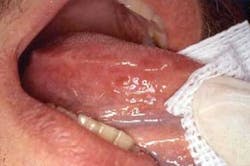
A fighting partner
Dentists and hygienists should be teaming up to be the first line of defense against oral cancer
by Donna Marie Grzegorek, RDH, EC
In the United States this year, more than 35,310 new cases of oral and pharyngeal cancer will be diagnosed, with an estimated 7,590 people who will die. Sadly, survival rates for oral cancer have not changed significantly in 40 years, and embarrassingly, dental professionals are alone among health professionals who screen for cancer with their hands and eyes. Under the watchful eye of the dental practitioner, 70% of the lesions found during visual and palpation exams are detected in Stage III and Stage IV, and one–half of those patients (58%) will survive less than five years. It gets worse ... a survey conducted by the American Dental Association revealed that only 15% of patients reported having an oral cancer examination during a routine dental appointment. And noteworthy, failure to diagnose oral cancer is the number two cause of dental malpractice in the United States. Oral cancer claims constitute the most expensive malpractice suits and the most difficult to defend, with awards typically exceeding $1 million.
If these statistics are not compelling enough, take note that the face of oral cancer is changing. No longer should we look at the older male patient with a chronic history of tobacco and alcohol abuse as the only high–risk patient. Twenty–seven percent of all new oral cancers are occurring in young adults with no associated risk factors. So I ask you ... isn't it time to increase the “standard of care” and incorporate a comprehensive early oral cancer detection program into your office protocol?
Where to begin
I strongly feel that the dental hygienist should be the first line of defense against this insidious disease. The practice act in many states limits the hygienist's ability to diagnose. Therefore, an early oral cancer detection protocol must involve a partnership between the dental hygienist and the dentist.
Several years ago, upon approaching my employer and stating my desire to increase the standard of care we provide to our patients regarding early oral cancer detection, we initiated our program. We discussed the benefits of incorporating an adjunctive blue spectrum light screening technology into our examination. Two weeks later, upon formulating an appropriate protocol, we launched our enhanced oral cancer screening program.
We began our new effort by educating our patient base. The preponderance of the hygiene appointment was dedicated to discussing the risks of oral cancer, reviewing statistics, and performing the visual, palpation, and blue light examination.
It is critical that the patient understand an adjunctive screening device is not a definitive diagnostic device, but rather a means of detecting disease early, in asymptomatic people.
Positive results are not diagnostic. They are a way to identify persons at increased risk for the presence of cancer, which warrants further evaluation. I review medical/dental and lifestyle risks that each patient possesses. This includes conversations regarding HPV and oral sex.
HPV and oral cancer
Human papillomavirus is now recognized to play a role in the pathogenesis of a subset of head and neck squamous cell carcinomas (HNSCCs), particularly those that arise from the lingual and palatine tonsils within the oropharynx. HPV cancers are the fastest growing segment of the oral cancer population. Although there are more than 100 different types of HPV identified, HPV 16, 18, 31, and 45 are sexually transmitted.
According to the U.S. Department of Health and Human Services, HPV is transmitted through skin to skin contact. HPV 16 and 18 are implicated in most cervical cancers and are also responsible for anal and penile cancers. It appears that HPV 16 is identified in the overwhelming majority of HPV positive oral tumors.
It is encouraging to note that HPV positive oral cancers have significantly better survival outcomes than the non–HPV–related tumors. It is believed that the HPV–related tumors are more susceptible and vulnerable to radiation treatments than their tobacco and alcohol counterparts. It has recently become understood that HPV affects the cell's molecular machinery. It interferes with the function of a key gene that would normally cause cells with potentially cancerous mutations to self–destruct.
Given the decline of tobacco use over the past 10 years and the increasing rate of HPV–related oral cancer, much of the blame is cast toward HPV transmission through oral sex. I make it perfectly clear to my patients that “oral sex is not safe sex.”
Foundation takes strong position
The Oral Cancer Foundation has expressed very strongly its position about non–tobacco–related oral cancers. The foundation states: “We strongly believe that in a younger population of nonsmoking oral cancer patients, HPV is presenting itself as the dominant causative factor. Since the historic definition of those who need to be screened is now changed by this newly defined HPV etiology, it is not possible to definitively know who is at risk for development of the disease, and who is not. Today, anyone old enough to have engaged in sexual behaviors which are capable of transferring this very ubiquitous virus needs to be screened annually for oral cancer. For this reason, we are strong promoters of opportunistic annual screenings to catch this disease at its earliest possible stages, when it is most vulnerable to existing treatment modalities and the survival rates are the highest.”
Wow … need I say more?
Every patient should be screened
As clinicians we must remember that patients don't walk into the office carrying a sign that states they are at high risk for oral cancer. Oftentimes patients are not truthful with the information they provide on their medical/dental histories.
With hard statistics showing that 27% of all oral cancers occur in young adults ages 18 to 35 who don't drink and don't smoke, what parameters can we establish to safely screen our patients? The truth is that EVERY patient should be screened for oral cancer.
I perform a comprehensive oral cancer examination during the hygiene visit on each patient age 17 and older at every recare appointment. An identical examination is repeated by the dentist when he completes his portion of the patient examination.
We believe that having two sets of eyes looking for oral cancer is better than one. This protocol has been well– received by our patients. It creates value for the procedure, but most importantly it sends a message of great significance to our patients. We encourage patients to return for a complimentary reexamination if they find any oral lesion that does not resolve in two weeks.
I dispense to each patient a “self examination” visual and palpation instruction sheet. I encourage self–examination of the head and neck on a monthly basis and compare the process to breast self–examination.
Up your game
I assert that any adjunctive screening device will enhance the office “standard of care,” and improve patient health outcomes. Complete your research and choose the methodology that provides the best fit for you, your patients, and your practice. I recommend not offering the oral cancer examination as if it were an option. Present a compelling argument through education and discussion so the patient thanks you for being one of the few offices that offer such a valuable service.
I believe dental hygienists must partner with their supervising dentists to create an effective early detection protocol. The dental professional is the first line of defense against this menacing disease. Together we can make a difference. In the past 29 years, I have observed the profession of dental hygiene mature from one of mechanical tooth debridement to one of veritable health–care provider. We have a unique opportunity and a critical responsibility to counsel our patients on the importance of living healthier lives through meticulous oral health care. It's wonderful to save a tooth, but as dental health–care providers in 2009, we have many opportunities to save lives.