Sealing to the limit: Sealants represent a safe and effective preventive measure across a variety of care settings
Sealants represent a safe and effective preventive measure across a variety of care settings
BY Noel Kelsch, RDHAP
A pit and fissure sealant is microbiology and prevention at their best. The occlusal surfaces of teeth are the most vulnerable to dental caries. In schoolchildren, up to 90% of decay occurs in this area (Kaste), with the highest risk teeth in children being first and second molars (NIDCR). A sealant is defined as a material placed to form a micromechanically-bonded protective layer in strategic places including pits and fissures, reducing caries up to 70% (Llorda). This protective layer blocks caries-producing bacteria from their source of nutrients; without functioning bacteria, there can be no decay.
Statistics are not in the public's favor when it comes to dental caries, whether you are an adult or a child. According to the National Institute of Dental and Cranial Research, 42% of children ages 2 to 11 have had dental caries in their primary teeth. Of those, 23% have untreated dental caries. As children get older, this chronic disease can progress. In addition, 59% of adolescents 12 to 19 have had dental caries in their permanent teeth - 20% with unmet needs.
---------------------------------------------------------
Other articles by Kelsch
- Sick staff, new law: Policies should spell out work restrictions for illnesses
- Jenn’s vision: A true lesson in best practices
- Give me a high five
---------------------------------------------------------
Adults are not faring much better - 92% of adults have had dental caries in their permanent teeth, and 26% have untreated decay. Sealants as a preventive measure can make a significant difference in treating this chronic contagious disease (NIDCR).
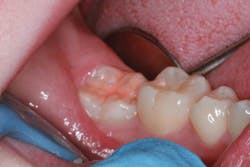
Photo courtesy of Dr. Daniel H. Ward, Columbus, OH
Decisions about sealant use should be based on the best available evidence about the effectiveness of the intervention on dental caries, including the risk factors and the epidemiology (Beauchamp). Clinicians should incorporate the science with the patient's individual needs and preferences. The oral health considerations of the patient include dry mouth, ability to perform oral care, caries risk, etc., giving the clinician a good understanding of which candidates should have sealants placed. Limiting the placement of sealants to only children and adolescents can limit preventive measures for adults and seniors.
The main contraindications for use of sealants are radiographic evidence of well coalesced and, thus, self-cleaning pits and fissures. Other considerations are a low caries risk and level of evident caries in proximal areas.
A Little History
My history of preventing dental disease came from my first dental experience. My childhood dentist did a procedure that was then considered preventive in nature. First introduced in the 1920s, an invasive procedure was performed on surfaces that might develop carious lesions (Hyatt). A prophylactic odontotomy was cut into the tooth and was then plugged with amalgam.
In 1955, Dr. Michael Buonocore came forward with a then-controversial, visionary, noninvasive procedure using bonded resin materials to "seal" out the decay process and fill in voids in fissures. There was much controversy about the possibility of sealing in bacteria with incipient lesions that would result in a rapid expansion of the lesion. In studies, it was found that the opposite was true; sealing of incipient caries in permanent teeth resulted in a 10% annual reduction in caries progression over unsealed teeth (Griffin).
By 1965, as etching and materials were refined, an 87% reduction in caries and a 71% retention was reported (Cueto). Interestingly, Buonocore chose the use of phosphoric acid because of improved adhesion of paint on metal after etching. In the 1970s, it was noted that it was difficult to identify where sealants were present because the resin materials were clear. Companies added white to sealants so that they could be identified easily.
In the 1980s, it was recognized that the first and second molars should be sealed as soon as possible after eruption (Burt). Not only can sealants be used to prevent caries; they can also be used therapeutically for early carious lesions or suspicious areas.
In 2000, products included the addition of color changes to allow the clinician to see if the process of curing the sealant has been completed.
Types of Sealants
The types of sealants are ever expanding. There are two basic types of sealants - glass ionomer cements and resin-based. The retention rates for both products are the same (Seth).
