On the tip of my tongue: Differential diagnoses for tongue lesions (part two)
The first part of "On the tip of my tongue" reviewed the anatomy of the tongue: fissured tongue, geographic tongue, hairy tongue, and median rhomboid glossitis. In this segment, we’ll look at three immunological pathologies of the tongue: aphthous stomatitis, oral lichen planus, and pemphigus vulgaris.
Immunological pathologies of the tongue
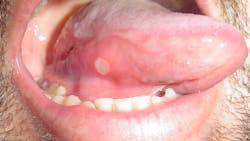
Aphthous stomatitis (figure 1)
The etiology of aphthous stomatitis is idiopathic and multifactorial, but it likely involves activation of the cell-mediated immune system. This pathology affects about 20% of the population, with a prevalence among younger women in their 20s and 30s. These symptomatic lesions may be triggered by local trauma, emotional or physiological stress, allergy or sensitivity (such as to sodium lauryl sulfate in toothpaste, cinnamon, cheese, citrus, etc.), hormonal changes, or alterations in the oral microbiome.
Clinically, the lesions look well circumscribed with a central necrotic ulcer having gray exudate surrounded by an erythematous halo on the nonkeratinized oral mucosa on the ventral surface of the tongue. They could be classified as minor aphthous ulcerations (less than 1 cm in diameter), round or oval, with yellow or gray pseudomembrane surrounded by an inflammatory red halo. The lesions typically heal within seven to 14 days; major aphthous ulcers are deeper and larger (often 2–3 cm in diameter).
Because the goal is to reduce pain, topical agents such as local anesthetics (benzocaine), coating or occlusive agents (bismuth subsalicylate, sucralfate, 2-octyl cyanoacrylate, and various bioadherent emollient pastes), antiseptics (chlorhexidine gluconate and hydrogen peroxide), and anti-inflammatory agents such as glucocorticosteroids may be used as a treatment.
With these immunological pathologies, the spectrum of differential diagnosis widens, and now we have more serious pathologies to consider such as squamous cell carcinoma, herpes simplex, drug-induced lesions, lupus, and lichen planus. Due to the painful ulcers, dehydration is one of the main complications for this type of lesion. Prognosis is good, and in most cases, a modification of the predisposing factors (stress control) is advised along with the treatment.
Oral lichen planus (OLP)
OLP is a T lymphocyte-mediated, chronic, inflammatory, localized, autoimmune oral mucosal disease1 in which the cytotoxic CD8+ T cells trigger apoptosis of the basal cells of the oral epithelium. OLP affects about 2% of the population, with a prevalence in middle-aged and elderly female patients.
There are six types of OLP: reticular, papular, plaquelike, atrophic/erosive, ulcerative, and bullous types. Two or more types of oral lichen planus can occur simultaneously in a patient, but reticular and erosive are the two types that affect the oral cavity. Clinically, the reticular type may appear as a thickened white lacelike pattern and is painful. The erosive type looks like a flat surface with a raised halo, and it also causes discomfort in the patient.
As a chairside diagnostic aid, direct immunofluorescence (DIF) could help establish the clinical diagnosis. The characteristic DIF finding for OLP lesions is a deposit of fibrinogen in a shaggy pattern at the basement membrane zone in the absence of immunoglobulin and complement.2 For the reticular lesions, if the clinical manifestations are bilateral and symmetric, we may or may not need to confirm the clinical diagnosis with a biopsy. For the erosive lesions, biopsy should always be performed due to the possible dysplastic change this lesion may have.
Because OLP is an immunologically mediated disease, corticosteroids are the drugs of choice for treatment. Lesions will heal within two to three weeks. It is critical to highlight the importance of maintaining good oral hygiene during the course of treatment.
The differential diagnosis for reticular and erosive OLP may include oral leukoplakia and oral erythroleukoplakia, lichenoid reactions, lupus erythematosus, pemphigus, and chronic ulcerative stomatitis.3 Prognosis is good, but fewer than 20% of OLP lesions may regress spontaneously. Symptomatic erosive lesions can be resolved by adequate corticosteroid treatment. However, the lesions usually come back if the patient’s health condition is worse.
