Intervention techniques for discontinuation of nonnutritive sucking habits
Ashley M. Adkisson, BS, RDH
Emily R. Holt, MHA, RDH, CDA, EFDA
Nonnutritive sucking habits are utilized by infants and children to provide a sense of calmness and comfort.1 Nonnutritive sucking includes use of a pacifier, thumb sucking, or finger sucking.1 Digit sucking occurs as early as the 29th week of gestation and is seen commonly in infants, peaking at 18–21 months of age.2 Digit sucking is the most prevalent of oral habits.2,3 Cessation of digit sucking usually stops on its own around the time a child begins attending school.
Multiple studies indicate that malocclusion is more likely to develop in children with nonnutritive sucking habits compared to those without a history of nonnutritive sucking habits.1 The duration of the habit also influences the severity of the malocclusion.1 Malocclusion is a developmental disorder of the maxillofacial system resulting from genetic and environmental factors.4 It encompasses several intraoral changes, including anterior open bite, labial flare of maxillary incisors, overjet, spacing of maxillary incisors, and high palatal vault.5
The variables that influence development of malocclusion from nonnutritive sucking habits include the position of the digit, the contractions of orofacial muscles, the position of the mandible while sucking, the facial skeletal structure, as well as the intensity, frequency, and duration of applied force.5 Children with nonnutritive sucking habits are 2.55 times more likely to have malocclusion compared to those who do not have nonnutritive sucking habits.6 Another study noted malocclusion in 54% of individuals with digit sucking as well as 48% of those without the habit.7 This validates the influence of genetics on the development of malocclusion.
It is important to prevent malocclusion in the primary dentition to avoid malocclusion in the permanent dentition.4 Nonnutritive sucking habits should be stopped at an early age before malocclusion has time to develop.2 Irreversible damage occurs to the oral cavity if the habit continues beyond the ages of 3–4 years old.4
Once malocclusion occurs in the permanent dentition, orthodontic treatment is required to correct the malocclusion.1 Knowledge of how the nonnutritive sucking habits contribute to malocclusion may motivate parents to find an intervention.4 Several interventions are described in the literature, but minimal research has been performed to determine the effectiveness of eliminating a nonnutritive sucking habit. Interventions include behavior modification, use of fixed or removable intraoral orthodontic appliances, barrier techniques, and chemical techniques. The focus of this paper is to determine if using conservative intervention techniques found in positive reinforcement is just as successful in discontinuing nonnutritive sucking habits compared to using an orthodontic appliance.
Orthodontic appliances
Orthodontic appliances are used to break nonnutritive sucking habits by preventing the digit from sealing against the palate to eliminate the pleasure associated with the digit sucking habits.2 The appliances are commonly fixed to the molars but may be removable.1 Most are worn for several months to ensure that cessation occurs and prevent reoccurrence of the habit. These appliances may include a palatal bar, palatal arch, palatal crib, hay-rake, bluegrass, or quad helix.5
While the outcome of these devices is similar, the mechanism to achieve cessation may vary. The hay-rake may be a fixed or removable appliance intended to punish the child. It has blunt spikes meant to cause discomfort when sucking habits occur.5 It can be used to discourage thumb sucking and tongue thrusting habits.5
Most orthodontic appliances do not cause discomfort, but break the digit seal to prevent pleasure.5 These devices feature orthodontic bands that wrap around the molars and wires that extend to the anterior portion of the palate. Most are similar in appearance. The most detailed devices include the bluegrass and the quad helix. Both of these utilize a stainless-steel wire soldered to molar bands and a roller or acrylic bead directly behind the central incisors.5 The roller or bead spins to distract the individual from nonnutritive sucking.5
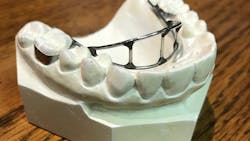
The palatal bar and palatal arch are very simple in construction with a single 0.04–0.03 inch diameter wire extending across the anterior palate but not touching the soft tissues.5 A palatal crib (figure 1) is more complex in design than a palatal bar or palatal arch. It uses a stainless-steel wire with vertical projections like a fence fitted behind the upper incisors, over the palatal rugae.5 It cements onto either the maxillary second primary molars or first permanent molars.1,5 A palatal crib is created by an orthodontist, which necessitates a referral from the general dentist.When used for several months, the palatal crib has been associated with high success rates, resulting in thumb sucking cessation within a week in 80% of cases and little relapse after three years.8 Within three months of wearing the palatal crib, evidence of improvement of the alignment of the teeth will be present, and by six months of wearing it, the anterior open bite will be resolved.8 When the palatal crib is removed after just three months of wearing it, the chances of relapsing the thumb/finger sucking habit are higher than if the appliance is continued to be worn for up to six to 10 months.8 The success rate for cessation of nonnutritive sucking habits with orthodontic appliances compared to no treatment is 46% to 7% respectively.1
