On the tip of my tongue: Differential diagnoses for tongue lesions
Why the tongue?
The tongue is hugely important in my life. I have the tendency to link foods I’ve eaten to certain people; for example, my mom and the Venezuelan national dish pabellón criollo, my husband and seafood, and so on. So having something that could disrupt the balance of those memories created through the taste buds is unacceptable; that’s why I make sure to perform a rigorous clinical examination on every one of my patients, because early detection leads to a better prognosis.
Besides collecting the patient’s complete medical history, including any potential carcinogenic habits they may have (e.g., smoking), we need to know that the clinical examination is among the most crucial aspects of patient care. It’s at that moment when we need to emphasize a complete documentation of our findings.1
Several factors, such as a history of allergies, the presence of certain medical conditions, and the use of medications, are associated with an increased probability of tongue lesions.2 It’s up to us to know how to evaluate, manage, and treat patients with alterations in their tongue. We must remember that if the lesion can be attributed to an obvious source (e.g., “I bit my tongue two days ago”), subsequent follow-up is appropriate. However, if there is any doubt regarding the lesion’s etiology or presentation, appropriate referral to an oral pathologist is warranted. We must not feel ashamed if we don’t know the proper terminology when describing or communicating about an oral lesion. Remember, the main goal is our patient’s health. And if we are capable of learning more in the process, good for us.
Remembering some “tongue facts”
The tongue is divided into the oral (presulcal) and pharyngeal (postsulcal) parts by the V-shaped sulcus terminalis. The dorsal epithelium is lined by nonkeratinized, stratified squamous epithelium posteriorly and fully keratinized epithelium anteriorly. The dorsal mucosa is directly attached to the underlying muscle with no interposed submucosa. Lingual papillae are protrusions of dorsal mucosa on the presulcal part of the tongue.
The tongue: A window to other organs
Tongue tie as a missing link to caries management
The taste buds transduce taste stimuli into electrical signals, and then transfer these signals to the sensory nerves. They are innervated by sensory neurons of the VII (facial) and IX (glossopharyngeal) cranial nerves3 and are divided into three groups: fungiform (located in the anterior two-thirds of the tongue), circumvallate (located in the posterior one-third of the tongue), and foliate (located on the lateral sides of the tongue). In a different category are the filiform papillae. These are the nontaste papillae of the tongue and are innervated by the V (trigeminal) cranial nerve.
A healthy tongue will look moist and rough, with its normal tonguelike color. When it’s been affected by something, the tongue may look patchy, fissured, red, or coated. When the tongue is unhealthy, it might present as areas with patches (red, white, or a mix of both) that are ulcerated or swollen.
What if we find something “different”?
We need to ask our patient about it and guide them in their answers. We could ask things like: Do you remember injuring the area? How long has this lesion been present? Does it hurt? Have you noticed any changes in its appearance? Does anyone in your family have something similar? By asking these simple questions, we’ll be able to start categorizing the approach we need to take.
The tricky part
The most difficult part of oral pathology is how to properly classify a lesion. It could be by its etiology, its color, or its appearance, just to name a few examples. What I like to do is to classify every lesion by its etiology, since that gives me a clearer view of the possible differential diagnosis. Overall, there are two main factors—intrinsic and extrinsic—and each one has different etiologies.
Classification of tongue lesions (etiology)
Intrinsic factors
Developmental/congenital
- Genetic
- Acquired
Metabolic
- Hormonal
- Genetically acquired
Nutritional
- Genetically acquired
Immunologic
Inflammatory
- Reactive/allergic
Neoplastic
- Premalignant
- Benign neoplasms
- Malignant neoplasms
Extrinsic factors
Inflammatory
- Trauma
- Physical
- Chemical
Infection
- Bacterial
- Fungal
- Viral
- Parasitic
Iatrogenic
Idiopathic
Fissured, geographic, and hairy
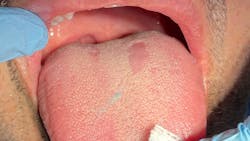
Fissured tongue (figure 1)
Its etiology is unknown, but ill-fitting prostheses, infection, parafunctional habits, allergic reactions, xerostomia, and galvanism are known to be part of this pathology. Also, systemic factors concerned with a burning sensation include medications, anemia, esophageal reflux, deficiency of vitamin B complex, zinc, iron, and psychological factors. Fissured tongue occurs in about 5% of the US population. As people age, this condition is found more commonly, and its severity also increases. Men are affected slightly more than women. It is important to highlight that fissured tongue has been found to be associated with HTA, diabetes, and gastritis.
