vapors, or potentially injurious light radiation.
- 1910.133(a)(2) - The employer shall ensure that each affected employee uses eye protection that provides side protection when there is a hazard from flying objects. Detachable side protectors (e.g., clip-on or slide-on side shields) meeting the pertinent requirements of this section are acceptable.
- 1910.133(a)(3) - The employer shall ensure that each affected employee who wears prescription lenses while engaged in operations that involve eye hazards wears eye protection that incorporates the prescription in its design, or wears eye protection that can be worn over the prescription lenses without disturbing the proper position of the prescription lenses or the protective lenses.
- 1910.133(a)(4) - Eye and face personal protective equipment (PPE) shall be distinctly marked to facilitate identification of the manufacturer.
- 1910.133(a)(5) - The employer shall ensure that each affected employee uses equipment with filter lenses that have a shade number appropriate for the work being performed for protection from injurious light radiation.
OSHA has adopted American National Standard Institute (ANSI) standards in designing its regulations for eye protection. This is an ever-evolving standard that is updated as new concepts and science-based information comes forward. OSHA currently has adopted three versions of ANSI Z87.1 as compliant with regulatory requirements for standards in eye protection: Z87.1-2003, Z87.1-1989 (R-1998), and Z87.1-2010. In 2015, Z87.1-2015 was adopted.
Z87.1-2015 was required to be implemented by November 25, 2016. It is clearly defined by performance approach and organizes the topics by the hazards encountered. These are the new items in the requirements from 2015:
- Look for the mark! The stamp Z87 should be on eye protection that is ANSI-approved. This eye protection will not only protect from splash and spatter because of its design, but it is impact-resistant or has the coating to prevent exposure to specifics such as laser beam (note that this eye protection must state that it is designed for that purpose).
- Prescription lenses: Magnifiers and readers are incorporated into the standard now, but must meet the same requirements or protective goggles must be worn over them, made by the same manufacturer of the same material and coating.
- Lens and frame marking: The impact-rated requirements include having the manufacturer’s logo as well as “+.” ANSI Z87.1-2015 requires that frames used for a general-purpose protector are marked as Z87- 2. Frames used for an impact-rated protector are marked with Z87-2 + (the lenses would also have a + symbol). Detachable side shields are both marked with Z87+. Additionally, if the side shield is permanent, it does not need to be marked.
- Thickness: There is no maximum thickness any longer. A minimum of 2.0 mm thickness is required, with no maximum.
- Resource: Eye protection must be selected according to the task you are undertaking. The International Safety Equipment Association has a wonderful guide for choosing and using eye protection available at safetyequipment.org.
Jenn’s story has unfolded as one of the paramount lessons in best practices. In choosing eye protection for the patient, best practices require the same standards as for the health-care provider. The patient is exposed to the same risks. RDH
References
1. Kelsch N. Jenn’s vision: A true lesson in best practices. DentistryIQ. http://www.dentistryiq.com/articles/2014/08/jenn-s-vision-a-true-lesson-in-best-practices.html. Published August 1, 2014. Accessed May 21, 2017.
2. Infection control: Frequently asked questions - Personal protective equipment (masks, protective eyewear, protective apparel, gloves). Division of Oral Health. National Center for Chronic Disease Prevention and Health Promotion. Centers for Disease Control and Prevention. www.cdc.gov/oralhealth/infectioncontrol/faq/protective_equipment.htm. Updated July 10, 2013. Accessed May 21, 2017.
3. Eye safety: Eye safety tool box talk - instructor’s guide. National Institute for Occupational Safety and Health Education and Information Division. U.S. Department of Health & Human Services. Centers for Disease Control and Prevention. www.cdc.gov/niosh/topics/eye/toolbox-eye.html. Reviewed July 29, 2013. Accessed May 21, 2017.
NOEL BRANDON KELSCH, RDH, RDHAP, MS, is a syndicated columnist, writer, speaker, and cartoonist. She serves on the editorial review committee for the Organization for Safety, Asepsis and Prevention newsletter and has received many national awards. Kelsch owns her dental hygiene practice that focuses on access to care for all and helps facilitate the Simi Valley Free Dental Clinic. She is a past president of the California Dental Hygienists’ Association.