Anesthesia for older adults: Local anesthesia facilitates aggressive perio treatment
Older adults are one of the fastest growing populations in the world. In fact, we soon will have more older people than children and more people at extreme old age than ever before as life expectancy increases.1 Since 1900, the percentage of Americans 65 and older has more than tripled (from 4.1% in 1900 to 14.1% in 2013). The older population itself is increasingly older. In 2013, the 65-74 age group (25.2 million) was more than 10 times larger than in 1900; the 75-84 group (13.4 million) increased by 70 percent and the 85+ group (6 million) was 49 times larger. It is predicted that the older population will continue to rise significantly in the future.2
National data have also shown that the rate of tooth retention has increased for older adults. In the 65-74 year-old age group, the prevalence of edentulism declined from 50% in 1960 to 24% in 2002. It is believed that advances in prevention and treatment have had significant impact on reduced tooth loss among older adults.3
Although age alone is not a determinant of periodontal diseases, there is an association between increased age and increased incidence of periodontal diseases.3,4 The American Academy of Periodontology reports that older people have the highest rates of periodontal disease, and data from the Centers for Disease Control and Prevention indicates that over 70% of Americans 65 and older have periodontitis.5,6
Dental hygienists play a significant role in prevention and treatment of dental diseases. Often, we provide local anesthesia for patients with periodontal diseases during nonsurgical periodontal therapy (NSPT) since it facilitates comfortable and aggressive treatment to prevent and control diseases. Aggressive treatment may be especially important to prevent and control periodontal disease for older adults.
Patient Profile
Older adults frequently present with a history of multiple and chronic diseases/conditions, including anxiety, arthritis, cardiovascular disease, cerebrovascular accident, depression, liver disease, and respiratory disease. They often:
- take multiple medications that can increase the rate of adverse reactions
- metabolize drugs at a slower rate, which can result in a higher risk of system toxicity
- have a higher pain threshold, but have a greater need for safe and high quality pain control (profound anesthesia) for existing conditions
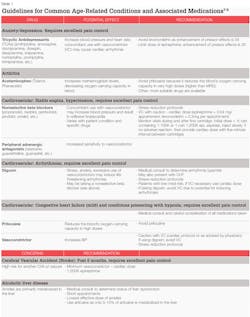
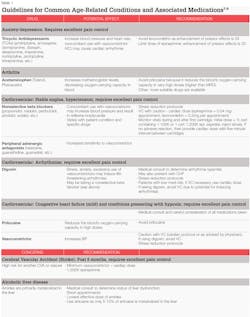
As discussed in the author's January 2016 article in RDH magazine ("Understanding available agents: Overview of injectable agents useful for nonsurgical periodontal therapy"), there are few absolute contraindications (true bisulfite allergy or documented drug allergy, for example) for specific local anesthetic agents for patients already eligible to receive elective procedures such as nonsurgical periodontal therapy. Even though local anesthetics are remarkably safe at therapeutic doses, we must consider existing conditions that may be exacerbated by the anesthetic agent and medications that may precipitate adverse interactions with local anesthetic agents. Discussed below are guidelines for some common age-related conditions and associated medications that may require modifications in use of local anesthetic agents (Table 1).
Since older adults frequently present with systemic disease and often take multiple medications, dental hygienists must carefully weigh the risks vs. benefits when considering pain control options. For the older and medically complex patients, it is particularly important to administer the lowest effective dose of the local anesthetic while utilizing proper technique to achieve safe, comfortable, and profound local anesthesia.
Care should be taken during tissue retraction and needle penetration as older patients often have loss of elasticity of lips and oral mucosa and may also have sensitive oral tissues due to xerostomia. Attention to agent selection, dose, injection technique, as well as stress reduction protocols (see Table 2) and monitoring of vitals may be necessary not only before and afterwards but also during the procedures. RDH
Table 2
Stress Reduction Protocol3,7
- Short, morning appointments early in the week are usually best
- Minimize patient waiting time
- Open, honest communication regarding questions, concerns, fears
- Calm, quiet, professional environment
- Premedication with benzodiazepines , if needed
- Ensure excellent pain control through judicious selection of local anesthetic agents and maintenance of comfort
- Use nitrous-oxide and oxygen sedation, if needed
- Terminate procedure if patient appears overstressed
- Contact patient evening of appointment
References
1. www.un.org/esa/population/publications/worldageing19502050
2. A Profile of Older Americans: 2014 (Administration on Aging)-Dept of HHS-USA
3. Darby ML, Walsh M. (2015). Dental Hygiene Theory and Practice 4th ed. Elsevier
4. Perry DA, Beemsterboer PL, Essex G. (2014) Periodontology for the Dental Hygienist 4th ed. Elsevier
5. https://www.perio.org/consumer/risk-factors
6. http://www.cdc.gov/OralHealth/periodontal_disease/index.htm
7. Little JW, Falace DA, Miller CS, Rhodus NL. (2013). Little and Falace's Dental Management of the Medically Compromised Patient, 8th ed. Elsevier
8. Logothetis DD. (2012). Local Anesthesia for the Dental Hygienist. Elsevier
9. Malamed S. (2013). Handbook of Local Anesthesia 6th ed. Elsevier
LAURA J. WEBB, RDH, MS, CDA, is an experienced clinician, educator, and speaker who founded LJW Education Services (ljweduserv.com). She provides educational methodology courses and accreditation consulting services for allied dental education programs and CE courses for clinicians. Laura frequently speaks on the topics of local anesthesia and nonsurgical periodontal instrumentation. She was the recipient of the 2012 ADHA Alfred C. Fones Award. She can be contacted at [email protected].
For the most current dental headlines, click here.
About the Author

Laura J. Webb, MS, RDH, FAADH
Laura J. Webb, MS, RDH, FAADH, is an experienced clinician, educator, and speaker who founded LJW Education Services (ljweduserv.com). She has provided educational methodology courses and accreditation consulting services for allied dental education programs and CE courses for clinicians. Laura has frequently spoken on the topics of local anesthesia and nonsurgical periodontal instrumentation. She was the recipient of the 2012 ADHA Alfred C. Fones Award. Laura can be reached at [email protected].
Updated May 2023