Pemphigus vulgaris
Pemphigus is an autoimmune blistering disease and can be classified into six types: pemphigus vulgaris, pemphigus vegetans, pemphigus erythematosus, pemphigus foliaceus, paraneoplastic pemphigus, and IgA pemphigus. Pemphigus vulgaris is the most common variant, showing oral lesions as an initial manifestation in 50% of the cases.4,5 The peak incidence occurs between the fourth and sixth decades of life with a prevalence in women. Clinically, the oral lesions are characterized by blisters that rapidly rupture, resulting in painful erosions. Patients usually note a burning sensation in the area. In about 53% of the cases, patients have initial oral manifestations.
The extent of oral lesions is rated using three grades: grade I (only one site involved), grade II (two sites involved), and grade III (three or more sites involved). In the case of this pathology, the diagnosis is based on three independent sets of criteria: clinical features, histology, and immunological tests. Demonstration of immunoglobulins, especially IgG, and complement in the intercellular space by DIF is a reliable test for pemphigus vulgaris. The treatment plan includes injections of sublesional corticosteroids.
The differential diagnoses may include mucous membrane pemphigoid, bullous lichen planus, paraneoplastic pemphigus, chronic ulcerative stomatitis, recurrent herpes lesions in immunocompromised patients, and erythema multiforme. In this pathology, the prognosis goes hand in hand with its early diagnosis and treatment since this determines the course of the disease. Early treatment could prevent serious involvement of other mucosal and cutaneous sites and, therefore, a fatal complication.6,7 Because the blisters and patches may become infected, life-threatening problems can arise such as sepsis, weight loss and malnutrition, along with decay and periodontal disease.
The most important thing to remember is that reassurance is key. None of these pathologies are contagious, and at the same time, the patient either thinks it’s something completely normal or feels ashamed of it. We need to highlight the importance of maintaining good oral hygiene while teaching our patients how to document any changes in their appearance.
Editor's note: This article appeared in the March 2023 print edition of RDH magazine. Dental hygienists in North America are eligible for a complimentary print subscription. Sign up here.
References
- Reamy BV, Derby R, Bunt CW. Common tongue conditions in primary care. Am Fam Physician. 2010;81(5):627-634.
- Cheng YSL, Gould A, Kurago Z, Fantasia J, Muller S. Diagnosis of oral lichen planus: a position paper of the American Academy of Oral and Maxillofacial Pathology. Oral Surg Oral Med Oral Pathol Oral Radiol. 2016;122(3):332-354. doi:10.1016/j.oooo.2016.05.004
- Lavanya N, Jayanthi P, Rao UK, Ranganathan K. Oral lichen planus: an update on pathogenesis and treatment. J Oral Maxillofac Pathol. 2011;15(2):127-132. doi:10.4103/0973-029X.84474
- Shamim T, Varghese VI, Shameena PM, Sudha S. Pemphigus vulgaris in oral cavity: clinical analysis of 71 cases. Med Oral Patol Oral Cir Bucal. 2008;13(10):E622-E626.
- Nguyen T, Ahmed AR. Pemphigus vulgaris localized to the tongue. J Dermatol Case Rep. 2014;8(2):55-57. doi:10.3315/jdcr.2014.1173
- Arpita R, Monica A, Venkatesh N, Atul S, Varun M. Oral pemphigus vulgaris: case report. Ethiop J Health Sci. 2015;25(4):367-372.
- Kumar SJ, Anand SPN, Gunasekaran N, Krishnan R. Oral pemphigus vulgaris: a case report with direct immunofluorescence study. J Oral Maxillofac Pathol. 2016;20(3):549. doi:10.4103/0973-029X.190979
About the Author

Andreina Sucre, MSc, RDH
Andreina Sucre, MSc, RDH, is an international dentist, oral pathology, and oral surgery specialist practicing dental hygiene in Miami, Florida. A passionate advocate for early pathological diagnosis, she empowers colleagues through lectures focused on oral pathologies. Andreina is the founder of The Patho RDH, a published author for RDH magazine, and a selected speaker at RDH Under One Roof 2026. Committed to community outreach, she educates non-native English-speaking children on oral health and actively volunteers in dental initiatives.