I screen, you screen, we all screen: No one has ever done that before!
A recap of this course from RDH Under One Roof 2023
Dental hygienists play a critical role in the early detection of oral and oropharyngeal cancer as well as identifying any head or neck abnormalities that may require referral to the appropriate specialist. Performing comprehensive visual, tactile extra- and intraoral evaluations is nonnegotiable.
When performing a comprehensive screening, patients will often say, “No one has ever done that before. Is this something new?” Some patients have either never received a screening before or were only given a cursory examination, perhaps only a quick look at the tongue. Others may have received a comprehensive screening but were never told it was an oral cancer screening. As dental professionals, we can’t assume our patients know what we are doing.
In the following paragraphs, we will review my course from RDH Under One Roof 2023, which was structured around the four science pillars of screening in the Cotten Method—with an emphasis on pillars II, III, and IV. I am thrilled to review the course in this article!
Pillar I: Etiologies
In the Cotten Method, etiologies encompass what we know about oral cancer. It’s essential to have a solid knowledge of the etiologies of oral and oropharyngeal cancer so we can share that information confidently with patients. Historically, we know that tobacco use in all forms and chronic high alcohol use increase the risk for oral cancer, and significantly increase the risk when used together. The human papillomavirus (HPV) causes over 70% of oropharyngeal cancers, and it is the persistent HPV infections that can go on to cause cancer in the oropharynx.1
Another known etiology of oral cancer is betel quid, made from the betel nut (aka areca nut), which is the seed of the areca palm fruit. Betel quid is the fourth most commonly used addictive substance worldwide behind tobacco, alcohol, and caffeine.2 The betel nut is chopped or sliced and mixed with slacked lime and other additives for flavor. The mixture is then placed on a betel leaf, rolled, and put in the mouth. When tobacco is added to the mixture, it is called gutka.
Pillar II: Additional risk factors
What we know now, there are additional risk factors for oral cancer just as there are risk factors for other diseases. It is important to remember that these are not causes. When assessing a patient, these factors deserve serious consideration in the overall picture to determine the best next steps for referral and follow-up of persistent signs and symptoms. Additional risk factors for oral cancer include poor oral health,3,4 obesity,5 previous occurrence of oral or oropharyngeal cancer,4 a compromised immune system,4 taking immunosuppressive medications,4 poor nutrition (a diet low in fruits and vegetables),4 and radiation exposure,6 to name a few.
Pillar III: Signs and symptoms
It is essential to know and recognize the signs and symptoms associated with oral and oropharyngeal cancer, as these may present before a lesion becomes noticeable in the mouth. Ask about signs and symptoms and how long they have persisted. If any sign or symptom persists for two weeks, the patient needs a referral to the appropriate specialist for further investigation.
Signs and symptoms include difficulty swallowing; the sensation of something caught in the throat that won’t go down; a mass or lump anywhere in the mouth, neck, or head; difficulty chewing; and unexplained weight loss. Other signs include persistent swollen lymph node(s), sore throat, cough, hoarseness, change in voice, lesions or sores, ear or jaw pain, any pain in the head or neck, numbness, and fatigue. This includes persistent lesions, sores, and red or white patches that do not resolve in two weeks.
Pillar IV: Comprehensive visual, tactile extra- and intraoral evaluation/oral cancer screening
Calibration in screening is essential to ensure continuity of care and early detection. Let’s look at the components of a comprehensive oral cancer screening, starting with telling your patient you are doing an oral cancer screening. Observe the patient from the moment you greet them in the reception area, watching their gait and listening to their voice.
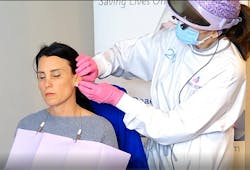
Extraoral evaluation: In the operatory, look at the head and neck for any asymmetries. Closely examine the skin, nose, ears, hairline, and part in the hair for any abnormal-looking tissue that may require a referral to a dermatologist (figure 1).
