When is the appropriate time to refer to a periodontist?
Dear Dianne,
My question is about a specific periodontal patient and follow-up treatment. My doctor and I do not always agree, but I’m trying to be as thorough as possible.
The patient in question had definitive periodontal treatment at a periodontist’s office, after which she returned to our office for routine cleanings. We noticed (after several visits) that there is a pocket remaining that is visible on the x-ray at No. 30 with calculus present at the base of the pocket. There is no bleeding, and probing reveals a 3 mm pocket. The patient started out with 4 mm to 8 mm pockets in general prior to treatment.
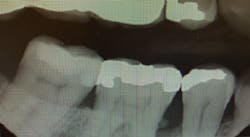
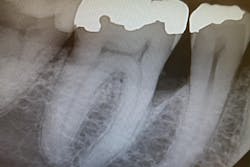
From the x-ray, it appears to be rather deep. [See figures 1 and 2.] Is it common or possible for tissue to reattach above the calculus level where the root surface is clean and smooth, giving the clinical appearance of a healthy area? I worked in a periodontist’s office for quite a few years and saw numerous false readings from reattached tissue versus reading the film.
The patient does not want to return to the specialist. How successful can a hygienist be performing scaling on an 8 mm to 10 mm pocket?
My employer has instructed me to go right ahead and scale that deeply, and then place a PerioChip. My thoughts were to bring the patient back at another date, anesthetize her, and then attempt to reach the depth of the pocket. My personal belief is that pockets over 6 mm are not within the realm of a general dentistry office and should be referred out. In this particular case, I think we need a different periodontist.
I believe that calculus is not always removed completely by Cavitron scaling alone and needs thorough hand scaling as well. I’ve heard different speakers question the value in doing a gross debridement, which allows tissue healing above the deeper calculus if the patient does not return within several weeks to complete treatment. What are your thoughts on that? My employer is telling me that Cavitron, not hand scaling, is the way to go now. I agree about removing biofilm with the Cavitron, but I also feel that hand scaling still has a beneficial use.
Sincerely,
Samantha, RDH
Dear Samantha,
This one is strange. When I view the radiograph, the accretion does not look like typical calculus. There appears to be some space under the deposit, and it is quite large. Also, there appears to be a small piece of calculus remaining on the 2015 radiograph. Since soft tissue cannot be seen on a radiograph and the probing is only 3 mm, I would guess that the tissue has closed over whatever this accretion is, or the calculus is impeding probe positioning to the base of the sulcus.
You asked a great question regarding closed debridement of deep pockets and thorough removal of calculus. According to a study by Drisko and Killoy, anywhere from 17% to 64% of calculus remains after scaling and root planing. Even after surgical intervention, from 7% to 24% of calculus remains.1
A periodontist once shared with me that even after a flap is laid, he sometimes could not remove all of the calculus, even with a handpiece and bur, without doing irreparable damage to the tooth root because the calculus is so deeply embedded in the cementum.
I believe our success in calculus removal goes down when the pocket is more than 6 mm deep, and several studies confirm that. A study by Rabbani et al. demonstrated “a high correlation between percent of residual calculus and pocket depth. It was shown that pockets less than 3 mm were the easiest sites for scaling and root planing. Pocket depths between 3 to 5 mm were more difficult to scale and pockets deeper than 5 mm were the most difficult. Tooth type did not influence the results.”2
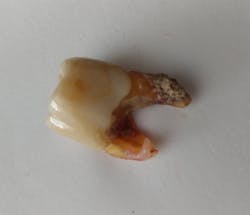
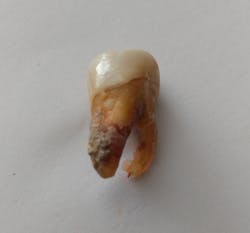
Your question hits very close to home, as my husband recently lost No. 3 due to periodontal infection and deep calculus (figure 3). This tooth previously had a lingual root amputation, endodontics, and a crown in 2009. There is no way a hygienist could have removed all of the calculus from this root surface. The only way would have been through surgical intervention. (And yes, he has been on three-month alternating care between his general dentist and a periodontist.)