• Glass ionomer (GI) - Glass ionomer cements, which fall into two basic groups of conventional and resin modified, do not require acid etching of the tooth surface, and they generally are easier to place than resin-based sealants. This is especially important in the public health setting and mobile practices. The added benefit of lack of moisture sensitivity really is a benefit when working with these materials (Browning). This material was developed to release fluoride and bond directly to the enamel. They do not shrink over time.
• Resin-based: Resin-based materials are available as polymerized by autopolymerization (no light curing required), photopolymerization using visible light (curing light), or a combination of the two processes.
Sources for sealants and related manufacturer information | ||
Product | Company | Website |
Aegis | Keystone-Bosworth Co. | keystoneindustries.com |
Alpha-Seal | Dental Tech | dentaltech.com |
Aura Lay | Denali Corp. | denalicorporation.com |
BeautiSealant | Shofu Dental Corp. | shofu.com |
Clinpro | 3M ESPE | 3mespe.com |
CosmeSeal | Cosmedent, Inc. | cosmedent.com |
Delton | Dentsply International | dentsply.com |
Embrace WetBond | Pulpdent | pulpdent.com |
GC Fuji Triage | GC America, Inc. | gcamerica.com |
Guardian Seal | Kerr Corp. | kerrdental.com |
Helioseal F | Ivoclar Vivadent | ivoclarvivadent.us |
Nu Radiance | Nu Radiance, Inc. | nuradiance.com |
PacSeal | Pac-Dent International, Inc. | pac-dent.com |
Toothfairy | Septodont | septodontusa.com |
Ultraseal XT | Ultradent Products Inc. | ultradent.com |
Virtuoso | DenMat Holdings, LLC. | denmat.com |
Suction: If you are using a sealant material that is moisture sensitive, make sure you have great suction. Suction devices developed to be retained or flexible can be a great help in this area.
Cotton rolls and dry products: I use cotton roll holders under the tongue to capture everything that Wharton's duct produces and a triangle that adheres to the side of the cheek for the Stensen's duct. To remove the cotton materials, simply moisten, and they will easily release.
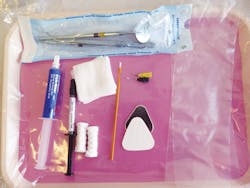
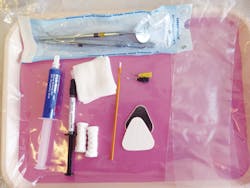
Make a list: Make a list of the products and instruments you will need to complete this task. This is one of the duties where it is very difficult for you to get up once you are seated. Keep a separate tray with all the needed supplies from your list.
Syringes: Cover syringes with barrier protection that you change between every patient. Place the disposable syringe tip before seating the patient. Check it to make sure the product can flow on a piece of gauze. Never reuse a disposable syringe tip! Always replace the permanent cap after use.
Curing light: Check your curing light regularly for bulb degeneration with an inexpensive radiometer. Look for any scratches, fractures, or chips on the end of the light. These flaws impact performance. Make sure there is no sealant material on the curing light, and do not touch the sealant material with the curing light. I prefer a noncorded light for ease of use. Make sure it is charged ahead of time, especially if you are going out into the field. Buying a second light can make a big difference.
Air-water syringe tip: One of the overlooked areas of dryness is the air-water syringe tip. Make sure you have a great tip that has a clear division between air and water and is not cross contaminating the air with water. You can check this by spraying the air on a piece of paper. There are great disposal tips that eliminate this problem.
Scheduling time: If you have a choice, see children after recess and before lunch. The saliva level goes down after a child sweats! Their energy and wriggle level also goes down.
BPA: There was a controversy about bisphenol A-glycidyl methylacrylate (BPA) that most sealants are made from because it replicates estrogen. It was thought that this could lead to hormonal reactions in the patient. This is a very small amount, and there have been no findings of systemic BPA after placement (Fung, Söderholm). BPA forms an oily residue after placement. Simply wipe it with a 2x2 after curing. If a patient or caregiver has an issue with BPA, simply use a glass ionomer.
Lips: Put a nonpetroleum-based product on the patient's lips (petroleum-based products can break down exam gloves). This area is the number one complaint of patients when doing several sealants.