Clinically, there’s a longitudinal groove on the back of the tongue sometimes associated with lateral furrows, which can be classified according to the number of grooves present: mild (with tongue fissures ranging from one to three), moderate (more than three fissures), and severe (more than 10 fissures).4 No treatment is necessary except to encourage good oral hygiene, including brushing the top surface of the tongue to remove any food debris from the fissures. The differential diagnosis of this pathology includes atrophic glossitis, oral lichenoid drug reaction, lichen planus, oral candidiasis, leukoplakia, and hairy tongue. The prognosis is good.
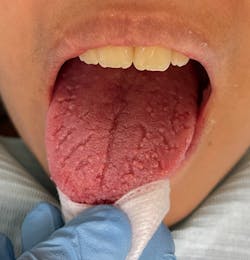
Geographic tongue (figure 2)
The etiology is also unknown. It can also be referred to as benign migratory glossitis, erythema migrans, and a wandering rash of the tongue.5 Psychosomatic and hereditary factors have been suggested to have a role in the etiology of geographic tongue. Redman et al. showed a higher prevalence of geographic tongue in mentally ill patients. Ebrahimi et al. showed that decreasing stress could help heal lesions in geographic tongue, further demonstrating an association between stress and geographic tongue.6
Geographic tongue occurs in up to 3% of the population but generally lacks symptoms, although some people experience food sensitivity or a burning sensation. It has a slightly greater predilection for women in their 20s and 30s. Due to clinical, histopathological, and immunohistochemical similarities between geographic tongue and psoriasis, some experts believe geographic tongue to be an oral manifestation of psoriasis.7,8 Tobacco use has been shown to play a protective role in the pathogenesis of geographic tongue.
The incidence of geographic tongue seems to be less in smokers compared to nonsmokers, possibly due to increased keratinization. Clinically, it is characterized by chronic, recurrent, mostly asymptomatic, migrating, erythematous patches with whitish borders on the lateral and dorsal aspects of the tongue.9 For treatment in patients with symptomatic lesions, topical corticosteroids, antihistamines, cyclosporine, vitamin A, zinc, and acetaminophen, have been shown to be effective. Even though geographic tongue is usually diagnosed by its characteristic history and clinical features, in cases of atypical lesions the differential diagnosis includes erythroplakia, lichen planus, candidiasis, contact stomatitis, leukoplakia, trauma, aphthous ulcer, squamous cell cancer, and plaque psoriasis. The prognosis is good.
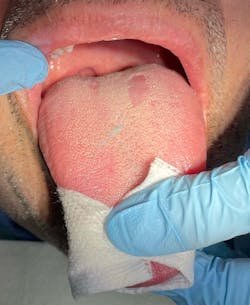
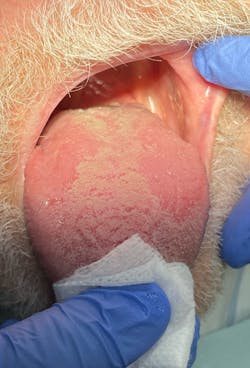
Hairy tongue (figure 3)
This appears when there is a lack of stimulation to the dorsal aspect of the tongue, resulting in a buildup of keratin. Hairy tongue is also associated with the use of medications, extensive use of antibiotics, radiation treatment (in the head and neck area), excessive coffee or tea drinking, or tobacco use. It occurs in about 13% of the population and is more frequent in older patients, although it could appear at any age. It has a predilection for males. Clinically, the tongue surface may be brown, white, green, or pink depending upon the specific cause and other factors. Patients with hairy tongue complain of gagging or a tickling sensation in the soft palate during swallowing. Halitosis may be present due to the taste buds holding on to debris in the mouth.10 Treatment consists of modification of the predisposing factors along with a diet high in probiotics, yogurt, raw veggies, and fruits. The differential diagnosis of this pathology includes acanthosis nigricans, oral hairy leukoplakia, pigmented fungiform papillae of the tongue, and congenital melanocytic nevi/macules. The prognosis is good.
