Erythema multiforme
Presentation: A 20-year-old male is scheduled for his six-month maintenance appointment. He takes no medications, is a college athlete, and has no health concerns.
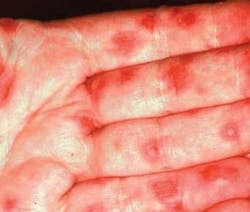
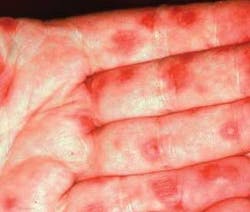
Notes and findings: The patient presents with evident lesions on the palms of his hands and has obvious oral inflammation. The patient reports noticing the lesions first on the palms and later developing the ulcerative oral lesions that have been present for several days. The lesions on the hands, as seen in Figure 1, have a “bulls-eye” appearance.
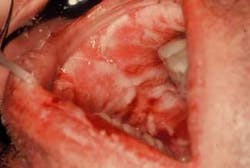
The oral lesions (Figure 2) have an aphthous-like appearance and are superficially distributed throughout the oral tissues. He also reports pain and a slight fever. His lymph nodes are indurated, mobile, and tender when palpated (lymphadenopathy).
Diagnosis: Erythema multiforme (multi-varied appearances)
Clinical impressions: The skin lesions in erythema multiforme present as erythematous papules, which enlarge to form central vesicles, or bullae, creating what is referred to as “iris,” “target,” or “bull’s eye” lesions. Target lesions usually appear on skin surfaces and the oral lesions usually have an ulcerative type appearance. The lips, buccal mucosa, palate, and tongue are the sites most frequently affected. Depending upon the severity of the condition, the patient may have both skin and oral lesions.
Oral and perioral features: The skin may have a central, dark-red zone bordered by a blanched halo with an erythematous zone at the periphery. When vesicles and bullae are present both with cutaneous and oral lesions, the course of the disorder is considered more severe. Oral lesions are reported in a range of approximately 50 percent of cases. Sometimes lesions are confined just to the oral tissues. The disease is termed minor and major erythema multiforme.
In the more severe cases, the disorder is termed Stevens-Johnson syndrome. This severe form may involve ulcerative lesions of the skin, the perioral areas, genitals, conjunctiva and oral tissue with crusting, and necrosis. A mortality rate of 5 to 15 percent has been reported with Stevens-Johnson syndrome.
Transmission: Erythema multiforme has been associated with the herpes simplex virus, mycoplasma, tuberculosis, and histoplasmosis; however, in many instances, the direct association is not substantiated since many individuals do not know if they were exposed to certain bacteria or viruses.
The use of medications is also associated with erythema multiforme, including sulfonamides, penicillin, barbiturates, phenylbutazone, and phenytoin. Erythema multiforme is believed to be a combination of humoral and delayed-type hypersensitivity mechanisms.
Significant microscopic features: Histological findings include epithelial hyperplasia, spongiosis, vesicles, and lymphocytic infiltrate. Necrotic keratinocytes and extensive vesicular changes are seen within the specimen.
Treatment: In the more severe type of erythema multiforme, Steven-Johnson’s syndrome, the patient may be at high risk of complications and this can be life threatening. In severe cases, systemic corticosteroids are recommended and topical corticosteroids for the oral conditions as well. Recurrence is reported in 25 percent of cases. Liquid diets are frequently necessary. For the less severe cases, erythema multiforme lesions subside after two to six weeks and are self-limiting and palliative treatment is suggested.
Differential diagnosis: The diagnosis is based on the clinical appearance and the absence of other symptoms, but some histological tests may be performed. Patient symptoms vary with severity and may include headaches, lymphadenopathy, and fever.
Confusion sometimes occurs with the following disease states: