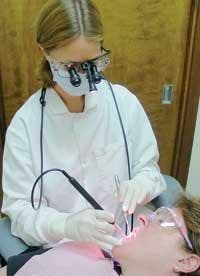
Lighting our world
At 8 p.m. on Wednesday, March 31, 1880, Wabash, Indiana became the first electrically lighted city in the world. Four electrical lamps perched on top of the county courthouse lit up the town square. People were amazed, awed, and overwhelmed by the strange sight.
Nine days later, the Wabash Weekly Plain Dealer reported the city council’s discussion about the new phenomena and the reaction of local citizens. “Everyone admits that Wabash is better lighted than it would be with several hundred gas lamps.” According to a local historian, “The mayor’s wife said they could read the paper on their porch three or four blocks away. One reporter said it was light enough to see the face of his watch when he was on a train three miles out of Wabash.”
Just like the excitement created so many years ago in this forward-thinking little Midwestern town, dental professionals who use auxiliary illumination devices or learn ways to improve existing lighting would never consider providing clinical care using only an overhead dental light.
Proper illumination makes it possible to see the clinical field clearly, assess patient needs, and deliver quality care. Inadequate lighting can lead to eyestrain, postural compromises, missed diagnoses, and poor quality clinical treatment.
Years ago, there was a lively discussion at a CE course about the benefits of wearing an auxiliary headlight to improve illumination. The speaker was discussing how supplemental lighting provides clinicians with a clear view of all posterior teeth. Someone in the audience piped up, “Oh, No. 15 has a distal buccal? I’ve never seen it.” The remark generated lots of laughter but everyone in the room knew how difficult it is to see many areas in the oral cavity by just using illumination provided by the overhead dental light. Quite simply, if you can’t see what you are doing, how can you expect to provide optimal clinical care? Isn’t it our ethical responsibility to examine all areas of our patient’s oral cavity, not just what we can see easily?
There are a number of ways to improve visualization of the entire working field. First, take a good look at your mouth mirrors. Cloudy or scratched mirror surfaces diminish the amount of available reflected light as well as render an unclear image. Worn-out mirrors should be taken out of service in a timely fashion. Instrument clean-up is the perfect time to change the mirror head. One can even swap them in the treatment room with a sterilized replacement head.
Fog forms immediately any time a cold mirror meets a warm, moist environment. A steamy bathroom mirror is a perfect example of this phenomenon. Fogged mirrors reduce the amount of light reflected into the clinical area. Warming a cold mouth mirror under hot tap water prevents this annoyance. Wiping mirror surfaces with mouthwash-dampened gauze or dipping the mirror into a commercial defogging solution prevents fogging and produces a surface free of nagging water droplets.
Foil-covered moisture-absorbing discs that are placed over the Stenson’s duct in the parotid gland increase light reflection in the mouth in addition to preventing salivary contamination during procedures that require a dry field. While reflection from these products may not seem that significant, any improvement in the volume of light will help improve visual acuity as well as make it easier to apply materials like traditional pit and fissure sealants.
The overhead light cover is the next thing to inspect. A sparkling clean cover allows every bit of light to shine on the clinical field. Dust particles and scratches are unsightly and diminish the amount of light by 10 percent or more. Replacing a worn-out cover is an inexpensive way to increase illumination. Some overhead lights have special controls that permit changes in intensity.
Other than the obvious light sources such as the overhead light, ambient lighting, or other light sources in the room, an auxiliary headlight shines additional light directly on to the clinical field. Auxiliary headlight systems, mounted on either the clinician’s magnification loupes or a device-specific headband, have been available for years. Additional illumination is available in a variety of devices such as high-speed handpieces, piezo electric ultrasonic scaler handpieces, magnetostrictive ultrasonic inserts, dental mirrors, and evacuation systems.
All light-powered illumination systems have an energy source. Energy sources, plugged directly into a wall outlet, power some devices. Others use a custom rechargeable battery pack or batteries available at retail outlets. Real-time usage of a battery-powered device is a function of the actual energy demand required to maintain illumination. Less intense illumination can be a result of lower energy requirements; however, battery-powered devices offer significantly more portability than plug-in units offer.
Before purchasing auxiliary lighting, it is smart to understand some basic facts about light technology. Other than the typical overhead dental light, there are three types of light currently used to illuminate the oral cavity: halogen, metal halide, and light emitting diodes (LED). Each lighting system provides additional illumination to the oral cavity; however, there are distinct differences regarding the type and quality of available light.
Today’s popular halogen headlight systems use a fiber-optic cable inserted into a light source to transmit an intense beam of clear light, approximately 2.3 to 5cm in diameter. The color of the light produced by halogen bulbs is similar to that produced in many dental unit overhead lights.
Halogen bulbs emit light as energy passes through a metal filament encased in a gas-filled quartz glass bulb. This modern-day technology uses a filament similar to an incandescent bulb. This allows changes in light intensity, similar to a dimmer switch in a home lighting system. Some units also permit the user to adjust the beam diameter within specified limits. Cordless, battery-operated halogen headlights, developed a number of years ago, did not gain favor because of weight and a diffuse, low intensity beam.
Metal halide units also use a fiber-optic cable to deliver light. These devices create light when energy is applied to a metal filament in a sealed chamber filled with halide gas. Metal halide bulbs create a very white light that has a slight bluish cast and are the brightest dental illumination devices on the market today. Clinicians who are sensitive to bright white lights can reduce the intensity by decreasing the diameter of the beam.
LED technologies, or light emitting diodes, are creating a buzz in the world of lighting technology. LED devices use a blend of small bulbs to create a light spectrum that appears white to the human eye. LED headlight illumination is not as bright as the light produced in halogen or metal halide devices; however, the light beam appears less harsh and more diffuse to some practitioners.
