Clearing up the confusion
Orofacial myology attracts the attention of hygienists, but do they know why?
By Angie Lehman, RDH, COM, and Joy Lantz, RDH, COM
Over the past several years, the field of orofacial myology has experienced a renaissance of sorts. Believe it or not, the concept of orofacial muscles affecting orofacial growth and development has been written about for centuries.1 Orofacial myology has officially been a growing subspecialty for over 45 years, yet many people have just recently started hearing the buzz surrounding this amazing field. As with any concept that experiences a rebirth or renewal, it’s often difficult to filter through what is factual and evidence based, and what is hype or pseudoscience.
Based on the number of inquiries we receive from dental hygienists each week, and the frequency that this topic appears in many dental-related social media threads, we wanted to present a concise summary of the basics of orofacial myology, and how we as hygienists have entered and flourished in this field.
Orofacial myology is defined as “the study and treatment of oral and facial muscles as they relate to speech, dentition, chewing/bolus collection, swallowing, and overall mental and physical health.”2 We treat orofacial myofunctional disorders, or OMDs. Although we typically refer to ourselves as orofacial myologists, we are also known as orofacial myofunctional therapists, myofunctional therapists or, in the early days of our specialty, tongue thrust therapists. It’s unfortunate to see how the term tongue thrust therapist has lingered for the past few decades because, even though we do treat tongue thrusting, the field of orofacial myology is so much more. Research has advanced our field in leaps and bounds over the years, and we now understand that tongue thrusting is not the source of an OMD. It just happens to be one of the easiest symptoms to recognize.
Identifying symptoms
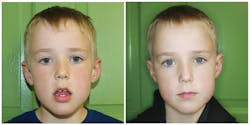
OMDs can include a myriad of different symptoms. In addition to tongue thrusting when speaking or swallowing, one of the most recognizable red flags is an open-mouth posture, often associated with chronic mouth breathing. The inability to breathe through the nose because of enlarged tonsils or adenoids or nasal allergies statistically leads to the highest number of OMDs.3 Noxious oral habits such as prolonged pacifier use or thumb sucking, or issues surrounding ankylosed oral frena also contribute to OMDs.
If we look at the common link between mouth breathing, sucking habits, and tongue tie, we will notice that in all three instances, the tongue is resting low in the mouth, the lips may be parted, and the jaw is opened beyond the normal freeway space. In other words, there is a deviation from the normal resting position of the orofacial muscles, which leads to altered function. Our goal as orofacial myologists is to address these issues and restore proper resting position and function, often through a team approach.
Certification in orofacial myology
If there is one facet of orofacial myology that seems to generate the most discussion and confusion, it is the topic of certification. It is a common misconception that taking any course leads to immediate certification. In fact, the certification process is much more involved, and can only be accomplished through one organization, the International Association of Orofacial Myology (IAOM).
The IAOM is a nonprofit organization that began 45 years ago, and their certified members can legally use the trademarked credential “COM” behind their name, only after they have completed and passed a written examination and an on-site clinical evaluation. No other letters can legally be used behind a therapist’s name at this point in time. Although anyone with an interest in orofacial myology can join the organization as an honorary member, the introductory courses and certification are limited to the three fields whose existing scope of practice already contains wording that allows them to recognize and treat OMDs: dentists, dental hygienists, and speech and language pathologists.
When it comes to training, the first step is a four-day, 28-hour introductory course. These courses are offered by a variety of instructors, but only IAOM-approved introductory courses can be used as a prerequisite to pursuing certification. A list of dates and locations can be found on IAOM’s website (iaom.com). Once the course is completed, you are eligible to become certified.
The process for pursuing certification is a very important component of orofacial myology training. Many certified therapists describe their time working on the test as one of the most beneficial learning tools on their journey in this field. It helps you grow as a therapist and as a person. It ensures that there is consistency and uniformity in the knowledge needed to treat patients. Just as licensure is an important part of becoming a hygienist, certification is an imperative component to becoming an orofacial myologist. As hygienists are required to have continuing education hours fulfilled each license renewal period, a COM also has mandatory CE hours that are required to maintain his or her certification.
Orofacial myofunctional therapy (OMT) could really be considered oral rest posture therapy. The focus of therapy, no matter what OMD we are treating, is always reestablishing proper oral rest posture. Take a moment to evaluate where your orofacial muscles are resting. Where is your tongue? Are your lips sealed? Are you breathing through your mouth or through your nose? A healthy oral rest posture includes the tongue resting on the palate, gently sealed lips, and nasal breathing. There should be approximately 2–3 mm of freeway space between the molars; therefore, the jaw is not hinged open, nor are the teeth touching.
When we have good rest posture, there is equilibrium in the orofacial complex, allowing for both proper form and proper function. Good oral equilibrium contributes to proper growth of the jaws, allowing for enough space to accommodate all of the permanent teeth. When the jaws are the proper size, we have wide sinuses and sufficient space for healthy breathing.
OMT is often the most beneficial when children are still growing. Just as early orthodontic treatment guides growth in the jaws, correcting oral rest posture can also have a significant influence on orofacial development during the rapid growth period that occurs in childhood. Additionally, OMT can also be very beneficial to adult patients. Even though we cannot significantly change the bony structures via therapy alone, correcting rest posture and maximizing function can have a considerable impact.
In recent years, we have seen research studies in relation to temporomandibular joint disorder (TMJD) and obstructive sleep apnea (OSA)/upper airway resistance syndrome (UARS). The science is promising and exciting; however, it is still in the early stages of research. Because OSA and TMJD can be caused by a myriad of different factors, we need to be cautious portraying OMT as a “treatment” for these issues. Therefore, it is important to only treat these patients if there are existing oral rest posture issues.
As hygienists who have entered this specialty and completed certification, we can tell you that nothing is more rewarding than this journey we are on. Is it hard? Absolutely. We have spent hours, months, even years educating the medical professionals in our areas. But every minute spent marketing and educating others is paying off. We love what we do. We love the impact that this therapy can have on our patients. We love the networking and collaboration that this field provides. We feel so privileged to be a part of the rebirth and renewal of the field of orofacial myology.
Angie Lehman, RDH, COM, has been certified by the International Association of Orofacial Myology (IAOM) and practicing orofacial myology exclusively since 2012. She currently serves on the board of directors for the IAOM. Angie is owner of Oral Myofunctional Therapy of York, a private practice in York, Pennsylvania, that provides myofunctional therapy to children and adults. She also provides continuing education for dental and medical professionals. Her passion is to see all dental and medical professionals work collaboratively to better understand oral function and craniofacial development and incorporate therapy into their specific areas of care.
Joy Lantz, RDH, COM, has over 20 years of experience in the dental field. She graduated from Prairie State College. She is a certified orofacial myologist at her privately-owned business, Spot On Myo, in Tinley Park and Palos Heights, Illinois. She loves being a tongue trainer and teaching all people how to tie cherry stems with their tongues, a lifelong talent.
References
1. Hanson ML, Mason RM. Orofacial Myology: International Perspectives. Springfield, Illinois: Charles C. Thomas: 2003.
2. Holtzman SR. Orofacial Myology: From Basics to Habituation. Orlando, Florida: Neo-Health Services; 2014.
3. Valera FC, Travitzki LV, Mattar SE, Matsumoto MA, Elias AM, Anselmo-Lima WT. Muscular, functional and orthodontic changes in preschool children with enlarged adenoids and tonsils. Int J Pediatr Otorhinolaryngol. 2003 Jul;67(7):761-70.