Case #7
A 27-year-old male visited a dental office for a routine checkup. Radiographic examination revealed a well-defined radiolucency in the left mandible.
History
The patient denied any history of pain in the left mandible. When questioned concerning trauma, he denied any history of trauma to the region. The patient appeared to be in a general good state of health with no significant medical history. His dental history included routine restorative treatment.
Examinations
The patient's vital signs were all found to be within normal limits. Extraoral examination of the head and neck region revealed no enlarged or palpable lymph nodes. Intraoral examination revealed no abnormalities present.
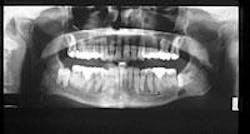
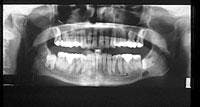
Based on the clinical examination of the patient, selected periapical radiographs, bite wings, and a panoramic film were ordered. A review of the panoramic film revealed an ovoid radiolucency in the left mandible (see radiograph). The radiolucency appeared unilocular with well-defined and corticated borders. The location of the radiolucency was inferior to impacted tooth #17 and above the inferior border of the mandible. No other abnormalities were noted on the panoramic radiograph.
Clinical diagnosis
Based on the clinical and radiographic information available, which one of the following is the most likely diagnosis?
- residual cyst
- radicular cyst
- Stafne defect
- traumatic bone cyst
- dentigerous cyst
Diagnosis
- Stafne defect
Discussion
The Stafne defect (also known as Stafne bone cyst, lingual mandibular salivary gland depression, static bone cyst, or static bone defect) is a developmental concavity found near the third molar or angle area of the mandible. Dr. Edward Stafne first described the defect in 1942 as an asymptomatic radiolucent lesion located near the angle of the mandible.
Located on the lingual surface of the mandible, the Stafne defect is a focal indentation of the cortical bone. This defect is not a cyst (as the terms Stafne bone cyst and static bone cyst imply), but rather a concavity. The concavity may contain salivary gland tissue, a variety of other tissues (for example, muscle, connective tissue, fat, or lymphoid tissue), or maybe devoid of any contents. As the name developmental lingual mandibular salivary gland defect suggests, when the concavity contains salivary gland tissue, it is believed that the concavity is caused by the entrapment of a portion of the submandibular gland during development.
Clinical features
The Stafne defect is asymptomatic and typically discovered during radiographic examination. The Stafne defect is estimated to occur in less than 0.05 percent of radiographic surveys. Males are affected more often than females, with 80 to 90 percent of all cases identified in men.
On a panoramic radiograph, the Stafne defect appears as an ovoid or round radiolucency with well-defined, corticated borders. The size may range from 1 to 2 centimeters in diameter. This defect rarely exhibits a change in size, hence the term "static" in static bone defect or static bone cyst.
The Stafne defect is found on the lingual surface of the mandible between the mandibular canal and inferior border, immediately anterior to the angle of the mandible. In some cases, the inferior border may be interrupted by the defect and present as a notch upon palpation. This defect does not extend above the level of the mandibular canal or contact the apices of the mandibular molars. The Stafne defect most often occurs unilaterally, although it has also been reported to occur bilaterally.
Diagnosis and treatment
The diagnosis of the Stafne defect is made based on the lack of symptoms and radiographic findings. The radiographic appearance and location of the defect are characteristic. A biopsy is not indicated. In cases where a biopsy is performed, normal salivary gland tissue is usually found. Other lesions that may be considered in the differential diagnosis for the Stafne defect include the radicular cyst, the residual cyst, and the traumatic bone cyst. When differentiating between these lesions and the Stafne defect, location is important - these lesions are all located above the mandibular canal.
The Stafne defect requires no treatment. Once the radiographic diagnosis is established, periodic panoramic radiographs is all that is necessary.
Joen Iannucci Haring, DDS, MS, is a professor of clinical dentistry, Section of Primary Care, The Ohio State University College of Dentistry.