Oral Lichen Planus And Coping With Stress
by NANCY W. BURKHART, BSDH, EdD, RDH
Consider reading: Damage caused by lip sucking
http://www.rdhmag.com/articles/print/volume-32/issue-11/features/lip-damage-from-sucking-on-tissue.html
Consider reading: Periapical cemento-osseous dysplasia
http://www.rdhmag.com/articles/print/volume-32/issue-2/columns/periapical-cemento-osseous-dyplasia.html
Consider reading: Do you remember the glands of Blandin and Nuhn?
http://www.rdhmag.com/articles/print/volume-32/issue-5/columns/do-you-remembfer-the-glands-of-blandin-and-nuhn.html
Your patient today is a 62 year-old female, Abby, who is a regular maintenance patient in your practice, and she has been suffering with oral and cutaneous lichen planus for many years. She is complaining of burning in the mouth and intensely pruritic sensations all over her arms and legs. As you examine her extremities, you notice the purple, polygonal, pruritic plaques (the four P’s of lichen planus) on most surfaces.
She tells you that the “itchy” feeling began several days ago, and it has gone from “bad to worse.” She also says that her life has been recently stressful with a parent who is seriously ill, a troubled marriage, parenting two school-age children, and a job she dislikes. She comments that administering to all of these tasks has become very emotionally draining.
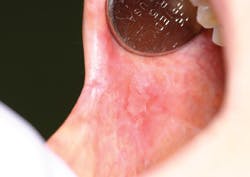
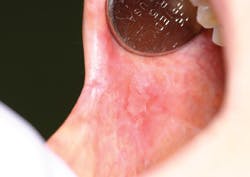
As you analyze her condition, you imagine how difficult it must be for her while dealing with all of the problems she is trying to cope with in her life. Could she be suffering from the ramifications of chronic stress in relation to the oral and cutaneous lichen planus? Figure 1 is an oral view of the erosive lichen planus that is observed.
The information below is designed to assist the dental practitioner who would like to provide some sound advice that may help anyone stay healthier, but especially those patients who are presenting with increased disease states and have obvious chronic stressful events in their lives. RDH
Oral Lichen Planus and Stress
Please use the educational material as a handout for your patients.
Why worry about your stress level?
What connection could your state of health have to do with stress?
You have lichen planus and this disorder is from an unknown cause?
You say that you are not stressed?
The type of stress that is detrimental to health is termed “unmanaged stress.” Stress is universal, and we all handle it in different ways. What is stress to one person may be more of a positive challenge to someone else. When the sympathetic nervous system is in a state of chronic arousal, the body may reach what is termed an “allostatic load” status. At an undetermined point — and this is different for each of us — there is sheer overload in handling and processing the chronic stress and its cumulative effect upon all organs/systems of the body.
Researchers have reported that one of the most detrimental types of stressors are those that make the person feel they have no control with minor and major issues in their lives. The effects of stress may be much worse when a person believes that whatever steps they take will not make a difference in their personal outcomes.
Sometimes these factors are job-related pressures, family pressures, or health related issues that are already in play. Situations involving severe, unresolved grief and loss will promote a long-term chronic type of stress. Losses come in many different forms such as the death of a loved one, loss of a loved one’s identity through disease states such as Alzheimer’s disease that may last for years, the loss of pets, divorce, the loss of a body part, the loss of one’s identity or possibly even the loss of a home that was part of one’s identity. With economic issues, the loss of property and jobs has become a major player in stress and its effect on the body. Often, the identity of the person is associated with their profession or with the possessions that they have accumulated in life.
Stress can have profound effects on all cells, tissues, organs and systems of the body. Some of the diseases and disorders that have been suggested are heart disease, hypertension, immune suppression, gastrointestinal disorders, anxiety disorders, certain cancers, low back pain, skin disorders, and general declines in health. The suggested cancers may be lifestyle related.
- Start a journal. Writing brings your observations into focus. Additionally, writing is a stress-reducer on its own, which promotes a sense of well-being. Record your reactions to everyday events. For patients with chronic and intermittent diseases such as lichen planus, a chronicle of daily events, foods consumed, and anything that you come in contact with through the environment should be documented. When an outbreak occurs, you can begin to assess a connection that might be meaningful to you. Patients who have oral lichen planus often report trigger mechanisms that occur before an outbreak of the lesions.
