Actisite® (tetracycline hydrochloride) and the Recare Patient
Part I: The role of the dental hygienist in Actisite® Treatment
Stephen Candio, DDS
One of the major challenges of modern dentistry has been to design effective therapies for the control of adult periodontitis. Because periodontitis is a chronic condition, treatment is traditionally an ongoing team effort in which the dental hygienist plays an important role. In fact, because the hygienist usually performs the initial preventive and therapeutic treatment as well as the ongoing maintenance and recare therapy, the hygienist often develops a high level of trust and rapport with the patient. Therefore, it is important that the dental hygienist, as part of the dental team, continues to be aware of emerging technologies in order to provide optimum care. One such treatment option is Actisite® (tetracycline hydrochloride) periodontal fiber, a 10-day site-specific course of antibiotic periodontal therapy which is used as an adjunct to scaling and root planing. This article will provide a general introduction to the hygienist`s role in Actisite® treatment. Part II will offer detailed practical approaches to Actisite® use, including sample answers to typical questions patients ask about therapy.
Overview of Periodontitis Treatment
It is important to remember that first and foremost, Actisite® is designed to provide an additional periodontal therapy option. Over the past decades, treatment for periodontitis has primarily consisted of plaque control and scaling and root planing, augmented in more severe cases by periodontal surgery to reduce or eliminate pathological periodontal pockets. These widely accepted therapies provide long-term stability in many patients; however, recurrence and progression of the disease are not uncommon.1 In fact, periodontal disease remains a major cause of tooth loss in the United States.2,3
Another conservative treatment option for adult periodontitis is the use of antibiotic agents in combination with scaling and root planing to control the bacterial pathogens in the crevicular pockets.4 In particular, tetracycline has demonstrated a high degree of bacteriostatic activity against the anaerobic bacteria thought to cause periodontal disease5-7 and has been shown to have beneficial effects on the clinical parameters of the disease when administered orally (systematically) in adults with refractory periodontitis. However, systemic use is limited by difficulty of achieving and maintaining therapeutic concentrations of the antibiotic in the crevicular fluid and by its association with side effects.4 Additional local delivery methods of administering antibiotics (including mouthwashes and subgingival irrigation) have also been investigated, but these techniques have limited effectiveness due to the difficulty of maintaining a therapeutic level of the antibiotic in the crevicular fluid over time.3, 7-8
Actisite® Periodontal Fiber
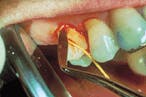
In 1994, a method of delivering tetracycline directly to the site of periodontal disease became available to the general dental professional, Actisite® (tetracycline hydrochloride) periodontal fiber. Manufactured and marketed by the Procter and Gamble/Alza Partnership, Actisite® (Figure 1) is a flexible polymer fiber impregnated with 12.7 mg tetracycline hydrochloride, which is released continuously over a period of 10 days.9 In Actisite® treatment, the fiber is placed into the affected gingival pocket (Figures 2 and 3), and secured by an adhesive. After the 10-day treatment period, the patient returns and the Actisite® fiber is removed.
Actisite® treatment is indicated as an adjunctive therapy to scaling and root planing for reduction of pocket depth and bleeding on probing in patients with adult periodontitis.10-12 Actisite® delivers a continuous local concentration of tetracycline to the individual pockets for a specific therapeutic length of time, with little systemic exposure.13-14 In pivotal clinical studies,15-17 the most common adverse events associated with the use of Actisite® were discomfort on fiber placement (10%) and local erythema following removal (11%).
Because of its benefits and ease of use, I believe that Actisite® will become a part of many practitioners` routine approach to the control of periodontal disease. It is equally evident that the dental hygienist will have an important role in helping the dentist create a comprehensive treatment regimen for Actisite® patients. This article will review some ways in which the hygienist may participate in Actisite® treatment and some influences that Actisite® is likely to have on how dentists and hygienists approach periodontal disease in the future.
The Hygienist`s Role in Actisite® Treatment Identification of Candidates for Actisite® Treatment
One of the major roles of the dental hygienist in the use of Actisite® is, clearly, to aid the dentist in identifying candidates for this site-specific antibiotic therapy. As in most practices, in our office the hygienist typically spends 45 to 60 minutes with the recare/maintenance patient in conjunction with the dentist, who spends 10 minutes performing the periodic examination. Information gathered by the hygienist through probing sulcus depths, scaling and planing, and polishing then becomes the basis for discussion between dentist and hygienist regarding the next phase of periodontal treatment. Following this type of procedure will greatly aid the dentist, who can use the hygienist`s recommendations to immediately concentrate on the "trouble spots" found by the hygienist, thus making the most productive use of the dentist`s time with the recare patient.
An office practice that takes advantage of the hygienist`s perspectives on any given patient is to structure the consultation between dentist and hygienist as a two-part procedure: First the hygienist and dentist discuss the results of the screening examination privately. Then both return to the examination room where the dentist will ask the hygienist "what did you find" in the patient`s presence. Since, in this scenario, the hygienist will already have explained the concern and potential treatment options to the patient, the patient hears this information for a second time from the dentist. This reinforces the initial emphasis on the patient`s dental disease and treatment.