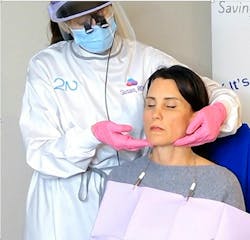
Assess the TMJ for crepitus, popping, or pain; palpate the submandibular, sublingual, and parotid glands; and palpate the lymph nodes of the head and neck (figure 2). Palpate each lobe of the thyroid gland, observing for symmetry and any nodules. Assess the patient’s swallow.
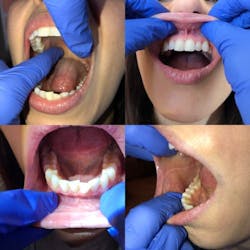
Intraoral evaluation: Observe the lips, looking at the commissures and vermilion border. Palpate and visualize the buccal and labial mucosa, the hard and soft palate, and the entire floor of the mouth, pulling the cheeks and lips out for optimal visualization (figure 3).
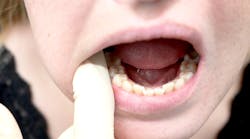
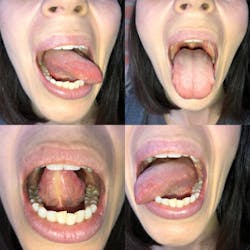
Thoroughly examine the tongue. Visualize and palpate the lateral borders, the posterior base of the tongue, and dorsal and ventral surfaces. Have your patient stick their tongue out, and move it side to side and to the roof of the mouth (figure 4). Ask your patient to open wide and say aah so you can visualize the entire oropharynx.
Start somewhere!
If you aren't performing a comprehensive screening—or screening at all—I encourage you to start somewhere. Get confident in performing this lifesaving procedure that increases early detection and reduces your risk of liability. If you feel the time you are given for your hygiene appointments doesn’t allow for thorough assessments and optimal treatment, have a professional and meaningful conversation with the dentist and office manager to advocate for yourself and your patients. Dental professionals are oral health specialists, and nothing shouts optimal oral health more loudly than screening for and detecting oral cancer to save a life!
Editor's note: This article appeared in the June 2024 print edition of RDH magazine. Dental hygienists in North America are eligible for a complimentary print subscription. Sign up here.
References
- Human papillomavirus (HPV). The University of Texas MD Anderson Cancer Center. https://www.mdanderson.org/prevention-screening/manage-your-risk/hpv.html
- Zdrojewicz Z, Kosowski W, Królikowska N, Stebnicki M, Stebnicki MR. Betel - czwarta najpopularniejsza używka na świecie. [Betel – the fourth most popular substance in the world.] Pol Merkur Lekarski. 2015;39(231):181-185. Polish.
- Irani S, Barati I, Badiei M. Periodontitis and oral cancer – current concepts of the etiopathogenesis. Oncol Rev. 2020;14(1):465. doi:10.4081/oncol.2020.465
- Oral cancer. The University of Texas MD Anderson Cancer Center. https://www.mdanderson.org/cancer-types/oral-cancer.html
- Heath BR, Gong W, Taner HF, et al. Saturated fatty acids dampen the immunogenicity of cancer by suppressing STING. Cell Rep. 2023;42(4):112303. doi:10.1016/j.celrep.2023.112303
- Risk factors. What causes cancers of the head and neck? Head and Neck Cancer Alliance. https://www.headandneck.org/risk-factors/
About the Author

Susan Cotten, BSDH, RDH, OMT
Susan Cotten, BSDH, RDH, OMT, is dentistry’s oral cancer coach, 2018 Sunstar/RDH Award of Distinction recipient, and developed The Cotten Method™ of Screening for oral, oropharyngeal cancer, and other head and neck concerns. With more than 30 years as an RDH, Susan provides in-office training, speaking, and hands-on workshops to deepen confidence in a comprehensive screening, reduce liability, and increase early detection. Determined to have a world Oral Cancer Free™, her course is available online through the National Network of Healthcare Hygienists. Reach her at [email protected].