Median rhomboid glossitis
Initially, median rhomboid glossitis was believed to be developmental in origin, but during recent years it has been considered a variant of candidiasis.11 It has a male predilection and occurs in less than 1% of the adult population. Clinically median rhomboid glossitis appears as a red flat or raised nodular area on the dorsum or back of the tongue, where the filiform papillae are missing. Usually, no treatment is required for asymptomatic cases, but in those cases where pain and discomfort are present, antifungal medication is prescribed. The differential diagnosis of this pathology includes erythroplakia, geographic tongue, and granular cell tumor. The prognosis is good, and there are no complications except in cases with discomfort, especially while eating.
Editor’s note: Part two of this article will focus on immunological pathologies.
This article appeared in the January/February 2023 print edition of RDH magazine. Dental hygienists in North America are eligible for a complimentary print subscription. Sign up here.
References
- McKinney R, Olmo H, McGovern B. Benign Chronic White Lesions of the Oral Mucosa. In: StatPearls [Internet]. StatPearls Publishing; 2022.
- González-Alvarez L, García-Pola MJ. Risk factors associated with tongue lesions: a propensity score–matched case–control study. Med Oral Patol Oral Cir Bucal. 2022;27(1):e25-e34. doi:10.4317/medoral.24836
- AlJulaih GH, Lasrado S. Anatomy, Head and Neck, Tongue Taste Buds. In: StatPearls [Internet]. StatPearls Publishing; 2022.
- Sudarshan R, Sree Vijayabala G, Samata Y, Ravikiran A. Newer classification system for fissured tongue: an epidemiological approach. J Trop Med. 2015;2015:262079. doi:10.1155/2015/262079
- Shareef S, Ettefagh L. Geographic Tongue. 2021 Aug 3. In: StatPearls [Internet]. StatPearls Publishing; 2022.
- Redman RS, Vance FL, Gorlin RJ, Peagler FD, Meskin LH. Psychological component in the etiology of geographic tongue. J Dent Res. 1966;45(5):1403-1408. doi:10.1177/00220345660450052301
- Nandini DB, Bhavana SB, Deepak BS, Ashwini R. Paediatric geographic tongue: a case report, review and recent updates. J Clin Diagn Res. 2016;10(2):ZE05-ZE09. doi:10.7860/JCDR/2016/16452.7191
- Monshi B, Grabovac S, Gulz L, et al. Psoriasis is associated with fissured tongue but not geographic tongue: a prospective, cross-sectional, case-control study. J Dtsch Dermatol Ges. 2021;19(8):1170-1176. doi:10.1111/ddg.14451
- Assimakopoulos D, Patrikakos G, Fotika C, Elisaf M. Benign migratory glossitis or geographic tongue: an enigmatic oral lesion. Am J Med. 2002;113(9):751-755. doi:10.1016/s0002-9343(02)01379-7
- Gurvits GE, Tan A. Black hairy tongue syndrome. World J Gastroenterol. 2014;20(31):10845-10850. doi:10.3748/wjg.v20.i31.10845
- Panta P, Erugula SR. Median rhomboid glossitis–developmental or candidal? Pan Afr Med J. 2015;21:221. doi:10.11604/pamj.2015.21.221.5733
About the Author

Andreina Sucre, MSc, RDH
Andreina Sucre, MSc, RDH, is an international dentist, oral pathology, and oral surgery specialist practicing dental hygiene in Miami, Florida. A passionate advocate for early pathological diagnosis, she empowers colleagues through lectures focused on oral pathologies. Andreina is the founder of The Patho RDH, a published author for RDH magazine, and a selected speaker at RDH Under One Roof 2026. Committed to community outreach, she educates non-native English-speaking children on oral health and actively volunteers in dental initiatives.