Lichen planus of the lip
by Nancy W. Burkhart, RDH, EdD
[email protected]
Your patient today is a 56-year- old woman, Mrs. Polk. She is a new patient to your office who was diagnosed with lichen planus approximately eight years ago.
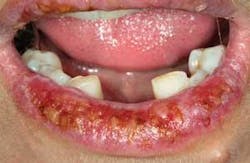
As you assess the lips of the patient, you realize that there are ulcerations on the vermilion borders and that the lesions extend intraorally. The patient tells you that she has not had lip lesions previously, but has noticed the current lesions for over a month (see Figure 1).
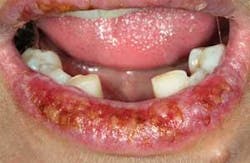
Mrs. Polk informs you that she has the appointment today because she needs to have some resolution of these lip lesions due to the discomfort and unsightly appearance. Even though the appointment was made for radiographs, an exam, and a prophy, you realize that Mrs. Polk has some other issues to address (see Figures 1 and 2).
Etiology: Lichen planus may be found in any lining tissue — for example, the mouth, the esophagus, the eyes, ears, and the genitalia. Skin surfaces such as the scalp, arms, legs, and torso may also be involved.
The etiology of lichen planus is unknown; however, the disease is classified as a cell-mediated immune response. Since a specific antigen has not been identified, many researchers do not classify lichen planus as a true auto-immune disease.
Epidemiology: Lichen planus affects approximately 2% of the population, with 57% or more being women over the age of 50.
Between 25% to 45% of patients have both oral and skin lesions. Since many cases of lichen planus are not reported and may not be included in the research data, the true demographics and incidence are unknown. Some cases of “lichen planus” may actually be what is termed “lichenoid reactions” from dental products, medications, and environmental components. These lesions are difficult to differentiate in most cases from lichen planus. But a careful medical/dental history may help to identify the causative agent, and the condition can then be resolved by removing the offending item.
Method of transmission: Lichen planus is not contagious, cannot be given to another person, and is not transferred via saliva, kissing, touching, or close contact with other individuals. A tendency toward lichen planus has been reported to occur in families, but a hereditary component has not been clearly established.
Pathogenesis: We know that lichen planus occurs when the cell surveillance system, for unknown reasons, goes awry. An antigen has not been found for lichen planus at this time. The disease behaves in a different way when compared to true autoimmune diseases and is not yet clearly understood.
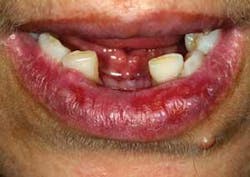
Extraoral characteristics: External skin lesions have been reported to exist in up to 45% of patients at any given time. Partial or full body lesions may exist and symptoms may range from mild to severe. Lesions on the vermilion border of the lip are relatively uncommon although the inner aspects of the lip are often involved. As in other sites, lesions of the vermilion border may appear as classic nonulcerative, painless, white stria (Wickham's stria). They resemble the lacy lichen moss that grows on rocks in gardens (see Figure 3).
Perioral and intraoral characteristics: Lichen planus was originally described as presenting in several forms:
- The reticular pattern consisting of white, keratotic lines or striae
- A plaque pattern of smooth, flat surfaces that resemble a leukoplakia
- Erythematous or atrophic form appearing as highly erythematous-colored tissue with alternating striae
- Ulcerative form appearing as a highly erythematous-colored tissue with alternating striae
- Bullous forms have single or multiple vesicles or bullae. This form is rare and not often seen clinically
Distinguishing characteristics: Cutaneous lichen planus is described as polygonal, pruritic, purple plaques. The lesions may appear anywhere on the body, but often are found on the flexor surfaces of the arms and legs. It may also affect the nails and scalp with varying degrees of destruction.
Significant microscopic characteristics: Lichen planus is generally recognized as a disorder that microscopically resembles a hypersensitivity reaction. Heavy lymphocyte production is diagnostic for lichen planus with liquefaction/degeneration of the basal cell layer. Additional features are a “saw-tooth” rete ridge pattern, and apoptotic keratinocytes in the basal zone are histological features.
Dental implications: The patient seen today is very uncomfortable and needs some treatment in order to minimize the lesions. It would be much too painful to continue with a maintenance appointment since the patient is having trouble eating, speaking, and sleeping at this time.
Research supports frequent professional cleaning because dental cleanings assist in tissue maintenance and repair of lichen planus. Additionally, patients with any mucosal diseases should be checked for oral lesions and tissue changes.