- Observe any patterns in your own life. Begin to review your journal periodically and observe items that do not promote a sense of well being for you. These may be activities, people in your life that may be causing you undue stress, and continued thoughts of past events that may not have been beneficial for you (termed rumination).
- Observe patterns that promote relaxation. What events bring you pleasure? When do you feel really good in what you are doing with your life? What people lift your spirits
- How do you view changes in your life (both small and significant changes)? Results from studies indicate that individuals who view change as a life-challenge are in most cases somewhat resilient to adversity, have what is termed “hardiness,” and generally stay healthier. Additional studies have reported that patients who have “persistence” as a characteristic trait in everyday life tend to remain healthier as well. Many of these traits also belong to centenarians.
- Do you see the glass as half full or half empty? Individuals who are optimistic rather than pessimistic are more resilient and are able to cope with stress more favorably. Optimism, it is believed, can be learned. Again, this is another trait of the centenarian.
- Make a plan to develop more appropriate coping strategies! Develop ways that assist you in either confronting harmful events, people or habits, and/or avoiding the situations that place you in these events or with people who do not add to your sense of well-being. Sometimes, simply recognizing what is taking place with your body when negative events occur may be all that is needed. Professional counseling may also assist in a long-term strategic plan as well.
Although it is true that we do not know the cause of lichen planus, most practitioners and patients with lichen planus will tell you that they can document the development of lesions when their stress levels increase.
Mason differentiated between the arousal of the sympathetic adrenal-medullary system by the fight-flight response (based on work by Selye) and the pituitary adrenocortical response. It has been documented that if the sympathetic adrenal-medullary system is activated excessively, persistently, and too often, illness and disease may occur. The release of catecholamines and epinephrine by the adrenal medulla and/or sympathetic nerve endings is believed to induce many of the pathological states associated with psychological stress: increased blood pressure, cardiac arrhythmias, and sudden death. Adverse life events have also been documented as occurring before the onset of functional abdominal pain, alopecia areata, headaches, cancer, heart disease, low back pain, and psoriasis.
Stress and stress-related illnesses have been studied extensively in the last 30 years. The results clearly indicate that stress, especially chronic stress, has profound effects on the body. The well-known Framingham, Mass., Heart Study identified the Type A personality and associated it with a doubling of the risk of coronary heart disease in men and women. Animals subjected to repeated stress show significant decreases in the total number of mononuclear cells, especially T cells, in the spleen and blood.
Acute stress has the ability to enhance the response of the immune system while chronic stress has a tendency to suppress the immune system. Chronic stress can cause a reduction in mitogenesis, alterations in lymphocytes, reductions in the ratio of T-helper cells to T-suppressor cells, and a decrease in the number of natural killer cells needed for defense. McEwen (2002) states that normal levels of stress hormones enhance the immune response, but if the stress response is repeatedly overactivated or prolonged, immune function is impaired. The body needs a balance of allostasis (maintaining stability) and a lower chance of allostatic load (resulting in too much stress).
Life events that produce chronic stress have been shown to have a wide range of effects on the body. Recently, a major emphasis has been placed on the patient’s ability to cope with the chronic stressors of daily life. Coping skills can be developed and learned. If this is a factor for you, seeing someone who can help you make a plan to increase your coping skill repertoire will help. RDH
Suggested Reading for Patients
- Buettner D. Blue Zones. National Geographic Society. Washington DC. 2008.
- Campbell TC, Campbell TM II. The China Study. BenBella Books, Inc. Dallas, Texas. 2006.
- Mate G. When the body says NO. John Wiley & Sons, Inc. Hoboken, New Jersey. 2003
- McEwen B. The end of stress as we know it. Joseph Henry Press, Washington D.C. 2002.
- Perls TT, Silver MH. Living to be 100. Basic Books, New York, New York. 1999.
- Sapolsky RM. Why zebras don’t get ulcers: a guide to stress, stress-related diseases and coping. W.H. Freeman and Company, New York. 1997.
- Seligman M. Learned Optimism. Pocket Books, New York, New York. 1990.
NANCY W. BURKHART, BSDH, EdD, is an adjunct associate professor in the department of periodontics, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (http://bcdwp.web.tamhsc.edu/iolpdallas/) and coauthor of General and Oral Pathology for the Dental Hygienist. She was a 2006 Crest/ADHA award winner. She is a 2012 Mentor of Distinction through Philips Oral Healthcare and Pennwell Corp. Her website for seminars on mucosal diseases, oral cancer, and oral pathology topics is www.nancywburkhart.com.
Past RDH Issues