Continuing care overload
Dear Dianne,
I work in a large practice with three doctors and six full-time hygienists. According to our practice management software, we have around 8,500 active patients. We are about 80% fee-for-service and 20% PPO. We are always busy, and the phone rings almost nonstop. There are four business assistants and an office administrator.
The problem we have is recall. I feel we do a poor job of keeping recall up to date because there are so many patients. Most patients schedule six months ahead, but some of our patients are on a one-year recall. Rarely do they schedule that far ahead. Then there are the perio maintenance patients who fall through the cracks because we do not have any openings. We get complaints from patients about not being able to get a timely appointment. We also have days when we have two to four open appointments, and the business desk apparently doesn’t know who to call to try to fill the time. It’s just a mess!
Do you have any tips for us on improving our recall system?
Thanks in advance,
Midsouth Hygienist
Dear Midsouth,
First off, I’d like to suggest that we all get away from using the term “recall.” It reminds me of a car company “recalling” its defective vehicles for some problem. Furthermore, the term “recall” trivializes the preventive visit, much like the phrase “cleaning and checkup.” My suggestion is to use the phrase “preventive care,” “continuing care,” or “professional hygiene care” as a better alternative.
I see two primary problems. One is a capacity versus demand issue. It takes about 800 to 1,000 patients to keep one full-time hygienist busy. With an active patient base of 8,500, you could keep eight hygienists busy. You have more demand for care than available appointments (capacity), and this creates a backlog. The second problem is that you may be understaffed and/or disorganized at the business desk. If a practice has a large number of hygienists, there should be one business assistant with the title of hygiene department coordinator. This assistant’s job would be to maintain the hygiene schedules of all hygienists and coordinate all continuing care. It’s a big job with a lot of responsibility. Because hygiene often drives the rest of the practice, it has to be someone’s primary responsibility to maintain the hygiene schedules and continuing care system.
When our schedules are full, most offices are not too concerned with contacting patients and getting them scheduled. However, the problem of more demand than capacity is detrimental in the long run. When patients become frustrated because they can’t get timely appointments, they go elsewhere. Sometime later, the office begins to see increasing open time in the schedule. That’s when they realize the pendulum has swung the other way, and they have lost a significant number of patients. It’s harder and more costly to get new patients than to retain existing patients, so it’s much better to address the problem by looking at ways to increase capacity. Some options include adding a satellite office, adding some nontraditional hours, or increasing the size of the existing office by adding more operatory space.
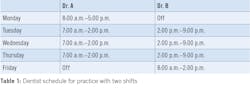
One office I worked with had three total operatories, and there was no space to build it any larger. So, to address the demand issue, it added a second shift dentist and staff. Table 1 shows how the schedule worked.
The beauty of this arrangement was that there was more efficient use of space, and many patients loved the nontraditional hours. The practice doubled its capacity and built a large, financially healthy practice without incurring heavy debt.
I would like to add that your problem is unique. Many offices today see the opposite scenario, where they have lots of open time in their schedules and low demand. Sometimes, there simply are not enough patients to keep everyone busy. Personally, I would rather see demand exceed capacity for obvious reasons.
From your post, I suspect there is no good continuing care system in place. If there was, the hygiene department would be experiencing minimal downtime. Having two to four open appointments per day per hygienist is definitely not minimal.
Fortunately, automation has enabled us to be far more efficient in communicating and keeping track of our patients than in the past. A large office such as yours should see automation as a necessity, not an option. So, my first suggestion would be to implement a good automated patient communication system. An automated system is almost like adding an additional staff member. There are several on the market, but my personal favorite is one called Lighthouse 360. It’s designed to prevent holes in your schedule and keep patients coming back. The cost at the time of this writing is $329/month with no annual contract.
Automated patient communication systems can reduce no-shows; tighten recall; automatically confirm appointments; send continuing care reminders; reach all of your patient base via email, text, phone, and mail; and sync with your practice management system.
Here are some additional suggestions for improving the continuing care system:
- You should reappoint most patients for their continuing care visits, but be discriminating. Do not offer this option to patients with a history of disappointments (i.e., missed appointments). Such patients should receive a card in the mail asking them to call for an appointment.
- Block time for periodontal scaling and periodontal maintenance. These are priority patients, and treating their infections in a timely manner is important. To know how much time to block, go back three months and total the number of periodontal appointments. Divide this number into the total days worked. This will be the average amount of periodontal time needed on a daily basis.
- In the absence of an automated system, print out a monthly report of unscheduled continuing care patients. Depending on the size of the list, the hygiene department coordinator should have a goal to contact a set number of patients per day on the list. This staff member should give a report at the monthly staff meeting detailing how many calls were made and how many patients were scheduled. It’s all about accountability.
- Select one time per month for making calls during nontraditional hours, such as a Saturday morning between 9:00 a.m. and 12:00 p.m. or an evening between 6:00 p.m. and 8:00 p.m.
- Always ask patients how they would like to be contacted, i.e., telephone, traditional mail, email, or text. Some may appreciate a combination approach.
Putting it all together
Keeping hygiene schedules full is an important function of a thriving and healthy dental practice. It requires diligence and daily (sometimes hourly) attention from a staff member who knows and understands how to be effective and efficient. A good patient communication system can simplify and improve efficiency exponentially if staff members receive the proper training and understand how to use the program to its full capacity.
All the best,
Dianne
DIANNE GLASSCOE WATTERSON, MBA, RDH, is a consultant, speaker, and author. She helps good practices become better through practical analysis and teleconsulting. Visit her website at wattersonspeaks.com. For consulting or speaking inquiries, contact Watterson at [email protected] or call (336) 472-3515.
About the Author
Dianne Glasscoe Watterson, MBA, RDH
DIANNE GLASSCOE WATTERSON, MBA, RDH, is a consultant, speaker, and author. She helps good practices become better through practical analysis and teleconsulting. Visit her website at wattersonspeaks.com. For consulting or speaking inquiries, contact Watterson at [email protected] or call (336) 472-3515.
Updated June 30, 2020