Differential diagnosis: In the case presented, the patient has been previously diagnosed with lichen planus. But in a patient of unknown etiology, a biopsy would be needed along with immunofluorescence diagnosis to rule out other types of skin and mucosal diseases. Several disease states such as lupus erythematosus, pemphigus vulgaris, and mucous membrane pemphigoid share similar characteristics.
Combinations of tests are necessary to differentiate between these skin diseases. Since lichen planus is an inflammatory disease state, adjunct cancer screening devices do not provide any useful information other than identifying cellular changes associated with undetermined inflammation.
Treatment and prognosis: Typically, lichen planus is treated when lesions are symptomatic. Generally, patients are treated using topical corticosteroids. In the case of painful, erosive lesions, more potent corticosteroids are used and sometimes systemic steroids are needed. Asymptomatic forms are usually only monitored.
Occasional biopsies may be needed when lesions are persistent or a change is noted in the tissue.
Corticosteroids used in treatment decrease the inflammation by suppressing the immune response. With the use of any steroid product, candida infection may develop and should be treated with antifungal products. Since lichen planus may be chronic for some patients, treatment may consist of bouts of remission and re-treatment.
Patients should use a bland, unflavored toothpaste and also be advised to limit flavoring agents in foods. Keeping a diary of foods, and other environmental exposures may help identify causative agents that may cause a flare-up.
The vermilion borders of the lip are thin and very sensitive to medications such as topical corticosteroids. The use of a highly potent topical steroid may thin the tissue even further. For most patients, a low potency topical steroid such as desonide cream (0.05% dosage) should be the first treatment attempted using only one or two applications daily. This treatment is not likely to resolve the severe ulcerations being experienced by the patient; however, stronger topical agents may be required but limited to use only until the ulcerations have healed.
Additionally, the patient may be able to control any future outbreaks by using a low dose corticosteroid at the first sign of any lip lesions. Hypersensitivity to dental products, lip balms, or other agents may mimic lichen planus of the lip lesions, especially in the early stages, so a complete evaluation is needed.
Recent studies by Choonhakarn (2008) have advocated the use of aloe vera for some patients. Improvements were seen in control studies of patients who used aloe vera gel compared to placebo groups. The authors suggest that the anti-inflammatory properties of aloe vera contributed to improvement in the patients studied. Again, this would depend on the severity of the case. Additionally, Rajar (2008) reported success of aloe vera in the treatment of vulval lichen planus.
Monitoring lesions of lichen planus:
- Digital slides should be made of the affected areas. These can be compared to the existing lesions during follow-up appointments to assess treatment progress or lack of progress.
- Inflammatory lesions that are widespread are difficult to follow and monitor without previous notations and photographs.
- Asymptomatic lesions may be monitored annually while erosive lesions need to be assessed every few months. Normally, the lesions are monitored in conjunction with maintenance appointments or at any time when changes are noticed by the patient.
For more information on maintenance guidelines and information on lichen planus, visit the International Support Group for Oral Lichen Planus (www.bcd.tamhsc.edu/outreach/lichen).
References
Choonhakarn C, Busaracome P, Sripanidkulchai B, Sarakarn P. The efficacy of aloe vera gel in the treatment of oral lichen planus: a randomized control trial. BR J Dermatol Mar; 158(3):573-7, 2008.
Delong L, Burkhart NW. General and Oral Pathology for the Dental Hygienist. Lippincott, Williams & Wilkins, Baltimore, 2007.
Hayes SM. Lichen planus: Report of successful treatment with aloe vera. General Dentistry, May/June 1999; 268-72.
Ujiie H, Sawamura D, Shimizu H. Development of lichen planus and psoriasis on lesions of vitiligo vulgaris. Clinical and Experimental Dermatology. 31: 375-377, 2006.
Rajar UD, Majeed R, Parveen N, Sheikh I, Sushel C. Efficacy of aloe vera gel in the treatment of vulval lichen planus. J Coll Physicians Surg Pak. Oct;18(10):612-4, 2008.
Regezi JA, Sciubba JJ, Jordan RCK. Oral Pathology: Clinical Pathologic Correlations. 4th ed. Saunders, St. Louis, 2003.
Kahanek N, Gelbard C, Hebert A. Desonide: a review of formulations, efficacy and safety. Expert Opin Investig Drugs. 2008 Jul;17(7):1097-104.