Clinical Pearls – Coronal Polishing
Lil Caperila, RDH, M.Ed.
Do you polish every tooth as a part of every prophylaxis procedure? Has polishing become an expected part of a patient’s hygiene visit?
The term ‘prophylaxis’ according to the American Dental Association is defined as, “Removal of plaque, calculus and stains from the tooth structures. It is intended to control local irritational factors.”1 The American Academy of Periodontology goes farther and defines how a prophylaxis can be achieved with their definition, “The removal of plaque, calculus, and stains from the exposed and unexposed surfaces of the teeth by scaling and polishing as a preventive measure for the control of local irritational factors.”2
The current position paper from the American Dental Hygienists’ Association on oral prophylaxis states that it should consist of, “supragingival and subgingival (below the gumline) removal of plaque, calculus, and stain.” The paper goes onto to say that “the components of the routine prophylaxis should include but not limited to, patient education, supra- and subgingival scaling, and polishing as appropriate.”3
Coronal or cosmetic polishing - is defined as “a procedure designed to make the tooth free of plaque and extrinsic stains. The process of achieving a smooth, mirror-like enamel or material surface that reflects light and is characterized as having a high luster.”4
Since the late 1970’s, the notion that every tooth during every routine prophylaxis should be polished has been replaced by the selective polishing theory that asserts that it should only be performed on teeth with extrinsic stain.4-6 It has been proven that coronal polishing, when done incorrectly or with an unnecessarily coarse grit paste can damage enamel, dentin, and restorations.7-8 Explanations of why coronal polishing is a seemingly routine of the patient’s “cleaning” appointment may range from patient expectations to oral healthcare provider’s desires to satisfy patients and provide the best care possible.
So, if it is recommended to only polish the teeth with extrinsic stain, and you know that there is a potential for damage to the teeth (e.g., abrasion, loss of enamel, sensitivity), but patients expect it and like the clean smooth feeling it provides, what should a hygienist do?
Below are some recommendations to make coronal polishing more effective and safer:4-6
- 1. Use proper technique to reduce unnecessary abrasion on the exposed enamel and dentin surfaces.
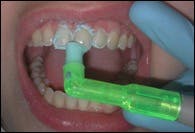
- 2. Correct technique is accomplished by holding the rubber cup at a 90° angle to the tooth surface. With a gentle pressure on the cup, the flare of the cup edge will provide better adaptation at the gingival margins and proximal surfaces.
- 3. Control the time, speed and pressure during the procedure. A moderate speed (1,000–3,000 rpm; see manufacturer’s recommendations) helps reduce abrasion. Limit the time spent polishing each tooth in order to limit heat and excessive removal of tooth structure.
- 4. One grit may not be appropriate for every patient. Select the least abrasive polishing agent that will remove plaque biofilm and stain. Coarse and extra-coarse grits are used commonly for stain removal, but if they are used it is recommended to follow-up with a fine grit. This helps to provide a smoother surface by removing scratches created during stain removal. In most cases, fine and medium grits are appropriate all-purpose choices.
- 5. When polishing a restorative material, care must be taken to use a softer abrasive particle than the restorative material. It may be appropriate to polish restorations with a diamond polishing paste.
To meet the needs of oral healthcare providers and patients, Premier Dental® offers Enamel Pro® Prophy Paste in 10 different flavors with grit sizes ranging from fine to extra coarse. Enamel Pro® paste also features a special formulation to deliver ACP (amorphous calcium phosphate) and is available with and without fluoride.
For questions about Enamel Pro® Prophy Paste and our other hygiene products, please go to www.premusa.com or call 888-773-6872 to speak to a customer service representative.
References and Links:
1. American Dental Association. Glossary of dental clinical and administrative terms. Available at: https://www.ada.org/en/publications/cdt/glossary-of-dental-clinical-and-administrative-ter#o. Accessed July 26, 2018.
2. American Academy of Periodontology. Prophylaxis, oral. Available at: https://members.perio.org/libraries/glossary/entry?GlossaryKey=93c13e7e-5a85-4ca4-b981-7ae22afb61fc&tab=groupdetails. Accessed July 26, 2018.
3. American Dental Hygienist’s Association Position Paper on the Oral Prophylaxis. Approved April 29, 1998. Available at: https://www.adha.org/resourcesdocs/7115_Prophylaxis_Postion_Paper.pdf. Accessed July 26, 2018.
4. Sawai MA, Bhardwaj A, Jafri Z, et al. Tooth polishing: the current status. J Indian Soc Periodontol. 2015 Jul-Aug;19(4):375-80. Available at: https://www.ncbi.nlm.nih.gov/pubmed/26392683. Accessed July 26, 2018.
5. Gutkowski S. Whether they need it… or not! RDH Magazine, November 1, 2001. Available at: https://www.rdhmag.com/articles/print/volume-21/issue-11/feature/whether-they-need-it-or-not.html. Accessed July 26, 2018.
6. Barnes CM. The science of polishing. Dimensions of Dental Hygiene 2009;7(11):18-20, 22. Available at: http://www.dimensionsofdentalhygiene.com/2009/11_November/Features/The_Science_of_Polishing.aspx. Accessed July 26, 2018.
7. CRA Dental Hygiene. Clinicians Report. May 2003.
8. Pence SD, Chambers DA, van Tets IG, et al. Repetitive coronal polishing yields minimal enamel loss. Journal of Dental Hygiene 2011;85(4):348-357. See: https://www.ncbi.nlm.nih.gov/pubmed/?term=22309876. Accessed July 26, 2018.
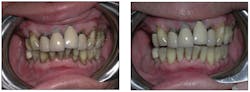
Acknowledgement: Clinical images and case examples courtesy of Dr. Shalom Mehler.
Learn more about Enamel Pro® Prophy Paste at:
https://www.premusa.com/product/hygienepreventative/enamel-pro/