Since LED technology creates very little heat, these lighting systems do not require cooling fans. This makes LED technology particularly appropriate for battery pack-powered portable lighting systems, thus eliminating the need to plug into a conventional light source that is plugged into a wall socket.
Just like any other sophisticated device, it is important to care for headlight systems properly. Nothing is more disconcerting than unexpectedly pulling a light source off the counter or running over the fiber-optic cable with your chair casters. Accidents like this invariably happen exactly at the time when you need the light the most.
Place fiber-optic light sources securely on the counter or house them in a special mounting bracket. Fiber-optic cables contain long, thin glass fibers encased in a sturdy flexible cable. Protect these cables from unnecessary stress. Take care to avoid pinching or bending the cable. Damage from drawers or other types of cable abuse break delicate glass fibers. Treat the cable stem with respect. Be careful when inserting or removing the cable stem from the light source. Store the headlight cable system in a safe place during break times and at the end of the workday.
Over time, both halogen and metal halide bulbs will need replacement. A spare bulb, stored in a handy location, is a clinical and mental lifesaver.
The light from a halogen bulb will begin to dim just before the bulb fails. Halogen bulbs last longer if the light source remains on for the entire day. Turning a unit off and on repeatedly stresses the light filament. Dim the light to its lowest level during nonclinical use. Power surges also shorten bulb life. Plugging the light source into a surge protector prolongs bulb life.
Both halogen and metal halide bulbs generate a lot of heat. Provide adequate ventilation for light sources. A small fan in the light source dissipates heat away from the bulb. Some units have quieter fans than others. Hot bulbs are particularly subject to premature filament failure, so allow sufficient time for adequate cooling before moving a light source or turning the light off at the end of the day.
Periodically inspect the energy source, including the fan blades, for dust. Unplug the unit before cleaning. Removing dust particles with a hand-held vacuum is the most environmentally friendly way to clean a unit. A gentle stream of compressed air also works, but remember to use it outside rather than have contaminated dust particles redistributed in a closed environment. Direct the stream of air so debris gets blown out of the unit.
While actual bulb time varies, most clinicians that practice full time replace the inexpensive halogen bulbs every couple of months. Purchasing 10 or 12 halogen bulbs reduces the overall cost to around $16 per bulb. Metal halide bulbs are longer lasting and more expensive than their halogen counterparts. Over a year’s time, the cost of bulbs for either technology runs about the same.
Make sure the old bulb is cool before replacing a burned-out lamp. Hold the bulb on the outside edges with a clean cloth or wear a pair of gloves when installing a new lamp. Even a small fingerprint on the quartz glass reflector in a halogen lamp will considerably shorten the life span of the bulb. Oils in the skin react with the glass, resulting in a weak area in the bulb. If you accidentally touch the lamp, use alcohol or an alcohol-based window cleaner to clean off the fingerprints.
In addition to headlights, auxiliary fiber-optic lighting is available in many high-speed dental handpieces and several piezo electric ultrasonic scalers. There are now magnetostrictive ultrasonic inserts that have a small LED light that lights up the tip end of the insert. Even though the light in these devices has a preset intensity and beam diameter, having additional light in the exact area is an additional benefit favored by many clinicians.
There are also lightweight, battery-operated, illuminated dental mirrors. One illuminated, cordless mirror uses split-beam illumination technology to light up both sides of the mirror. Another company makes an all-in-one fiber-optic illumination, isolation, and suction device. The intensity of the fiber-optic light can be adjusted in this combination unit.
Follow the manufacturer’s recommended infection control procedures for disinfecting any nonautoclavable illumination devices. Moist disinfecting wipes allow surface disinfection with less chance of damaging delicate electronic and electrical apparatus.
Intensity, color, and type of light are options that require careful consideration before selecting an illumination system. Weight of apparatus, ability to adapt to other systems such as magnification, cost of disposable parts, portability, countertop footprint, warranty, and price of the unit are factors that can influence a purchase decision. Typically, the price of an illumination device is a direct reflection of the quality and durability of a product.
Auxiliary illumination is an important addition to the clinical armamentarium, but like anything else, it is important to understand the differences between technologies and recognize the amazing advances in lighting technology over the last century. Fortunately, today’s dental clinicians have a wide range of choices to illuminate the oral cavity.
Technology is complicated and modern-day living requires tradeoffs. The ability to visualize the oral cavity clearly is not only critical for extending one’s clinical career but is vital to delivering quality clinical treatment.
Wouldn’t you just love to have Thomas Edison in your dental chair today and show him how his patent No. 223898 propelled the modern world to move from gas-lighted illumination to his improved lighting model that revolutionized the incandescent lighting we take for granted every day?
Author’s note: I wish to gratefully acknowledge the assistance of Harold Henson, RDH, MEd, with the preparation of photographs appearing in this article.
According to Lynn R. Owens, former retired division fire chief, the light helped firefighters see their equipment better when they arrived for emergencies in the middle of the night. The bulb has been lighting the firehouse nonstop for 104 years with one exception. A 10-minute interruption in service occurred when it was transferred to its second home in 1976. To date, it has been burning continuously for over 100 years, racking up a total of 911,020 hours.
What is its secret to success? The famous Livermore bulb, constructed with a long, thick carbon element by the Shelby Electric Company, connects to a special unit that eliminates electrical surges. The bulb uses less than four watts of energy, which is the amount of light produced by a handful of fireflies. The light never turns off so the filament is not subjected to repeated power fluctuations that shorten the life of modern-day bulbs. You can visit this amazing little light at www.centenialbulb.org.