Do not limit: Sealants are one of the least invasive ways to prevent dental decay. Make all your patients aware of this simple preventive measure. Seniors will pay more for the deductible on a filling than the cost of a simple sealant. Sealants done bedside for patients unable to come into the dental setting can prevent the progression of disease.
Protective eyewear: Always make sure all your patients are wearing protective eyewear when working in the dental setting. This is especially important for the phosphoric acid contained in the etchant. If etchant does get in the eye, follow the package directions, which generally state: Flush immediately with copious amounts of water; consult a physician after flushing.
They can be unfilled or filled. Filled sealants contain particles of quartz and/or glass that increase strength and resistance to wear. Sealants with fillers may require adjustment because of their strength and are more viscous. Unfilled sealants are usually clear and are self-occluding - therefore ideal for public health settings. There is no difference in retention in filled or unfilled products (Wilkins).
It is important to note that you need to read and follow the directions that are provided with sealants. They differ from manufacturer to manufacturer.
One of the most challenging areas of doing sealants, especially in the school-based setting, is maintaining clean, dry surfaces before placement. Tests with contaminated enamel yielded poor/lower bonding strength (Thomson). Drying agents have been introduced with very little difference in outcomes for retention (Rix).
The use of etchants has been examined from many aspects:
• Etchant vs. air abrasion: It does not appear that air abrasion had any advantage over acid etching. Studies showed retention with air abrasion is inferior to acid etching (Kanellis).
• Strength of etchant: The research on the strength of etchant material was interesting. When Buonocore started his studies of sealants he was using 85% phosphoric acid for 60 seconds. After studying the retention levels with different levels of acid, it was found that the acid could be as low as 35% and still be effective.
• Time of exposure: Time of exposure to etchant has evolved over the years. During the 1970s, due to the "prismless" nature of primary enamel, it was thought that primary molars would require twice the etching time of permanent enamel, and this became the standard clinical procedure. It was then discovered there is no evidence of prismless enamel on occlusal surfaces, and studies showed that there was no difference in retention using 60 seconds of etching vs. 120 seconds of etching (Simonsen 1978). A later report noted that, "Decreasing the etch time for primary molars has been found to decrease the chance of contamination, during etching. Additionally, the shorter etch time was far more acceptable to 3- and 4- year-old children" (Simonsen).
For permanent enamel, shorter etching times have been found just as effective as longer etching times. The findings demonstrate that the retention rates of fissure sealants using 20 seconds etching time are comparable to those reported with the more conventional 60 seconds (Eidelman).
Exposure time to the curing light was also evaluated, comparing 15, 30, 45, and 60 seconds. Interestingly, these different etching times in first permanent molars or second primary molars did impact retention (Duggal).
Fluoride Treatment and Postop
Several studies dispel the myth about fluoride treatments initiated prior to sealants. This makes treating the patient in one visit so much easier. Previously, there was the misconception that sealants could not be placed after a fluoride treatment.
Studies have shown that topical fluoride treatment has no clinical effect on retention. Sodium fluoride, stannous fluoride, and acidulated phosphate fluoride use prior to placement of unfilled sealants has no effect on in vitro bond strength between the enamel and sealants (Brown, Koh). It is clear that fluoride does not block the ability of phosphoric acid to etch enamel.
After placements of sealants, using fluoride varnish on the surfaces of teeth that do not have sealants can be a great advantage and does not negatively impact the sealant. If the sealant has failed or is shrinking, they are an advantage.
When sealants are placed, some patients and caregivers get the impression that home care and contributing factors such as diet can be set aside. It is vital for the clinician to remind the patient and caregivers of the importance of continuation of home care and to counsel them on all contributing factors.
Once sealants are placed, it is vital that they be evaluated for retention through both tactile and visual exams every six months. If there are voids in the sealants, these can be repaired by etching the area and reapplying the sealant or following the product's directions.
Pit and fissure sealants are a safe, effective, and preventive measure. They can make a difference in the progression of dental caries. RDH
NOEL BRANDON KELSCH, RDHAP, is a syndicated columnist, writer, speaker, and cartoonist. She serves on the editorial review committee for the Organization for Safety, Asepsis and Prevention newsletter and has received many national awards. Kelsch owns her dental hygiene practice that focuses on access to care for all. She helps facilitate the Simi Valley Free Dental Clinic and has devoted much of her 35 years in dentistry to educating people about the devastating effects of methamphetamines and drug use. She is a past president of the California Dental Hygienists' Association.