Identifying candidates for Actisite® is an easy task to add to the hygienist`s normal screening and treatment regimen, and it is recommended that hygienists and dentists discuss in advance specific parameters the dentist would want identified for Actisite® use. In general, however, sites that are good candidates for Actisite® treatment exhibit the same "danger signs" that hygienists typically look for in any periodontal maintenance patient. These include increased pocket depth (Actisite® is recommended for use in pockets of 5 mm or greater depth) and/or bleeding on probing, especially in sites where prior charting showed the teeth to be within normal limits. These are all indications that the patient is having difficulty maintaining optimum health at these sites, and these are the types of locations that the hygienist would generally note and bring to the attention of the dentist.
Patient Education
Another very important role of the hygienist is to assist in educating the patient about periodontal disease in general and Actisite® treatment in particular. Although treatment of infections with antibiotics is expected in medicine, it is not a well-known treatment for the control of recurrent, localized site-specific periodontal disease. Therefore, Actisite® treatment will represent a change for most dental patients, and in order to accept it, they will require more education about periodontal disease and its treatment. Because of the structure of the recare/maintenance appointment previously discussed, the hygienist will be a critical participant in this effort. Here are some key features of such an enhanced education effort:
Because of the painless nature of many periodontal problems and because most patients see dental treatment as consisting mainly of mechanical procedures (cleaning, fillings, etc.), it is important to introduce the concept of dental disease when a "problem spot" is discovered. Important points to include are the general nature of the periodontal disease process, how it is site-specific and episodic. Furthermore, it is important to stress that periodontal disease is generally a painless, chronic condition that causes few patient-observable symptoms in its early stages, but can cause permanent damage if left untreated. Here again, drawing a comparison to a medical condition such as high blood pressure where early symptoms may many times go unnoticed until the disease is well advanced can be very helpful in establishing the nature of periodontal disease.
Once the patient understands the nature of the problem, the hygienist can next discuss various treatment modalities with the patient - for example, scaling and root planing or scaling and root planing followed by Actisite®. One way to introduce this discussion is to tell the patient that you have discovered an area showing warning signs of periodontal disease, and that the dentist may feel that the problem area is an appropriate area for treatment with Actisite®, a site-specific antibiotic therapy. Other points that can be made about Actisite® include that it is easy, relatively painless, can be performed in the dentist`s office, is not invasive, and may mean that the need for additional procedures may be reduced.
As in the discussion of any periodontal therapy, it must be stressed that the disease requires constant reevaluation, and Actisite® is one of several options. The best approach is to present Actisite® as an effective adjunctive treatment that is one of the most conservative (i..e., relatively painless, non-invasive) ways to treat this condition.
In talking with patients who seem very resistant or apprehensive to periodontal therapy, it is often helpful to make a statement that reinforces the fact that Actisite® treatment is similar to taking antibiotics. Presented in this light, most patients are very open to Actisite® treatment, and we have found that even hesitant patients generally want to begin treatment immediately.
This type of patient education during the recare/maintenance appointment with the hygienist reinforces several key elements leading to therapy. First it informs the patient of the problem and educates (or reminds) the patient that periodontal disease is an infection, and that treatments are available. It shows that the condition is serious enough that both the hygienist and dentist are concerned and want to consider timely intervention. And finally, it can encourage patients to comply with recommended treatment.
After proper introduction by the hygienist, the dentist`s diagnosis and suggestion for treatment will have the force of a second opinion without the patient even leaving the office. Speaking as a practicing dentist, I know that it is much easier to ensure the patient receives the needed treatment when the hygienist has properly prepared the patient before I complete the examination. In this regard, the hygienist can be instrumental in ensuring the patient receives appropriate treatment.
The Follow-Up Visit
Following scaling and root planing, the patient should return within approximately 3 weeks for follow-up evaluation. This 3-week interval will give the dentist and hygienist the opportunity to reevaluate the tissue response, evaluate the effectiveness of the patient`s oral home care, and reinforce its importance. The examination may include probing the previously charted areas and evaluating the health (or non-health) of these locations. Based on these findings, the dentist can make the final decision on treatment.
If the clinical indications for Actisite® therapy (pocket(s) ≥ 5 mm and bleeding on probing) remain at this 3-week follow-up, the patient - already understanding the possible need for adjunctive therapy - can be scheduled for an appointment for Actisite® placement, in accordance with office practice.
If, on the other hand, evidence of tissue inflammation is no longer present, no further treatment is indicated at this time. The hygienist can explain the situation to the patient by saying that the suspect areas have healed for the time being. However, it should also be stressed at this time that because periodontal disease is a chronic and recurrent disease, close monitoring of the inflamed site (and all teeth) will be made when the patient returns for recare appointments at the office-recommended intervals. Should the clinical signs of an unstable situation return in the future, appropriate therapy (including Actisite® treatment) can again be considered.
