Health screening
A focus on chronic medical conditions that devastate oral health
by Sonya L. Prater, RDH, BS, FACE
As I see it, the two approaches to health screening are comprehensive and laissez-faire (so to speak). In the past, when I heard the word "screening," I thought of a two-question pop quiz:
- Are there any changes in your health history?
- Are you having any problems with your teeth or gums?
At this point, no one should be surprised by the answer they are about to receive – "No." You might as well be asking them about the weather; you would get more of a response. Unless you have a patient who enjoys being sick and lives to tell you about it (you know those few), the answer will always be, "No." How many times have you heard, "Everything's the same; no changes"? People either don't realize the importance of your knowing their current health status or they just don't want you to know.
Recently, a patient filled out a health update form for me. Granted, this particular form is not designed as an in-depth review of health status; it mainly asks any changes in medications, as well as any changes in the health status since the last appointment. Of course, that two-letter word, "no," was written beside the question. During our conversation at the beginning of the appointment, I found out that he had his first eye exam during the previous month, was diagnosed with glaucoma, and had laser surgery on both eyes – all within two weeks.
What if this had been a total hip replacement – and the patient needed to premedicate – but wasn't previously informed by his physician or us? If I did not take the time to review his health with some level of thoroughness, the appointment could have proven to be fatal. That would be the worst case scenario but I wouldn't even want to put someone in the hospital, much less threaten their very life.
From a more comprehensive point of view, the health screening could last throughout the entire appointment. Even with a series of specific questions, we don't always find out what we need to know – until we look in the mouth. In many cases, the mouth has definitely been the window to the body. Inflammation, bleeding, mouth lesions, acid erosion, and rampant decay are like a secret code. We must dig deeper to find out what is going on.
Overall, we have a pretty educated patient population. They've heard commercials, googled topics, know from personal experience, or have watched the Dr. Oz Show enough to have a fair amount of knowledge about health issues and the impact they have on oral health, and vice versa. Patients are beginning to recognize the link between the mouth and the whole body, but it is taking a great effort on our part as dental professionals to get the word out there.
Here are a few questions to consider when screening your patients:
- What do I need to know?
- Why is it important that I know?
- What is my obligation to the patient?
- What are the educational opportunities (for me and the patient)?
Critically thinking through the appointment aids in thoroughness.
What are the chronic medical conditions?
We have so frequently been exposed to certain medical conditions and medications that we begin accepting a chronic condition as the norm. Is there ever a day that you don't see a patient who is on a blood thinner, cholesterol medication, or a diuretic? I highly doubt it. There are so many chronic medical conditions these days, ranging from the simple to complex. Examples include (but are not limited to) obesity, high blood pressure, high cholesterol, heart disease, diabetes, asthma, and autoimmune diseases. Unfortunately, taking medications for these chronic illnesses may have developed chronic xerostomia.
Xerostomia has very damaging results and yet is the most common side effect of prescription and nonprescription drugs. Decay is widespread among people who have dry mouth. They experience great discomfort and long-term problems. Relief is sought out in mints, cough drops, gum, and beverages. Many times, the products patients choose are sugary, thus adding to the problem. Several products help combat dry mouth, but the only "cure" often seems to be to stop taking the medications, which can't always happen. Many factors are involved with xerostomia – not just medications. Insomnia, systemic diseases, radiation therapy, dehydration, stress, depression, and lack of chewing are all causative factors for dry mouth.
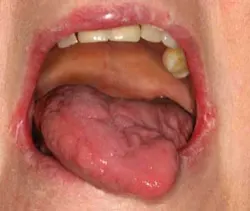
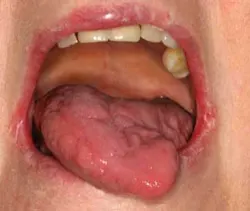
This patient's tongue is a perfect example of how xerostomia can irritate the oral tissues. It has a "beefy" appearance.
