Periodontal Regeneration
A review of the biologic principles of restoring bone resorbed as a result of periodontal infection (part 1 of a two-part series).
Timothy J. Hempton, DDS,
Esther Wilkins, DMD, and
Diane Lancaster, RDH, BS
Periodontal infection can lead to attachment loss and, if not treated, eventual possible tooth loss. Today, many patients are aware that the disease process can be interrupted, thereby arresting the progression of periodontal breakdown. They understand that, with professional help, the dentition can be preserved. Dental hygienists play a critical role in patient assessment, providing various periodontal treatments, and as sources of therapeutic information to enable patients to make better choices in achieving oral health.
Advances have been made in periodontal research over the years which can reverse the process of attachment loss, not just arrest it. To reverse the damage done by periodontal disease, the bone which was lost must be replaced along with the attachment apparatus which connected the bone to the root surface. The purpose of this article is to review the biologic principles of restoring bone resorbed as a result of periodontal infection. Part II will cover Guided Tissue Regeneration (GTR) and discuss the advances that have been made in effecting the re-establishment of the attachment apparatus which connects the new bone to the previously diseased root surface.
Risk factors which affect wound healing
Regrowth of lost bone is known as bone or osseous regeneration. A successful prognosis, as with all periodontal therapies, depends on good patient oral hygiene prior to surgery and after surgery. Good general health is also important for success.
An example of a systemic medical problem that could have a negative impact on successful osseous regeneration is insulin-dependent diabetes, a condition which impairs the patient`s immune system. In general, the patient with diabetes has significant difficulty during wound healing. Tissue repair is slow thereby reducing the prognosis for successful bone regeneration.
Tobacco usage is another consideration. In the last few years, cigarette smoking has been described as having a negative effect on bone regeneration therapy. When a patient smokes cigarettes and the therapist has decided that a bone regeneration procedure would be beneficial, it is important to inform the patient that the smoking habit must be cut back or eliminated. The patient must realize that smoking can lower the prognosis for success significantly.
Anatomy of bone defects
When periodontal disease occurs, attachment loss can proceed with the development of an intrabony defect. To understand the terminology better, remember intra means within. Intrabony delineates within bone. Supra denotes above. Suprabony means above the bone crest.
When periodontal infection results in the development of an intrabony defect, the base of the pocket is apical to (or below) a wall of bone. By contrast, when a suprabony pocket develops, the base of the defect is coronal to the crest above the bone.
Therapists agree that intrabony defects are more amenable to bone regeneration than suprabony defects. As the amount of bone adjacent to the pocket increases, there is more bone available to provide a matrix from which new bone can develop.
Description of intrabony defects
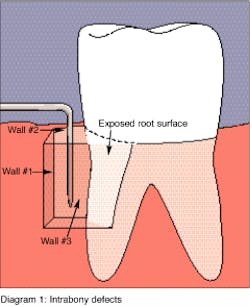
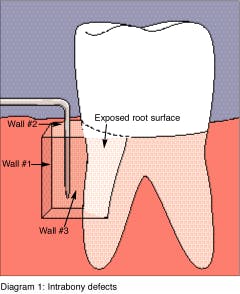
The pocket can be surrounded by bone on one, two, or three sides. To aid this discussion on osseous defect morphology, consider the intrabony defect to be shaped like a box which has no top. The intrabony pocket has four sides, a base and an opening. Refer to Diagram 1.
The base of the box is the base of the pocket. One side of the box or pocket is next to the root surface which has undergone attachment loss. The opening, or where the box is missing its top, corresponds to the entrance to the pocket (i.e., the coronal opening located through periodontal probing).
Three remaining sides of the box are left, that is three walls of the defect. When the soft tissue which lines the pocket is surrounded by three walls of bone, the defect is described as a three-wall defect. If the defect is lined by only two walls of bone, the defect is a two-wall defect. If the defect is lined by only one wall of bone, then it is known as a one-wall defect.
Bone defects which have the best prognosis for bone fill are three-wall defects. The increased number of walls and the height of these walls lends an increased bone matrix on which new bone can grow. When there are fewer numbers of bony walls associated with a shallow defect, the prognosis for success is decreased because the amount of available bone on which to build has decreased.
The walls of the intrabony defect can be located on the facial, lingual, or proximal sides of the exposed root surface. In addition, the pocket itself can be located on the facial, lingual, or proximal surface. Any number of combinations of the parameters can occur. The location of the intrabony defect relative to the tooth and the number of remaining osseous walls is considered to be dependent upon where the risk for periodontal breakdown is greatest.
