MRSA - An Increasing Infection Prevention Issue
by Mary Govonni, CDA, RDH, MBA
According to the Centers for Disease Control and Prevention, methicillin-resistant Staphylococcus aureus (MRSA) infections are becoming more and more common. MRSA is a type of staph infection that has acquired resistance to many common antibiotics. These infections can be very contagious and difficult to treat. MRSA occurs in two forms: hospital-associated and community-associated. In October, a high school student in Virginia died as a result of a MRSA infection. This prompted a district-wide shut down of the schools, in order to disinfect facilities and to evaluate protocols to prevent further outbreaks of infection.
Hospital-associated or -acquired MRSA infections occur not only in hospitals, but also in long-term-care facilities/nursing homes, dialysis centers, and other outpatient care facilities. Modes of transmission include urinary catheters, surgical procedures, and dialysis ports. Patients who contract these infections are usually those with compromised immune systems.
Community-associated MRSA infections are those that are acquired outside of hospital settings - in public places such as gyms, athletic facilities, day care centers, and other public areas. These infections typically result from contact with the contaminated hands of individuals who are carriers and/or have active infections.
What is important to know about MRSA?
Staphylococcus aureus or “staph” bacteria commonly live on the skin. They also colonize in the nasal passages of about a third of the population of the United States. The bacteria live harmlessly on the skin or the mucous membranes of the nasal passages. If the bacteria enter the body through cuts or sores, however, a serious, potentially life-threatening infection can occur. These infections include cellulitis, endocarditis, pneumonia, bacteremia or blood poisoning, and toxic shock syndrome, which can ultimately lead to organ failure and death. Less serious infections can also occur but do require medical intervention.
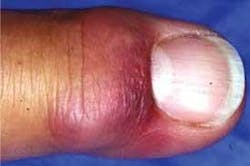
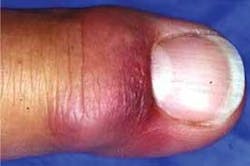
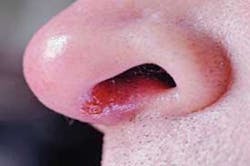
Individuals with active MRSA infections may have red, swollen, painful areas on the skin (sometimes mistaken for insect bites), boils or pimples filled with pus, blisters filled with fluid, or a rash. An individual experiencing these symptoms should immediately cover the affected area with a bandage and seek medical attention. Antibiotic therapy to treat these resistant infections is limited to a few drugs, such as Vancomycin, although some staph infections are resistant to that drug as well. Taking the entire antibiotic prescription as directed is extremely important in these cases to avoid creating an even more resistant infection.
Skin-to-skin contact is the most common method of transmission for MRSA infections. Typical contacts might include touching objects in public areas such as doorknobs or telephones, using equipment at a gym, or sharing personal items such as towels or razors. Contacting these surfaces that might be contaminated with staph bacteria and then touching your eyes, nose, or mouth can cause you to be infected or colonized with MRSA. Being colonized doesn’t necessarily lead to active infection. In fact, many cases of MRSA infection are asymptomatic.
Individuals who are known to be carriers of MRSA must take precautions to prevent the spread of their infection to others, including pets. Pets can also be carriers of MRSA and have active infections. If your pet shows signs of skin infection, contact your veterinarian.
The CDC recommends specific personal care guidelines to prevent contracting or spreading MRSA. These include:
- Wash hands frequently.
- Carry alcohol hand sanitizer for hand washing when soap and water are not available.
- Keep fingernails short to facilitate cleaning and preventing bacteria from growing under nails.
- Avoid sharing towels, razors, toothbrushes, or other personal items (e.g., makeup).
- Change sheets and towels regularly.
- If a cut or scrape on the skin occurs, clean the wound with soap and water and cover with a bandage.
- Get medical attention at the first sign of infection in a cut, such as redness, swelling, pain, or pus.
- Inform health-care providers if you have had an MRSA infection in the past.
For more information about MRSA, these are some helpful Web sites:
- www.cdc.gov
- www.mayoclinic.com/health/mrsa
- www.webmd.com
- www.goapic.org/MRSA.htm
- www.pets-mrsa.com
There are also Web site support groups for individuals who have MRSA. A great deal of research is available online regarding treatment and prevention of MRSA.
As frontline health-care providers, you may come in contact with patients who have MRSA infections. If your practice or facility is following appropriate standard precautions as recommended by the CDC, the risk of transmission of MRSA in a dental setting is minimal. Surface disinfectants typically used in dental settings have been tested for effectiveness against Staphylococcus aureus on environmental surfaces. Sterilization methods are also effective in killing the bacteria on instruments. Hand washing is, of course, one of the most important and effective preventive measures. Always remember that washing hands after removing gloves helps to reduce the possible contamination that may have occurred through micro tears in the gloves during use.
Since many individuals have the bacteria in their nasal passages, pay close attention to the care of nitrous oxide masks. Using masks that can withstand heat sterilization or using disposable masks or liners in the masks would be preferable to wiping the mask with surface disinfectants.
From an infection control/prevention standpoint, it is not necessary to do anything different or extra for patients who indicate that they have MRSA, just as it isn’t necessary with patients who have HIV/AIDS or hepatitis. If a patient has a suspicious-looking skin lesion, it would be prudent to ask if he or she has had a medical evaluation. If not, urge the patient to do so, and explain the possibilities of MRSA infection. If the lesion is uncovered, you may want to encourage the patient to cover the lesion with a bandage for their protection and that of others.
As with all infectious disease threats, education and information are the best tools for prevention. Be aware of this increasing problem and consider providing educational materials (available from the CDC) in your facility to raise your patients’ level of awareness. And, as always, wash your hands
About the Author
Mary Govoni, CDA, RDH, MBA, is the owner of Clinical Dynamics, a consulting company based in Michigan. She is a member of the Organization for Safety and Asepsis Procedures and is a featured speaker on the ADA Seminar Series. She also writes a column for Dental Office magazine. She can be contacted at [email protected].