References
1. Beauchamp J, Caufield PW, et al. Evidence-based clinical recommendations for the use of pit-and-fissure sealants: A report of the American Dental Association Council on Scientific Affairs JADA 2008;139(3):257-267.
2. Brown JR, Barkmeier WW. A comparison of six enamel treatment procedures for sealant bonding. Pediatr dent. 1996;18:29-31.
3. Browning WD. The benefits of glass ionomer self-adhesive materials in restorative dentistry. Compen Contin Educ Dent. 2006;27:308-314.
4. Burt BA. Fissure sealants: Clinical and economic factors. J Dent Ed. 1984;48:96-102.
5. Cueto EI, Buonocore MG. Sealing of pits and fissures with adhesive resin: Its use in caries prevention. JADA. 1967:75:121-128.
6. Duggal MS, Tahmassebi JF, Toumba KJ, Mavromati C. The effect of different etching times on the retention of fissure sealants in second primary and permanent enamel: an evaluation. ASDC J Dental Child. 1989;56:186-190.
7. Eidelman E, Shapira J, Houpt M. The retention of fissure sealants using twenty-second etching time: three-year follow-up.ASDC J Dent Child. 1988 Mar-Apr;55(2):119-20.
8. Fung E, Ewoldson N, St. Germain H, Marx D, Miaw CL, Siew C, Chou HN, Gruninger S, Meyer D. Pharmacokinetics of bisphenol A released from a dental sealant. J Am Dent Assoc. 2000 131(1): 51-58.
9. Griffin SO, Oong E, Kohn W, Vidakovic B, Gooch BF. CDC Dental Sealant Systematic Review Work Group, et al. The effectiveness of sealants in managing carious lesions. J Dent Res 2008;87(2): 169-174.
10. Hyatt TP. Prophylactic odontotomy: the cutting into the tooth for prevention of disease. Dent Cosmos. 1923:65:234-241.
11. Kaste LM, Selwitz RH, Oldakowski RJ, Brunelle JA, Winn DM, Brown LJ. Coronal caries in the primary and permanent dentition of children and adolescents 1-17 years of age: United States, 1988-1991. J Dent Res 1996;75 (Spec No):631-41.
12. Kanellis MJ, Warren JJ, Levy SM. A comparison of sealant placement techniques and 12-month retention rates. J Public Health Dent. 2000;60:53-56.
13. Koh SH, Chan JT, You C. Effects of topical fluoride treatment on tensile bond strength of pit and fissure sealants. Gen Dent. 1998;46;278-280.
14. Llodra JC, Bravo M, Delgado-Rodriguez M, Baca P, Galvey R. Factors influencing the effectiveness of sealants-a meta-analysis. Community Dent Oral Epidemiol 1993;21(5):261-8.
15. nidcr.nih.gov/datastatistics/finddatabytopic/dentalcaries/
16. Rix Am, Sams DR, Dickinson GL, Adair SM, Russell CM, Hoyle SL. Pit and fissure sealants application using a drying agent. Am J Dent. 1994;7:131-133.
17. Seth S. Glass ionomer cement and resin-based fissure sealants are equally effective in caries prevention. J Am Dent Assoc 2011 142(5): 551-552.
18. Simonsen RJ. Fissure Sealants: deciduous molar retention of colored sealant with variable etch time. Quintessence Int. 1978;9:71-77.
19. Söderholm KJ, Mariotti A. BIS-GMA-based resins in dentistry: are they safe? J Am Dent Assoc. 1999 130(2): 201- 209.
20. Thompson JL, Main C, Gillespie FC, Stephen KW. The effect of salivary contamination on fissure sealant-enamel bond strength. J Oral Rehabil. 1981;8:11-19. Wilkins EM. Clinical Practice of the Dental Hygienist (10th ed., pp. 60-64). Baltimore: Lippincott Williams & Wilkins, 2009.