The interproximal area is involved most often since it is the least accessible for daily removal of bacterial plaque by the patient. Moreover, proximal restorations can be plaque retentive especially if overhangs are present.
Surgical access for root debridement
One goal of periodontal therapy is to achieve a level of root surface debridement which is commensurate with periodontal health. This can be accomplished during phase I therapy especially if good access is achieved during the nonsurgical treatment. Optimal root surface debridement can lead to pocket reduction and possibly bone fill (i.e., osseous regeneration).
Unfortunately, good access is not always available, and therapists may advocate periodontal surgery to gain direct vision of the involved root surface and the number of bony walls surrounding the defect. Surgical access affords improved root debridement especially if furcation involvement or root concavities are present. Surgical access also allows the therapist to visualize the remaining number of bony walls. The surgeon then can make an improved clinical determination as to whether or not a bone regeneration procedure would be beneficial. As previously mentioned, deep three-wall defects have the greatest prognosis for successful bone fill.
Once a defect has been accessed surgically, all granulation tissue in the defect is removed. At that point, the therapist can visualize the exposed root surface which has undergone attachment loss due to periodontal breakdown.
The root surface is thoroughly debrided and planed. When the therapist is satisfied that proper decontamination of the root has been accomplished, a bone graft can be placed. The bone graft material could either be harvested from an edentulous area or from a healing extraction socket entered approximately eight weeks after the tooth has been removed. A healing extraction socket (eight weeks post extraction) offers osseous tissue which is at an optimal stage for bone regeneration.
Bone Morphogenic Protein (BMP)
Another alternative would be to use commercially available bone graft material. One such material is freeze-dried bone supplied by a number of bone banks. It can either be mineralized or demineralized bone. The advantage of placing either the patient`s own bone (an autogenous graft) or human cadaver bone (an allograft) from a bone bank is that either material contains bone morphogenic protein (BMP). The purpose of the bone protein is to enhance bone deposition. BMP is already present in the bone which is adjacent to the defect. In theory, the additional BMP in the grafted bone may effect increased bone deposition during wound healing.
It must be emphasized, however, that to achieve osseous regeneration a bone graft does not necessarily have to be placed. Bone morphogenic protein from donated bone (whether it is autogenous or an allograft from a bone bank) is not essential for regeneration. Successful regeneration of bone can occur without bone grafts. After thorough root debridement, the therapist usually punctures the remaining bone walls to allow blood flow into the area. This is known as decortication. The clot which subsequently forms can serve as a matrix into which new bone (regenerated bone) will develop.
After decortication and possible placement of a bone graft, the therapist can close the surgical area with sutures. Prior to closure, a membrane can be placed which, in principle, allows for development of a new attachment apparatus to the regenerated bone.
A discussion regarding utilization of membranes for regeneration of a new attachment apparatus will be covered in part II guided bone regeneration (GTR).
After the surgery is completed, postoperative instructions are given to the patient regarding pain management and maintenance of oral hygiene. Often chlorhexidine rinses will be prescribed to reduce plaque development. In selected cases, oral antibiotic therapy can be employed to reduce the risk of postoperative infection. A radiograph is taken six months post surgery to determine if osseous fill of the bone defect has occurred.
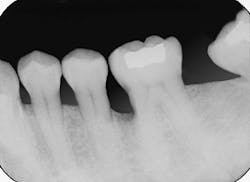
Figure 1 is a radiograph of a 38-year-old nonsmoking female in good health. Vertical bone loss is evident on the mesial aspect of tooth #19. The defect appears deep and the base extends toward the apical one third of the root. Clinical examination revealed 8mm probing depths at the mesiobuccal and mesiolingual line angles. A three-wall defect was diagnosed.
A large deposit of calculus can be seen on the mesial aspect of the molar in Figure 2. Recognizing that the bony defect had an excellent prognosis for bone fill, the root surface was debrided via hand instruments and ultrasonic scaling. The surrounding three walls of bone were then punctured (decorticated) so as to allow blood to exit the narrow spaces and enter the defect. As previously mentioned the blood forms a clot onto which new bone will develop.
The patient was advised that a bone graft consisting of demineralized, freeze-dried bone could be placed to enhance bone deposition. The patient declined placement of a graft.
A resorbable membrane (obtained from Guidor USA) was placed over the defect to effect the development of new attachment. The membrane can be seen in Figure 4. The membrane was placed to exclude all cells which are not progenitor cells for the development of a new attachment apparatus (i.e., new cementum and new periodontal ligament fibers which engage the root to the regenerated alveolar bone).
