Pernicious Anemia
By Nancy W. Burkhart, BSDH, EDD
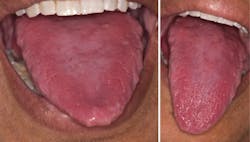
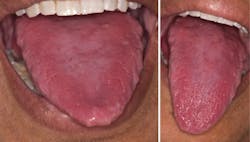
Your patient today is Mary, a 57-year-old African American female. Her chief complaint at the appointment is the red appearance of her tongue. Her family members have commented on the change in color from pink to red, as well as the increased thickness of her tongue (see Figure 1).
As you begin to review Mary's health history, you note that she is postmenopausal, has some food intolerance such as dairy products, she consumes no over-the-counter medications, and has had surgery three years ago for a hiatal hernia. She also states that she sometimes notices a burning sensation on her tongue with various spicy foods and toothpaste.
--------------------------------------------------------------------
Consider reading these articles by Burkhart
--------------------------------------------------------------------
You wonder if Mary could have a toothpaste allergy or possibly an allergic response to a food item. A change in toothpaste, the use of a diet diary, and a careful analysis of lifestyle factors led to no tissue improvement within a two-week period. Mary was sent to her physician for a complete blood analysis and a general physical with an assessment of her chief complaints.
After a full assessment with blood analysis, it was determined that Mary is deficient in vitamin B12 and has developed pernicious anemia. It was determined that she is not producing intrinsic factor (IF). She has a very fissured tongue that makes this appearance somewhat unusual with the combination of fissuring and the red color of her tongue. The red appearance is characteristic of a vitamin B12 deficiency.
What is pernicious anemia?
The general term "anemia" may constitute multiple conditions and is not a single disease. The term refers to the blood having an inadequate number of high functioning normal blood cells but the cause may be from different sources. These blood cells are responsible for cycling oxygen and carbon dioxide between the tissues of the body and the lungs. An abnormal number and size of erythrocytes results in fatigue and general weakness.
The terms megaloblastic and macrocytic anemia involve defective deoxyribonucleic acid (DNA) and ribonucleic acid (RNA) resulting in abnormally large erythrocytes with a shortened lifespan. The erythrocytes appear elongated or oval when compared to normal erythrocytes. The two most common reasons that megaloblastic anemia occurs is because of a vitamin B12 (also called cobalamin) deficiency or a folic acid deficiency.
Pernicious anemia is an autoimmune condition in which the body cannot make healthy red blood cells because it does not have enough vitamin B12. Vitamin B12 is found in food, but is not absorbed properly in some individuals. The usual cause is a failure to produce intrinsic factor (IF), a protein that is made in the stomach or produced in the gastric mucosa. The IF is responsible for the transportation of B12 across the intestinal mucosa. In some individuals, an autoimmune response causes a lack of intrinsic factor. There appears to be a genetic propensity linked to the inability of the stomach to produce IF in pernicious anemia. In this case, the immune system makes antibodies or proteins that attack the individual's tissues.
At one time, before B12 treatments were available, the condition was often fatal; however, vitamin B12 is now available in pills and injections. Other causes of a vitamin B12 deficiency include alcoholism, pancreatic disorders, stomach bypass or stapling, gastrointestinal surgery that removes some of the stomach tissue, and even very strict vegetarian diets. Celiac disease, Crohn's disease, and a lack of hydrochloric acid also affect the absorption of vitamin B12. Women are more affected than men, and 1% of the population over 60 years of age is most affected.
All B vitamins work together to help the body use fats and proteins. They all have a role and the lack of one vitamin will affect the others in different ways. Vitamin B12 and folic acid deficiency must be differentiated since the symptoms may be very similar. Neurological symptoms will prevail if vitamin B12 is not treated properly or mistaken for folic acid deficiency. Pernicious anemia usually occurs in more elderly individuals and in about 20 out of 100,000 individuals.
The symptoms of anemia may include the following:
- Fatigue
- Pale skin
- Arrhythmia
- Constipation
- Weight loss
- Headaches
- Dyspnea
- Tachycardia
- Blotchy skin pigmentation
- Neurological symptoms (paresthesia of the hands and feet)
- Proprioception (the ability of a person to be aware of the position of their body)
- Ataxia (jerky movements)
- Pale oral mucous membranes
- Ulceration of oral tissues
- Smooth, beefy-red tongue with soreness
In regard to the latter, symptoms may mimic burning mouth syndrome and oral candidiasis. Lab analysis will determine vitamin levels and treatment will follow to correct the vitamin deficiency.
The symptoms must be differentiated and determined to be a true vitamin B12 deficiency in order for successful treatment of the patient. If the cause is inadequate intake of the vitamin, the diet will be adjusted. But if the cause is the failure to produce IF factor, lifelong administration of the vitamin may be needed through intramuscular injections.
Certain medications may interfere with vitamin B12 levels in individuals. These include chloramphenicol, proton pump inhibitors, H2 receptor antagonists, and metformin. Many patients are using proton pump inhibitors, and the oral signs of anemia could be observed during an oral exam.
The patient presented in this oral case study also had a fissured tongue, making the classic appearance different from the usual smooth, balding appearance caused by the atrophy of the papillae. The beefy-red color is characteristic of the changes that occur in the surface of the tongue.
The dental professional is in a prime position to identify oral tissue changes that may indicate nutritional deficiencies. Patients may notice tissue changes and ask specific questions related to their overall health that should be addressed by the dentist or hygienist during routine office visits.
As always, listen to your patients and continue to ask good questions!
NANCY W. BURKHART, BSDH, EdD, is an adjunct associate professor in the department of periodontics, Baylor College of Dentistry and the Texas A & M Health Science Center, Dallas. Dr. Burkhart is founder and cohost of the International Oral Lichen Planus Support Group (http://bcdwp.web.tamhsc.edu/iolpdallas/) and coauthor of General and Oral Pathology for the Dental Hygienist. She was a 2006 Crest/ADHA award winner. She is a 2012 Mentor of Distinction through Philips Oral Healthcare and PennWell Corp. Her website for seminars on mucosal diseases, oral cancer, and oral pathology topics is www.nancywburkhart.com.
References
DeLong L, Burkhart NW. General and Oral Pathology for the Dental Hygienist. 2nd edition. Wolters Kluwer-Lippincott, Williams & Wilkins. Baltimore, 2013.National Heart, Lung and Blood Institute. http://www.nhlbi.nih.gov/health/health-topics/topics/prnanmia/
Office of Dietary Supplements: National Institutes of Health
http://ods.od.nih.gov/factsheets/VitaminB12-HealthProfessional/
http://ods.od.nih.gov/factsheets/VitaminB12-QuickFacts/
University of Maryland Medical Center
http://umm.edu/health/medical/reports/articles/anemia