Inflammation and bleeding are critical factors during any discussion of diabetes, heart disease, and high blood pressure. Although the systemic link between these conditions and periodontal disease is well known in the dental profession, trying to keep a stable periodontal condition is a challenge. The first step is making sure patients are aware of the systemic link and then coming up with a plan to control the dental disease, which in turn should have a positive effect on their current health condition.
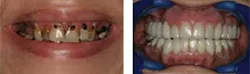
The before-and-after photos illustrate the damage that was done due to effects of Sjogren's syndrome, as well as xerostomia.
One of the best ideas is to have a medical-dental cooperative team – not just a referral system but to have leaders in each field sharing knowledge about case studies and developing a total body wellness plan for the cases. Having a comprehensive view of health could move people from being dental insurance driven, which would allow for more thorough treatment to take place.
Autoimmune diseases
Something I've been exposed to more often are patients with autoimmune diseases. In addition to HIV, patients have autoimmune diseases that many of us remain unfamiliar with, such as rheumatoid arthritis and Sjogren's syndrome. Simply put, the body attacks itself and can be very difficult to control, and without a cure. Strong medications are used with very damaging side effects.
Rheumatoid arthritis and Sjogren's syndrome can many times mimic each other. Depending on the knowledge and experience of the physician, the diseases can take up to 10 years to show up in blood work and be diagnosed. In the meantime, irreversible damage can occur. These diseases attack the mucous membranes, leaving eyes, mouth, and even the skin dry (a mild assessment of symptoms at best).
A 40-year-old British female recently presented with rampant decay and broken and missing teeth. She was a nurse, and her initial complaint was that she didn't like her "black" teeth. She reported good health – a vegetarian who consumed a very limited amount of sugar, if any, and was very athletic – until 2005 when her teeth and health started to decline. There was no sign of any autoimmune disease in her blood work for several years. Finally, based on all of her symptoms, her physician diagnosed her with Sjogren's syndrome.
The disease affected not only her oral condition but all of her mucous membranes, intestines, stomach, eyes, and now her skin. Other medical complications included seizures, muscle spasms, cysts on her ovaries, intestinal issues, overproduction of bile, and daily aches and pain. As a result of her condition, multiple surgeries occurred.
Her daily medications were Klonopin, Singulair, Fentanyl patch, and Nexium. PRN medications were Colestipol, aspirin, tramadol, Tylenol-Codeine #3, and Lydoderm.
The patient informed me that, after moving to the United States, the decline of her oral health had accelerated. Fillings were "popping out" again and crowns were coming off. She was unable to eat properly and was vomiting frequently.
A British dentist recommended she do home fluoride trays two days a week. She was able to do that for three years until she came to the United States. She states with certainty that was how her teeth remained healthy for so long. In 2009, the decay was throughout her entire mouth and uncontrollable. Within one year, her teeth were literally rotting away.
This patient's whole mouth has recently been restored and her dental wellness visits will be at three-month intervals. CariFree products and topical fluoride will be routine for her, and we will adjust products as necessary.
We can slip back into the same routine and chalk the decay up to poor home care or even Mountain Dew in these cases. If we are not committed to getting to the root of the problem, we will let situations like this go ignored.
One reason I enjoyed dental hygiene is that we did not have to take our work home with us. This is a sentiment of the past. I want to find out the when, where, why, how, and the solution when a patient of mine has a question or concern about an issue, or if I detect an unexplained problem. Having a network of referring doctors is helpful in situations like this to discuss signs and symptoms when things just don't seem to add up. Many times we assume that physicians know certain things, and they assume we know certain things.
We have a responsibility to our patients. Getting to the root of the problem, by whatever means necessary, and providing the highest level of care possible should be our focus. It starts with the total body health screening.
Sonya Prater, RDH, BS, FACE, graduated from Western Kentucky University and has been in private practice for 16 years. Having held eight state licenses, she remains in active status in North Carolina, South Carolina and Georgia. She is currently practicing in Savannah, Ga., in a very progressive, customer service driven dental office that specializes in highly complex and reconstructive TMD cases. As a member of the Niche Practice Seminars, she is dedicated to developing a highly specialized program that will raise the bar for dental hygiene as we know it.
Past RDH Issues