Figure 5 is a radiograph taken at six months. A comparison of the radiograph in Figure l to the radiograph in Figure 5, using the level of the furcation as a reference point, reveals a significant increase in the amount of bone fill or osseous regeneration on the mesial aspect of the molar.
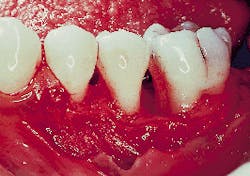
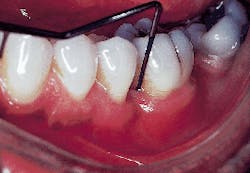
Figure 6 demonstrates a periodontal probe placed on the mesial aspect of the molar. A probing depth of less than 3mm`s can be seen. The original probing depth was 8mm`s.
Summary
Patients who demonstrate good oral hygiene, who are nonsmokers, and in good general health are optimal candidates for bone regeneration procedures. A description of the anatomical characteristics of bony defects where therapists may opt to place bone grafts was reviewed.
Bone grafts may consist of autogenous bone from the patient or freeze dried bone which can be obtained from a bone bank. Either type of bone graft contains bone morphogenic protein which can enhance bone fill in the defect. A bone graft is not essential for bone regeneration however. Bone defects can fill subsequent to root debridement and decortication of the remaining bony walls.
Osseous regeneration has the best prognosis when the defect has three bony walls and is deep in nature. The increased amount of available bone present under this circumstance acts as a matrix for the development of new osseous tissue. After healing, the interface between the newly regenerated bone and the previously diseased root surface can consist of new periodontal ligament fibers engaging new cementum. Development of a new attachment apparatus can be facilitated by placement of a membrane for guidance of this type of tissue regeneration.
Membrane placement and the principle of guided tissue regeneration will be covered in part II.
Timothy J. Hempton, DDS, and Esther Wilkins, RDH, DMD, are members of the department of periodontology at Tufts University School of Dental Medicine. Diane Lancaster, RDH, is a practicing hygienist in Dedham, Mass.
References
- Carranza F.A., Newman M.G., (ed) Clinical Periodontology - 8th ed. Philadelphia: W.B. Saunders Co, 1996, pp 622-636.
- Perry, D.A., Beemsterboer P.L., Taggart E.J., Periodontology for the Dental Hygienist. Philadelphia: W.B. Saunders Co, 1996, pp 244-250.
- Polson A.M. (ed) Periodontal Regeneration; Current Status and Directions. Chicago: Quintessence Publ. Co. 1994.
- Rosenberg M.M., Kay H.B., Keough B.E., Holt R.L., Periodontal and Prosthetic Management for Advanced Cases. Chicago: Quintessence Publ. Co, 1988, pp 191-245.
- Becker W., et al: Clinical and Volumetric analysis of three wall intrabony defects following open flag debridement. J. Periodontol 57:227, 1986.
Diagram 1: Intrabony defects
Figure 1: A periapical radiograph indicates angular bone loss on the mesial aspect of tooth #19.
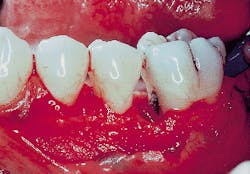
Figure 2: A clinical view of the defect on the mesial aspect of tooth #19 subsequent to flap elevation, note the calculus deposit on the mesial root. The defect adjacent to the first molar is a three-wall defect.
Figure 3: The three-wall defect subsequent to root debridement.
Figure 4: A resorbable membrane which was placed over the defect to facilitate tissue regeneration.
Figure 5: A periapical radiograph taken of toth #19 six months post-treatment. Note the bone fill (osseous regeneration) adjacent to tooth #19.
Figure 6: A clinical photograph of tooth #19 at six months. Probing depths on the mesial aspect of this tooth were less than or equal to 3mm`s.
Would you like to receive continuing education credit for this article?
If so, answer the questions on the quiz at right by filling out the enclosed answer sheet.
- First, carefully tear off the answer sheet along the perforated line. Answer the questions by making a heavy, black mark in the circle next to your choice. Fill out the personal information (name, address, etc.) and the payment options on the front and back of the answer sheet.
- Insert the answer sheet (and check, if that`s your payment option) into the business-reply envelope that`s provided along with the answer sheet.
- If for some reason, the envelope was lost during the mailing process, you can still mail your answers to: SUNY Farmingdale, Office of Continuing Education, 2350 Broadhollow Road, Farmingdale, NY 11735-1021. Questions or comments concerning this article also can be directed to the university.
To receive continuing education credit for reading this article and answering the questions above, please use the answer sheet and business-reply card included with this article. Nine of 12 questions must be answered correctly in order to receive certification for this course..