Toothpaste allergy
by Nancy Burkhart, RDH, EdD
Presentation: Amy Anderson is your patient today. She is a 34-year-old female who has been seen in your practice for about five years. Amy has had no significant medical history, and she is scheduled every six months for maintenance appointments. Her home-care routine consists of using an electric toothbrush, daily flossing, using a tartar control toothpaste, a non-alcohol mouthrinse, and a tongue cleaner. Her description of her diet leads you to believe that she eats very well and is aware of the relationship between diet and health.
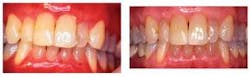
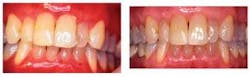
Notes and findings: Extraoral tissues appear within normal limits, although you notice some redness of the lips. Since she just removed her lipstick, you determine that this may just be residue of her lipstick. As you examine the intraoral areas, you find the following (see Figure 1):
Clinical impressions: The tissue exhibits a diffuse red color without ulceration. Consequently, lichen planus, mucous membrane pemphigoid, pemphigus vulgaris, and the usual mucosal disease states are not at the top of your differential diagnosis. The normal color of the vestibular tissues contrasted with the fiery red gingival changes makes you curious about a contact allergy. You suggest that the patient change toothpastes to a bland dental product that does not contain cinnamon. After a two-week period, the gingival lesions subsided and your diagnosis was confirmed.
Diagnosis: Contact stomatitis caused by a reaction to a type of toothpaste containing cinnamic aldehyde.
Etiology: Toothpaste allergy is caused by a sensitivity reaction to an additive or a flavoring agent found in the dental product. Sometimes several products used in combination may elicit an allergic type response.
Method of transmission: Toothpaste allergy is a contact sensitivity reaction and is not transmissible from one person to another. Discontinuing the product or ingredient is usually all that is needed for resolution.
Pathogenesis: Contact stomatitis caused by a toothpaste allergy is due to the sensitivity to an active ingredient in the dental product. Toothpaste allergy is often attributed to the use of cinnamon flavoring agents (cinnamic aldehyde) that have been added to the toothpaste. Cinnamon is from the inner bark of a tropical evergreen tree or bush that grows in wet, warm climates at a low altitude. The bark is cut and dried into rolls or quills. Cinnamon is one of the most aromatic of the spices and has been used since ancient times as a medicinal treatment and as a type of preservative. Its oil, which is a type of phenol, has antifungal and antibacterial properties. Cinnamic aldehyde is the principal component of cinnamon oil, and cinnamic acid is another flavoring agent sometimes used in various products.
The flavor of cinnamon is often used in many current dental products such as toothpaste. Many of the tartar control toothpastes contain tetrasodium or tetrapotassium pyrophosphates that act as an anti-calculus agent. These products have a strong, bitter or salty taste. A flavor enhancer such as cinnamon is often used to make the product more desirable to the consumer. The cinnamon spice is not only used in dental products such as toothpaste and mouthrinse, but is also found in many food products as well. Often the patient is consuming cinnamon without even being aware of doing so. Flavoring agents in general are widely consumed by most individuals through not only dental products, but also mints, gums, salsa products, cola drinks, canned products, and even some cosmetics such as lipsticks and lip balms.
Flavoring agents such as peppermint, wintergreen, and spearmint have been reported to be problematic for some patients. It is thought that the sensitivity may be an accumulation of combined products and the development of a sensitivity over time. Westra et al. (1998) reported a malignancy of the tongue associated with the excessive use of cinnamon gum. Endo and Rees (2006) reported 37 cases of contact stomatitis related to toothpaste and others related to gums and foods. Miller, et al. (1992), recommended that when histopathologic features of hyperkeratosis, chronic lichenoid mucositis with plasmacytic infiltration and marked chronic perivasculitis are viewed microscopically, cinnamon stomatitis should be considered.
Perioral and intraoral characteristics: In the study by Endo and Rees (2006) the most common sites for the contact stomatitis related to toothpaste allergy were lips, gingiva, tongue, and perioral skin. Clinical features included erythema, swelling, desquamation, peeling, epithelial sloughing, and erythema in the buccal mucosa, the tongue, and the gingiva.
Extraoral characteristics: The perioral areas may be affected as well with redness of the lips and peeling of the tissue.
Distinguishing characteristics: Toothpaste allergy may affect any oral tissue, but the gingiva is most commonly affected. This is in contrast to products such as chewing gum that contact the tongue and buccal mucosa. Additionally, a characteristic sign of toothpaste allergy is the normal appearing tissue in the vestibule (see Figure 2).
The toothpaste product does not usually contact this area of the mouth since the tissue is protected by the fold of the lips. The vestibular area can be markedly clear and would appear to indicate a more contact type of reaction rather than a systemic reaction.
Significant microscopic features: Generally, the microscopic features appear as inflammatory in nature with hyperkeratosis, chronic lichenoid mucositis with plasmacytic infiltration, and marked chronic perivasculitis.
Differential diagnosis: Mucosal diseases such as lupus, lichen planus, mucous membrane pemphigoid, pemphigus vulgaris, and candidiasis should be considerations. With any type of a lesion and chronic irritation in the mouth, the clinician should entertain the thought of oral cancer until proven otherwise.
Treatment and prognosis: If your diagnosis is correct, discontinuing the products containing cinnamon will allow the tissue to return to a normal state. The difficulty arises in trying to determine what products the patient is consuming on a daily basis that contain the cinnamon or possibly other additives and/or flavoring agents.
A food diary and careful evaluation are needed. Be sure to check toothpastes to determine whether the product does contain cinnamon. If uncertain, contact the manufacturer. Several brands on the market have been used with success and are reported to be free of cinnamon. As stated previously, the patient may react to several ingredients in dental products. Essentially, the less flavor and additives the dental products contain, the more likely the tissues will respond favorably.
Patch testing for cinnamon sensitivity may also be performed at a facility capable of this type of evaluation. The stomatology center at Baylor has a dermatologist as part of their team for complete evaluations. As the products are discontinued and substituted with those that are free of flavoring agents, the tissue will continue to improve. The Baylor Stomatology Center has found that the optimal time needed to see improvement is two to three weeks. Patients may have slight sensitivity reactions that may go undiagnosed for months to years and may escalate at certain times. As more and more of these types of products become available and are used in combination by the consumer, there is a real possibility that these types of oral reactions are likely to increase in numbers. RDH
Nancy Burkhart RDH, EdD, is an adjunct associate professor in the Department of Periodontics at Baylor College of Dentistry, Texas A & M Health Science Center in Dallas. Nancy is also a co-host of the International Oral Lichen Planus Support Group through Baylor (www.bcd.tamhsc.edu/lichen). She can be contacted at [email protected].
References
Endo H, Rees TD. Clinical features of cinnamon-induced contact stomatitis. Compendium. 20:7, July 2006.
Miller RL, Gould AR, Bernstein ML. Cinnamon-induced stomatitis venenata. Oral Surg Oral Med Oral Pathol 1992;73:708-16.
Westra WH, McMurray JS, Califano J, Flint PW, Corio RL. Squamous cell carcinoma of the tongue associated with cinnamon gum use: a case report. Head and Neck. 20(5): 430-33. 1998.