There are disadvantages of these appliances as well. Depending upon the age of the child, the appliance may create emotional upset until adjustment occurs.5 Other complications include a temporary change in speech and difficulty in eating.2,5 Fixed appliances may be difficult to brush around, thereby increasing the risk for gingival inflammation and decalcification of enamel.2,5
Positive reinforcement
Positive reinforcement is a psychological intervention aimed to modify behavior through encouragement and reinforcement.1 Methods for positive reinforcement include verbal praise and providing rewards when the child meets the expectation.9 In one study with psychological interventions, the parents were instructed to praise the child when sucking was absent, provide pleasant treats and surprises when sucking was absent for an extended period, and stop television or bedtime stories when sucking occurred.1 It is important to gear the rewards and explanations to the age of the child when using positive reinforcement.1 Children tend to expend more effort if the reinforcement is preferred, so parents should thoughtfully select an appropriate reward.9 Reinforcement should be provided immediately following the desired behavior to encourage compliance.9 Providing too much positive reinforcement should be avoided as it may decrease the value of the reinforcement. Therefore, it is important that the parent remains consistent.9 The opposite intervention is negative reinforcement. This method encourages the parent to discuss the negative outcomes from nonnutritive sucking with the child to generate interest in cessation.1
Cessation of nonnutritive sucking occurs after the child abstains from the habit for three months. Therefore, parents’ involvement should include using a calendar system to track the children’s progress with the use of a rewards system.8 The success rate of psychological interventions compared to no treatment for the cessation of digit sucking habits in children is 19% to 3% respectively.1 There was a statistically significant difference that was shown in favor of the psychological interventions versus no treatment for long-term cessation.1 No studies compare the significance of positive reinforcement in preventing malocclusion.
Comparison of effectiveness
While no reports are published comparing the success rates of positive reinforcement compared to orthodontic appliances, research on the success rates of each method were compared. Positive reinforcement had a success rate of 19% while orthodontic appliances had a success rate of 46% compared to no intervention at all. Use of an orthodontic appliance reduces malocclusion related to the anterior open bite. Positive reinforcement seems to be effective to help children stop nonnutritive sucking habits, but the evidence for preventing malocclusion is low. Further high-quality clinical trials are required to guide decision-making for the best method. After reviewing several studies, it appears that any intervention is better than no intervention at all.
Integration into dental hygiene practice
Dental professionals should involve the child in the discussion and the decision of the cessation intervention because success hangs upon the child’s willingness to stop the habit.10 Explore the child’s values and how the child can feel in control. Use encouraging words to stress the importance of stopping the habit.
Parents’ compliance in taking children for routine dental examinations is crucial in successfully breaking nonnutritive sucking habits and preventing malocclusion. A study in China showed that the frequency at which children visited the dental office was correlated with the presence of malocclusion.7 Eighty percent of children who never visited dental clinics had malocclusion compared to 47% of children who visited dental clinics every six months.7 Routine monitoring of primary dentition was associated with a lower incidence of malocclusion, which validates the need for preventive dental visits in children.7
Since positive reinforcement is the cheapest option and noninvasive, it may be the first intervention suggested to the child. If positive reinforcement isn’t effective for the child, or the parent isn’t interested in the intervention, use of an orthodontic appliance can be suggested. Dental professionals should inform the parents that this is the more expensive option as well as more invasive than positive reinforcement.