Moolya et al. demonstrated viable organisms residing in calculus. Therefore, the incomplete removal of calculus results in incomplete removal of disease-causing microbes.3
I agree with your position that the best and most thorough approach to pocket debridement is by using a combination of hand and power scaling. Both modalities have their place in active treatment. Certain long-shank curettes will fit into tight areas, whereas power scalers allow for light touch and the delivery of medicaments while scaling that can be beneficial for the patient.
Since we have to accept that complete calculus removal is not always possible, we should make use of various other adjuncts that help with microbial control. First on my list is the use of the dental endoscope, which allows the clinician to see inside the pocket and remove residual calculus. Another tool in microbial control is the use of a laser, which uses heat energy to reduce pathogens. There are a number of very good chemotherapeutic approaches to eradicate pathogens. One that I recommend is called ioRinse (iotechinternational.com). It is a unique molecular iodine product that is nonstaining and has a pleasant taste without a detectable iodine taste. It is many times more effective than other forms of iodine, extremely safe, and does not cause microbial resistance (like chlorhexidine does). This product is arguably the most powerful mouth rinse available today as it kills bacteria, viruses, and fungi. Using ioRinse in a Waterpik allows the patient to deliver the medicament into deep pocket areas.
The idea that reattachment of ligament can occur on clean root surfaces above existing calculus is new to me. I’m not saying it cannot happen. I checked with two periodontists, and both said it was unlikely. A “gross debridement” procedure that removes bulky calculus only can result in periodontal abscesses from the presence of deep calculus that remains if the patient procrastinates or fails to return for more thorough debridement. But I have never seen reattachment coronal to calculus.
I think we are well aware that periodontal probing is often inaccurate due to problems with angulation and root accretions that block the probe from being inserted correctly. A 3 mm reading on the area you shared seems strange, to say the least.
Thank you for sharing this most interesting case. If this lady were my patient, I would want her seen by a periodontist. If she didn’t like the first one, find another one. She may need flap surgery to figure this out. I would consider it a ticking time bomb, given the strange nature of the accretion and the surrounding bone. The safe route is to have a specialist decide if this is something that warrants further treatment. It is obvious that the patient is losing bone, and if she waits, she could lose the tooth.
All the best,
Dianne
References
1. Drisko CL, Killoy WJ. Scaling and root planing: removal of calculus and subgingival organisms. Curr Opin Dent. 1991;1(1):74-80.
2. Rabbani GM, Ash MM Jr, Caffesse RG. The effectiveness of subgingival scaling and root planing in calculus removal. J Periodontol. 1981;52(3):119-123. doi:10.1902/ jop.1981.52.3.119.
3. Moolya NN, Thakur S, Ravindra S, Setty SB, Kulkarni R, Hallikeri K. Viability of bacteria in dental calculus – A microbiological study. J Indian Soc Periodontol. 2010;14(4):222-226. doi:10.4103/0972-124X.76921.
DIANNE GLASSCOE WATTERSON, MBA, RDH, is an award-winning author, speaker, and consultant. She has published hundreds of articles, numerous textbook chapters, and three books. Her new DVD on instrument sharpening is now available on her website at wattersonspeaks.com under the products tab. Visit her website for information about upcoming speaking engagements. She may be contacted at (336) 472-3515 or by email at [email protected].
About the Author
Dianne Glasscoe Watterson, MBA, RDH
DIANNE GLASSCOE WATTERSON, MBA, RDH, is a consultant, speaker, and author. She helps good practices become better through practical analysis and teleconsulting. Visit her website at wattersonspeaks.com. For consulting or speaking inquiries, contact Watterson at [email protected] or call (336) 472-3515.
Updated June 30, 2020