Actisite® Placement and Removal
The duties of the dental hygienist in the placement and removal of the fibers will be determined to large extent by what is permitted by each state`s dental practice act. In states where hygienists are allowed to do placement and removal, the techniques will generally be learned by the same means currently available to dentists. Detailed discussion of such techniques is beyond the scope of this article, but generally speaking, placing Actisite® is very similar to placing retraction cord. The technique is fully demonstrated in the instructional video that accompanies the Actisite® product and discussed at length elsewhere in the literature.10, 12, 18-19
Conclusion
The availability of Actisite® periodontal fiber has given dental practitioners an additional weapon in the continuing fight against periodontal disease. Because Actisite® is a non-invasive therapy that is recommended as an adjunct to scaling and root planing for use in patients with recurrent adult periodontitis, its use in the general practice environment calls for a coordinated effort between dentists and hygienists in evaluating candidates for treatment, administering treatment, and following up on a long term basis. In most practices, hygienists will be instrumental in implementing these efforts and in ensuring their success.
An important element in this effort is an ongoing dialogue among dentist, hygienist, and staff concerning the treatment of localized periodontitis. This will help ensure a unified attitude towards Actisite® treatment that will, in turn, encourage proper compliance with Actisite® therapy and will lead appropriate candidates to take advantage of this adjunctive periodontal treatment for site-specific adult periodontitis.
Please see accompanying brief summary of side effects and contraindications.
References
1. Ramford S, Caffassee RG, et al. 4 modalities of periodontal treatment compared over 5 years. J Clin Periodontol 1987; 14:445-452.
2. McFall WT Jr. Tooth loss in 100 treated patients with periodontal disease. A long-term study. J Periodontol 1982; 53-539-549.
3. Lindhe J, Nyman S. Long-term maintenance of patients treated for advanced periodontal disease. J Clin Periodontol 1984; 11:504-514.
4. Goodson JM. Antimicrobial strategies for treatment of periodontal diseases. Periodontology 2000 1994; 5:142-168.
5. Baker PJ, Evans RT, Slots J, Genco RJ. Susceptibility of human oral anaerobic bacteria to antibiotics suitable for topical use. J Clin Periodontol 1985 12:201-8.
6. Alfant M, Walker CB, Bashkar P. Local delivery of tetracycline as possible adjunct to conventional periodontal therapy. (Abstract no. 1083). J Dent Res 1983; 62:289.
7. Silverstein L, Bissada N, Manouchehehr-Pour M, Greenwell H. Clinical and microbiologic effects of local tetracycline irrigation on periodontitis. J Periodontol 1988; 59:301-5.
8. Christersson LA, Norderyd OM, Puchalsky CS. Topical application of tetracycline-HCI in human periodontitis. J Clin Periodontol 1993; 20:88-95.
9. Tonetti M, Cugini MA, Goodson JM. Zero-order delivery with periodontal placement of tetracycline-loaded ethylene vinyl acetate fibers. J Periodontol Res 1990; 25:243-9.
10. Killoy WJ, Cobb CM. Controlled local delivery of tetracycline in the treatment of periodontitis. Compend Contin Educ Dent 1994, XIII; 12:1150-1160.
11. FDA clears tetracycline periodontal fiber for marketing. Biological Therapies in Dentistry. Vol. 10, July 1994.
12. Tonetti MS, Giovanpaolo Pini-Prato, Cortellini P. Principles and clinical applications of periodontal controlled drug delivery with tetracycline fibers. Int J Periodont Rest Dent 1994; 14:421-435.
13. Rapley Jr, Cobb CM, Killoy WJ, Williams DR. Serum levels of tetracycline during treatment with tetracycline-containing fibers. J Periodontol 1992; 63:817-820.
14. Ciancio SG, Cobb CM, Leung M. Tissue concentration and localization of tetracycline following site-specific tetracycline fiber therapy. J Periodontol 1991; 63:849-853.
15. Newman MG, Kornman KS, Doherty FM. A 6-month multi-center evaluation of adjunctive tetracycline fiber therapy used in conjunction with scaling and root planing in maintenance patients: Clinical results. J Periodontol 1994; 65:685-691.
16. Goodson JM, et al. Multicenter evaluation of tetracycline fiber therapy: II Clinical response. J Periodont Res 1991; 26:371-379.
17. Clinical studies support safety and efficacy of Actisite periodontal fiber. Biological Therapies in Dentistry. Decker Periodicals, 1994.
18. Thompson DM. Actisite: Site-specific sustained-release periodontal therapy. Dental Econ; February 1995:98-99.
19. Dental Rx. Placement of Actisite tetracycline-impregnated fiber to treat adult periodontitis by Procter & Gamble/ALZA. Dent Prod Report; Vol 29, No 2:15.
Figure 1: Actisite® tetracycline-impregnated periodontal fiber.
Figure 2: Schematic drawing of the application sequence of Actisite® fiber (left to right).
Figure 3: Clinical illustration of the application of Actisite® fiber.