A referral to an orthodontist is required to pursue an orthodontic appliance. Fixed orthodontic appliances may create difficulties while eating.2 Mentally disabled children may try to remove their fixed orthodontic appliance and also may frequently break it.2 Removable appliances require patient cooperation, which may not be achievable depending upon the age of the child.2 Since removable appliances require patient compliance, this makes it especially difficult for individuals with mental disabilities.2
Parents can also experiment with barrier techniques, such as a brace that straps around the elbow to prevent the thumb from reaching the mouth, or a brace that fits over the wrist and thumb to prevent the thumb from fitting into the mouth. While no studies are in the literature to evaluate the effectiveness of barrier techniques in cessation of nonnutritive sucking habits, these interventions may be explored before more costly interventions are implemented.
Conclusion
Cessation of nonnutritive sucking habits should be discussed when the habit is still present at the age of three to four.4 It is important to encourage parents of young children to schedule routine dental appointments to prevent and detect malocclusion. The chances of developing malocclusion may decrease when parents are properly educated and actively participate in prevention strategies, leading to lower cost for orthodontic treatment, such as braces.
Acknowledgement
The authors would like to express gratitude to Sarah Mullis and Riley Goad for their contributions to reviewing literature and editing in the initial stages of writing.
References
- Borrie FRP, Bearn DR, Innes NPT, et al. Interventions for the cessation of non-nutritive sucking habits in children. Cochrane Database Syst Rev. 2015 Mar 31;(3):1-53. doi:10.1002/14651858.CD008694.pub2.
- Shetty RM, Shetty M, Shetty NS, Deoghare A. Three-alarm system: revisited to treat thumb-sucking habit. Int J Clin Pediatr Dent. 2015 Jan-Apr;8(1):82-86. doi:10.5005/jp-journals-10005-1289.
- Dhull K, Verma T, Dutta B. Prevalence of deleterious oral habits among 3- to 5-year-old preschool children in Bhubaneswar, Odisha, India. Int J Clin Pediatr Dent. 2018 May-Jun;11(3):210-213. doi:10.5005/jp-journals-10005-1513.
- Ling HTB, Sum FHKMH, Zhang L, et al. The association between nutritive, non-nutritive sucking habits and primary dental occlusion. BMC Oral Health. 2018;18(1):1-10. doi:10.1186/s12903-018-0610-7.
- Gairuboyina S, Chandra P, Anandkrishna L, Kamath P, Shetty A, Ramya M. Non-nutritive sucking habits: a review. J Dent Orofac Res. 2014 Jul-Dec;10(2):22-27.
- Lopes GM, Espasa JE, Rodrigues IC, Butini L, Ustrell JM, Boj JR. Non-nutritive sucking habits and their effects on the occlusion in the deciduous dentition in children. Eur J Paediatr Dent. 2016 Dec;17(4):301-306.
- Zhou Z, Liu F, Shen S, et al. Prevalence of and factors affecting malocclusion in primary dentition among children in Xi’an, China. BMC Oral Health. 2016;16(1):91. doi:10.1186/s12903-016-0285-x.
- Silva M, Manton D. Oral habits—Part 1: The dental effects and management of nutritive and non-nutritive sucking. J Dent Child. 2014 Sep-Dec;81(3):133-139.
- Project Ideal. Project Ideal website. http://www.projectidealonline.org/v/positive-reinforcement/. Updated 2013. Accessed October 23, 2018.
- Tanaka O, Oliveira W, Galarza M, Aoki V, Bertaiolli B. Breaking the thumb sucking habit: When compliance is essential. Case Reports Dent. 2016. doi:10.1155/2016/6010615.
Ashley M. Adkisson, BS, RDH, is a 2019 dental hygiene graduate from the University of Southern Indiana.
Emily R. Holt, MHA, RDH, CDA, EFDA, is a clinical associate professor of dental hygiene at the University of Southern Indiana. She has 19 years of experience in clinical practice and serves as an examiner for the Commission on Dental Competency Assessments.