The Differential Oral Pathology Diagnosis
By NANCY W. BURKHART, BSDH, EdD
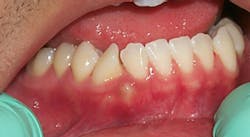
The patient presented in Figure 1 is a 35-year-old male who is in your practice today for a routine maintenance appointment. His medical history is taken, and there are no significant findings. While assessing the oral tissue, you have noticed an area in between and inferior to tooth number 26 and 27, and a rotated cuspid. The area of concern is raised, slightly yellow, very firm when palpated, and is approximately 4 x 7 mm. In addition to the larger growth, a smaller growth is seen closer to the bicuspid approximately 2 x 2 mm with the same appearance. The growth does not appear to be inflamed and consists of smooth tissue. The patient is totally unaware of the raised area in the lower right quadrant.
What course of action would you take in order to systematically make a differential diagnosis of what you are viewing clinically? You would want to begin to determine the etiology of the growth and whether a frictional or a behavior/habit is involved. Unless a clear cause is apparent, you would need to determine a differential diagnosis.
WHAT IS A DIFFERENTIAL DIAGNOSIS?
Determining a differential diagnosis involves distinguishing the characteristics of an entity and applying that knowledge toward a reasonable evaluation that leads to a possible cause/effect. In essence, the ruling out of other possibilities is the main component of the differential diagnosis.
Generally, the practitioner would list the most likely types of diseases and lesions that appear similar to what is being witnessed clinically. Most medical/dental students are taught “If you hear hoof sounds, look for horses and not zebras” or many cite Occam’s razor, which means (in simple terms), “The simplest explanation is usually best.” Or, “Entities should not be multiplied unnecessarily.”
By using a differential diagnosis for determining the possibilities of disease states, the most logical explanations are evaluated first. It is usually best to rule out the more implausible diseases first, based on the information that you have obtained. However, if there is a possibility of a serious disease such as cancer, we want to rule that out first. Making assumptions of benign or malignant states is obviously not a good practice.
WHY IS A DIFFERENTIAL DIAGNOSIS IMPORTANT?
The probability that a certain disease state is occurring is weighed against what is seen clinically, what the patient is reporting, and what is viewed through additional tests that are available, such as laboratory tests and radiographs. A list of the possibilities is generated and listed in the order of probability.
Often, the more detrimental disease states are ruled out first. Sometimes the clinically observed characteristics may be elements of a larger, more ominous type of disease.
For example, the discovery of an osteoma could lead to the discovery of Gardner syndrome — an autosomal dominant disorder characterized by numerous hard and soft tissue tumors and multiple intestinal polyps (polyposis) that have a tendency to become malignant. So, if an osteoma were discovered, Gardner syndrome would be at the top of your differential diagnosis and would need to be evaluated, confirmed, or eliminated as a disease.
Another example is that of lesions that are believed to be of a frictional nature. Sometimes, depending upon the clinical appearance, a biopsy may be necessary. However, if a frictional component is identified, the patient can eliminate the behavior and the tissue will usually return to normal. Another example of this would be cheek chewing (morsicatio buccarum). You would expect the patient to return for a follow-up evaluation with markedly improved tissue once the behavior ceases. If this should not occur, a biopsy may be needed to confirm a definitive diagnosis.
PROTOCOL FOR COMPLETING A DIFFERENTIAL DIAGNOSIS
Complete a thorough medical history. Note any factors that the patient verbally relays while completing the medical history form. Sometimes patients may give you verbal information that they did not think important enough to list on a form. (Maybe there was no appropriate box to check?) Make a list of all symptoms.
Complete a thorough intraoral and extraoral exam with palpation. Some disease states have skin manifestations so an examination of visible skin surfaces is important in a differential diagnosis. The patient may not see any connection between an oral finding and one that is appearing on the skin. A good example is oral lichen planus that may also have purple, polygonal, pruritic papules, or discoid lupus presenting with ulcerative type skin lesions.
Complete a thorough description of any abnormal findings documenting the location, size, shape, color, texture, consistency, and patterns of the lesion (sometimes, a simple drawing gives the pathologist a better idea of the clinical appearance). List the possibility of any external causes of the area in question such as habits and behaviors. Does the patient have a habit of biting the lower lip, etc.?
Intraoral photography is very standard in offices today and well worth the investment. Digital images are easily transferred to a pathologist for evaluation along with the tissue when a biopsy is needed. It is extremely helpful when the pathologist can see both the histology and the clinical image. Images are excellent resources for comparison of chronic lesions and conditions.
The current adjunct devices are helpful in assessing suspicious lesions and may increase motivation for those patients who are undecided as to whether a biopsy is really necessary. Although they do not confirm a diagnosis, the adjunct tests can provide additional information in some cases.
Based on the findings that are gathered, the practitioner should list the most logical explanations for the lesion that is discovered. It is important that the most serious disease states be ruled out first.
We can assess the image presented with this column. What possibilities should be listed? Several entities could be possibilities:
- Osteosarcoma, chondrosarcoma, and Ewing’s sarcoma
- Bone growth (exostosis)
- Osteoma/odontoma
- Gingival cyst
- Lateral periodontal cyst
- Lipoma
Given the clinical appearance of a noninflammatory lesion with no exudates, nonmovable, firm to hard, and painless, several of the above may not fit the profile. At the top of the list for differentials are bone cancers. Although these are very rare, isolated areas such as the image presented here are eye-catching. Exostosis would be possible, but since the area is very isolated, we would still want to keep a more serious bone disorder in mind until we know otherwise.
A radiograph would assist in ruling out something more serious and offer some confirmation. The osteoma or odontoma may be a consideration since small toothlike fragments may be present. The gingival cyst may also have a raised appearance and may have a yellow hue. The lateral periodontal cyst could be a consideration from the clinical appearance. The lipoma does have a yellow hue, but is soft in consistency and is not found in the gingival region but usually in soft tissue such as the buccal mucosa.
WHAT IS THE DIAGNOSIS?
After making a radiograph of the area in question, we discover a supernumerary tooth is present. This is an unexpected finding, and the tooth may continue to break through the tissue and will need removal.
Our consideration of bone diseases or hard tissue components would make sense and are good choices. Had the tooth been more erupted, an inflammatory process may have been present, and we may have had a different arrangement of the differential considerations based on a clinical appearance. In this case, the radiograph was instrumental in confirming the supernumerary tooth.
Using decision trees and critical thinking processes are part of the clinical practice, whether made mentally or by systematically writing your thoughts on paper.
This is also a valuable skill that is developed as clinical exposure is increased.
As always: Keep listening to your patients and always ask good questions. RDH
NANCY W. BURKHART, BSDH, EdD, is an adjunct associate professor in the department of periodontics, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (http://bcdwp.web.tamhsc.edu/iolpdallas/) and coauthor of General and Oral Pathology for the Dental Hygienist. She was a 2006 Crest/ADHA award winner. Her website for seminars is www.nancywburkhart.com. She recently received the Phillips/RDH 2012 Mentor of Distinction” award.
Past RDH Issues